Researchers Create hChaMP, a Beating Bioprinted Heart Pump
Through the creation of a new bioink, researchers at the University of Minnesota (UMN) were able to bioprint a functioning centimeter-scale heart pump with real human cells. The custom, extracellular matrix (ECM)-based material enabled stem cells to proliferate before differentiation, allowing the team to create a beating muscle pump with high wall thickness and cell density similar to that of native cardiac tissue. The findings could have far-reaching implications for in vitro cardiology assays, disease modeling, medical device testing, and regenerative medicine research for a wide range of heart conditions. 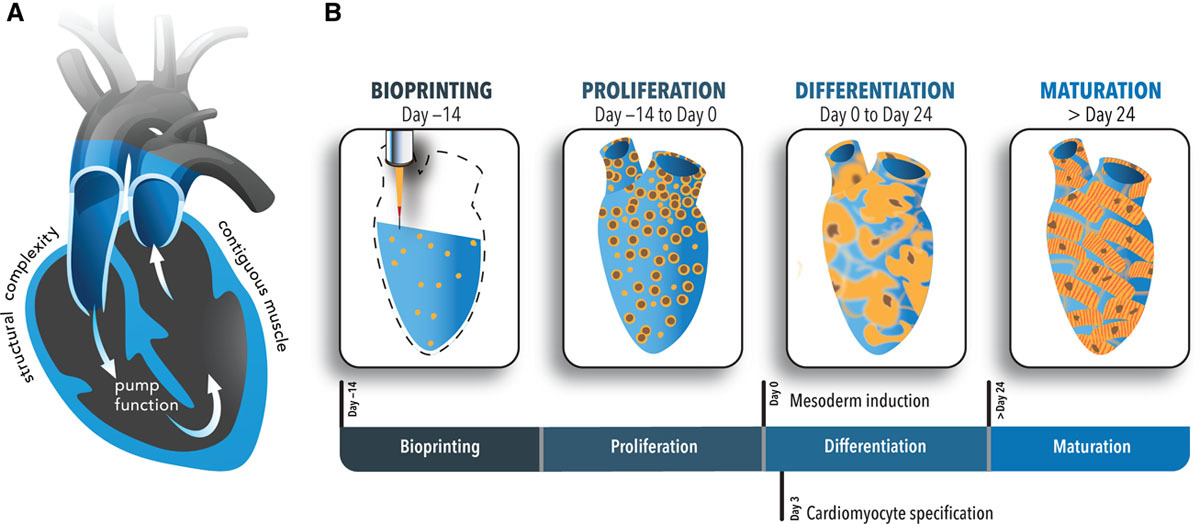
(Image courtesy of University of Minnesota/Circulation Research)
Numerous scientists have tried to 3D print cardiomyocytes derived from human pluripotent stem cells (hiPSCs) to generate cardiac tissues in vitro. But mimicking the cell density of native heart muscle cells, as well as the mechanical properties needed for functioning, remained ultimate challenges. To overcome this hurdle and achieve thick layers of contiguous muscle, the authors created a custom bioink formulation that allowed cells to form robust connections to each other as they differentiate. The results of the study, published in the American Heart Association‘s Circulation Research journal, showed a contracting human chambered muscle pump (hChaMP) capable of beating for at least six weeks, able to mimic the chambers and large vessel conduits of a native heart while housing viable, densely packed, and functional cardiomyocytes.
“At first, we tried 3D printing cardiomyocytes, and we failed, too,” said Brenda Ogle, the lead researcher of the study and head of the Department of Biomedical Engineering at the UMN’s College of Science and Engineering. “So with our team’s expertise in stem cell research and 3D printing, we decided to try a new approach. We optimized the specialized ink made from extracellular matrix proteins, combined the ink with human stem cells, and used the ink-plus-cells to 3D print the chambered structure. The stem cells were expanded to high cell densities in the structure first, and then we differentiated them to the heart muscle cells.”
