While originally conceived of as a way to help surgeons with complicated or extremely delicate surgical procedures, doctors are discovering some unexpected benefits from using 3D printed replicas of patients organs for surgical-preplanning for more common surgeries. So much of the surgical techniques that are used today involve surgical pre-planning using MRI or CT data, which provides an image of exactly what the surgeon will be cutting into, especially when the doctor is using laparoscopic or robotic surgical tools. Unfortunately, because that 3D data is presented as a 2D image it isn’t always going to give the doctor the clearest picture. But turning that 3D data into a 3D printable model allows doctors to get a much clearer idea of their patient’s internal anatomy, and make better treatment recommendations.
When 65-year-old Londoner Alexander Spyrou was diagnosed with prostate cancer he was, naturally, terrified. After all, prostate cancer is the second most commonly diagnosed type of cancer found in men, and while it is highly survivable in the US, globally it is the fifth leading cause of cancer-related death in men. But even if you place the fear of mortality aside, prostate cancer can still cause a wide variety of health problems that can lead to erectile dysfunction and even incontinence. But being able to see and touch a 3D printed replica of his prostate not only helped his doctor offer Spyrou more accurate treatment options, but it allowed the eventual surgical procedure to go smoother for the surgeon himself.
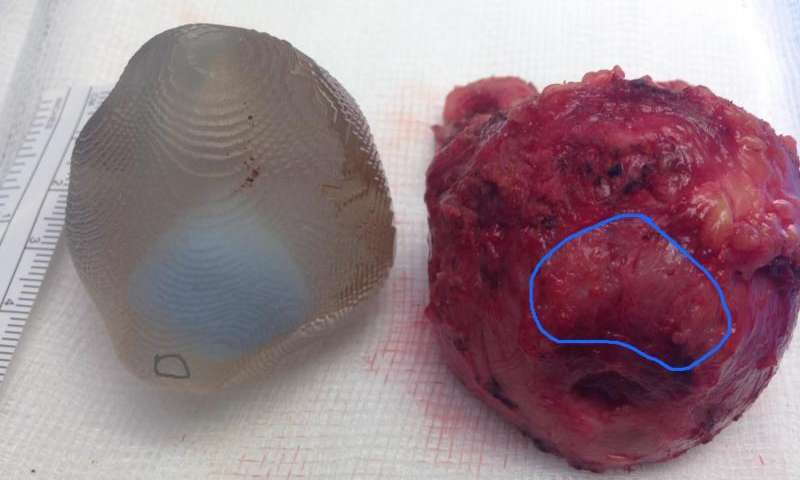
“One of the disadvantages of doing prostate surgery the way I do it, with robotics, is the lack of touch. While you can see things better in 3D, HD, magnified 10x, you lose this crucial sense of touch. In this patient, I could feel the tumor in the 3D model and feel how close the tumor was to the surface. Normally, we plan where the tumor is in our minds but here I held the model in my hand as I performed the procedure with the Da Vinci Robot, where I’m seated remotely at a console. The model allows for better planning and accuracy – which is what you want to hear in cancer surgery,” explained London Clinic’s Professor Prokar Dasgupta, who removed Spyrou’s tumor.
In Spyrou’s case, the surgical procedure to remove the tumor would typically have been considered a risk due to the location of the cancerous growth. The tumor was only a millimeter away from the sphincter muscle, and the slightest error during surgery could have resulted in Spyrou being incontinent for life. On the other side of the tumor was the bundle of nerves that control erections, and any damage to that tissue would result in ED. Typically cases like this would have used radiotherapy to attack and shrink the tumor, however the London Clinic had just started offering 3D technology as a surgical aid, and after discussing the issue with his doctors, and actually feeling where his tumor was on the model, he opted to simply have the tumor removed.
The entire operation took Dasgupta about two hours and involved six tiny incisions in the stomach and groin area that allowed the robotic arms access to Spyrou’s prostate. Dasgupta was able to remove all of the cancerous growth without damaging any of the delicate tissue surrounding it. Once the incisions were closed with staples, it only took about seven days for the holes to heal up. After only a few months of recovery, Spyrou has no loss of function, and is well on the way to a speedy recovery.
“Using this 3D technology here at the London Clinic perfectly demonstrates just how much a multidisciplinary team can achieve. From myself at the diagnostic stage, to Dr Allen in Radiology and Professor Dasgupta as the surgeon, it has brought together all avenues of our expertise and is a truly inspiring achievement,” said Mark Feneley, a consulting urologist at the London Clinic, and the doctor who referred Spyrou to Professor Dasgupta.
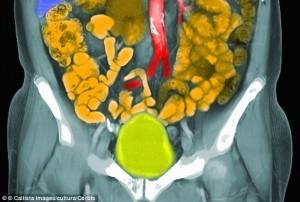
The 3D printed prostate was created Using a process developed by the London Clinic’s radiologist Dr. Clare Allen, who was also consulted by Professor Dasgupta. Dr. Allen started by capturing MRI data of Spyrou’s prostate, and using specialized 3D software she mapped out exactly where the tumor was, then turned it into a 3D printable model. The location of the tumor and accuracy of the 3D printed model was then verified using standard surgical assessments before the actual surgery was conducted. The 3D model was so accurate that Professor Dasgupta was able to hold it in his hand during the actual surgery and could use it as a guide.
Beyond being a useful surgical pre-planning aid, the 3D printed prostate models offer another benefit: the ability to help patients make better choices with their care. By allowing the patients to see and touch the model, they can form a clearer picture of exactly what the surgeon will be doing, and of the severity of the cancer, leading to more use of 3D models for these applications. The model can also help doctors avoid unnecessary treatments for smaller or less serious growths, and can prevent important or dangerous cancers from being missed. This could prevent younger patients from risking ED and incontinence issues on low-risk cancers, and result in fewer medium to high-risk cancers being mistaken for low-risk. Discuss in the 3D Printed Prostate Model forum over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
New Report: Semiconductor Industry to See $1.4B in 3D Printing Revenues by 2032
“The semiconductor sector has become the most strategically significant area of global industry.” Truer words are hard to come by when it comes to the modern world, and they are...
Will Photonic-Crystal Lasers Revolutionize 3D Printing?
Powder bed fusion (PBF) for metals and polymers predominantly utilizes lasers as the primary heat source. Some directed energy deposition (DED) technologies also employ lasers, while various vat polymerization methods...
3D Printing Unpeeled: Orbex Investment, IndoMIM and HP, Ultrasonic Waves
INDO-MIM has bought three HP Metal Jet S100 printers, operating two in India and one in Texas. This is a win for HP because the company has deep experience in...
3D Printing Webinar and Event Roundup: April 21, 2024
It’s another busy week of webinars and events, starting with Hannover Messe in Germany and continuing with Metalcasting Congress, Chinaplas, TechBlick’s Innovation Festival, and more. Stratasys continues its advanced training...