Use your head. It’s a phrase we’ve heard all our lives — and often good advice. Now, scientists are taking this advice quite literally, in 3D printing models of patients’ heads to assist in facial transplants.
Use your head. It’s a phrase we’ve heard all our lives — and often good advice. Now, scientists are taking this advice quite literally, in 3D printing models of patients’ heads to assist in facial transplants.
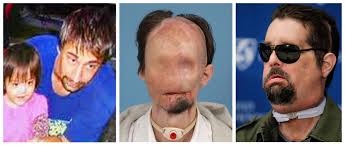
Patients requiring facial transplants all have one thing in common: they have been through extreme trauma with examples such as dog, bear, and chimpanzee maulings; shooting and construction accidents; and fires.
A relatively new surgical procedure that takes as long as 24 hours to complete, only a handful of full facial transplants have been done in the US, with a scattering of them done internationally as well. The first partial facial transplant was completed in 2005 in France, and the surgeries have progressed since then with a number of full — and successful — facial transplants, with one of the most famous in the US being that of the first full face transplant on Dallas Wiens in 2011 at Brigham and Women’s Hospital in Boston.
It’s hard to imagine we are capable of a surgery so intricate, removing what’s left of the face and then replacing it with a new one from a donor. While there are a host of issues to consider, mainly in having to suppress the patient’s immune system and fight infection, most of these surgeries worldwide have been successful.
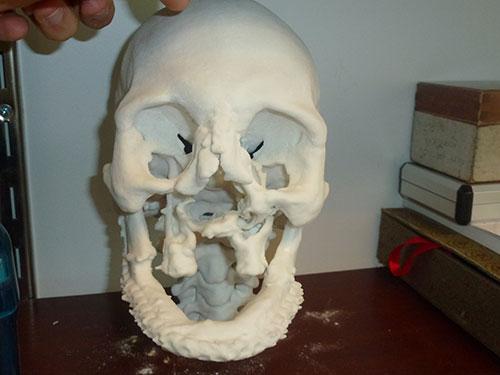
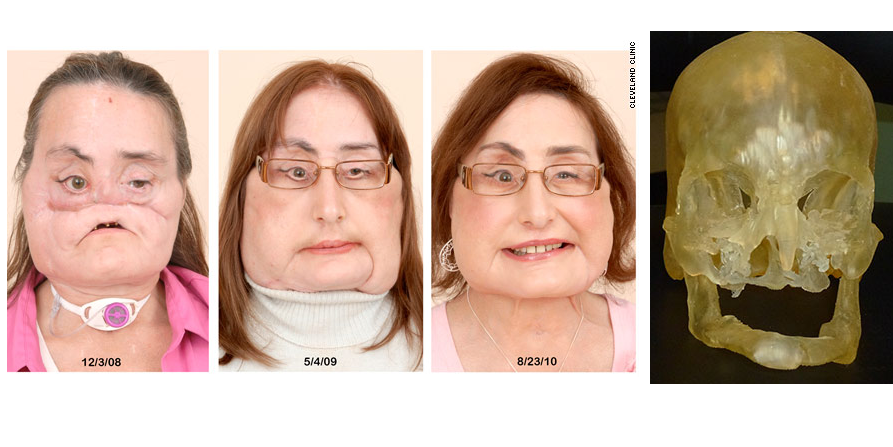
The process is refined with each surgery, though, and with 3D printing technology, surgeons and medical professionals now save time before and during the procedure. They are able to use 3D printed full-size models of the patients’ heads as guides to help with a variety of different issues and concerns during pre-operative planning, as well as ‘onsite’ help during the actual procedure.
Today in Chicago at the annual meeting of the Radiological Society of North America (RSNA) researchers led by Frank J. Rybicki, M.D., radiologist and director of Brigham and Women’s Hospital’s Applied Imaging Science Laboratory, Bohdan Pomahac, M.D., lead face transplantation surgeon, and Amir Imanzadeh, M.D., research fellow, presented a study regarding the use of 3D printed models of transplant recipient’s heads for pre-operative planning.
“This is a complex surgery and its success is dependent on surgical planning,” Dr. Rybicki said. “Our study demonstrated that if you use this model and hold the skull in your hand, there is no better way to plan the procedure.”
The researchers tested the impact of the 3D printed models during planning of surgery on facial transplant recipients. They used CT images of the patients’ heads to create specialized software data for 3D printing of models to assist in the 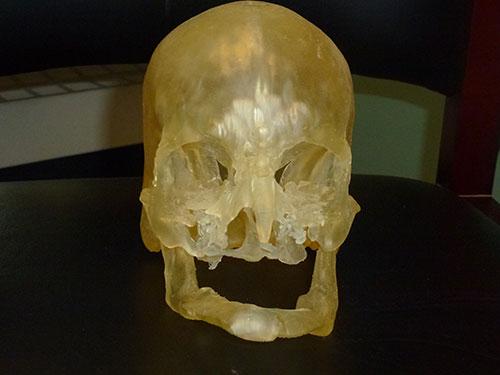 planning and even operative stages of a delicate surgery that involves replacing and making new vascular connections from the donor, which includes stopping flow of blood for up to an hour.
planning and even operative stages of a delicate surgery that involves replacing and making new vascular connections from the donor, which includes stopping flow of blood for up to an hour.
“In some patients, we need to modify the recipient’s facial bones prior to transplantation,” Dr. Imanzadeh said. “The 3D printed model helps us to prepare the facial structures so when the actual transplantation occurs, the surgery goes more smoothly.”
In general life, planning can be everything, so one can only imagine how crucial the pre-operative planning process is in attaching a new face from a donor to the transplant recipient.
“If there are absent or missing bony structures needed for reconstruction, we can make modifications based on the 3D printed model prior to the actual transplantation, instead of taking the time to do alterations during ischemia time,” Dr. Rybicki said. “The 3-D model is important for making the transplant cosmetically appealing.”
Surgeons and radiologists are all in agreement that the 3D printed models afford excellent data for them to study before the procedure occurs, as well as being able to highlight ‘complex anatomy and bony defects’ better, which can be dealt with and discussed before the procedure — rather than during.
“Less time spent in the operating room is better for overall patient outcomes,” Dr. Pomahac added.
3D printed models have been such a success in use for the transplant procedures that medical professionals will be using them for other complex procedures as well. Use of the 3D printed models for surgical planning for face transplantation procedures at Brigham and Women’s Hospital is now mandatory.
Has your doctor used a 3D printed model to explain a medical procedure to you, or used it in planning a medical procedure for you? How do you think this technology will transform medical procedures? Tell us about it in the 3D Printing and Full Facial Transplants forum at 3DPB.com.
Co-authors on the study presented are Maximilian Kueckelhaus, M.D., Kanako K. Kumamaru, M.D., Ph.D., Nicole Wake, M.S., Dimitris Mitsouras, Ph.D., Elizabeth George, M.D., Gerald T. Grant, D.M.D., M.S., Peter C. Liacouras, Ph.D., and Edward J. Caterson, M.D., Ph.D.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
New Report: Semiconductor Industry to See $1.4B in 3D Printing Revenues by 2032
“The semiconductor sector has become the most strategically significant area of global industry.” Truer words are hard to come by when it comes to the modern world, and they are...
Will Photonic-Crystal Lasers Revolutionize 3D Printing?
Powder bed fusion (PBF) for metals and polymers predominantly utilizes lasers as the primary heat source. Some directed energy deposition (DED) technologies also employ lasers, while various vat polymerization methods...
3D Printing Unpeeled: Orbex Investment, IndoMIM and HP, Ultrasonic Waves
INDO-MIM has bought three HP Metal Jet S100 printers, operating two in India and one in Texas. This is a win for HP because the company has deep experience in...
3D Printing Webinar and Event Roundup: April 21, 2024
It’s another busy week of webinars and events, starting with Hannover Messe in Germany and continuing with Metalcasting Congress, Chinaplas, TechBlick’s Innovation Festival, and more. Stratasys continues its advanced training...