After years of research, Ogle and her team were ready to give up when two biomedical engineering doctoral students, Molly Kupfer and Wei-Han Lin, suggested printing the stem cells first. Ogle decided to give it one last try: “I couldn’t believe it when we looked at the dish in the lab and saw the whole thing contracting spontaneously and synchronously and able to move fluid.” The team found that for the first time they could achieve the goal of high cell density within less than a month to allow the cells to beat together, just like a human heart would.
Ogle also observed that this was a critical advance in heart research because the new study showed how they were able to 3D print heart muscle cells in a way that the cells could organize and work together. Because the cells were differentiating right next to each other, the process was closer to how the stem cells grow in the body and then undergo specification to become heart muscle cells. Compared to other high-profile research in the past, Ogle believed this discovery created a structure that is like a closed sac with a fluid inlet and fluid outlet, where researchers can measure how a heart moves blood within the body, making it an invaluable tool for studying heart function.
“We now have a model to track and trace what is happening at the cell and molecular level in pump structure that begins to approximate the human heart. We can introduce disease and damage into the model and then study the effects of medicines and other therapeutics,” Ogle went on. “All of this seems like a simple concept, but how you achieve this is quite complex. We see the potential and think that our new discovery could have a transformative effect on heart research.”
To produce the final cell-laden bioink, the team of researchers mixed gelatin methacrylate (GelMA) with hiPSCs and ECM proteins critical to support cardiomyocyte differentiation. According to the study, the optimized formulation could be extruded from a needle, but its low viscosity made it challenging to use with standard extrusion methods. Instead, it was 3D printed with Cellink‘s Inkredible bioprinter, and using the Freeform Reversible Embedding of Suspended Hydrogels (FRESH) method, which helped maintain the structure of the printed construct thanks to a gelatin support bath.
Developed by a team of researchers led by biomedical engineer Adam Feinberg, professor at Carnegie Mellon University, the FRESH technique uses a hydrogel as temporary, thermoreversible support that can be washed away after printing. This technique has proved successful at overcoming many challenges associated with existing bioprinting technology and is able to achieve unprecedented resolution and fidelity using soft and living materials.

3D digital models of the human heart template and the printed structure (Image courtesy of University of Minnesota/Circulation Research)
Specifically designed to fit into the abdominal cavity of a mouse for further study, the 1.5 centimeters long 3D printed muscle model had two chambers and a vessel inlet and outlet. After hiPSCs proliferated to a sufficient density, the researchers differentiated the cells within the structure and demonstrated the function of the resultant beating hChaMP. With final cell densities close in magnitude to those of native tissue, the hChaMP is considered by UMN as the first research study to achieve robust electromechanical function in a perfusable, chambered cardiac pump, able to maintain these functions for at least three weeks more than other similar models.
Replication of the geometrically complex heart structure in vitro has the potential to one day replace animal models, as well as advance the field of cardiac tissue engineering, and eventually move into clinical therapy for patients with heart disease, which is responsible for over 17.9 million deaths worldwide every year. The investigators’ novel bioink and in situ differentiation approach were key findings that allowed hChaMP to beat synchronously, build pressure, and move fluid as a living pump would, maintaining the complex geometries of cardiac muscle. In the last decade, numerous projects have been focusing on techniques to recreate human heart structure and function, but there are still many challenges ahead. This new report encompasses a substantive step toward a macroscale chambered model of the human heart, and even though the team is already initiating new studies to improve it, the achievement stands a solid base for future models that could be used as testbeds for a variety of drugs and devices, as well as a model for heart disease.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Amnovis Expands to the US
Belgian firm Amnovis is a scalable partner for orthopedic innovations. From design to production and regulatory, you can rely on them to take your innovation to market. Coupled with deep...
Scaling 3D Printing Takes More Than You Think; HP’s Webinar Looks at Making It Work Long Term
3D printing is no longer new. In fact, most manufacturers already know what it is, where it fits, and what it can do. But knowing the technology and actually scaling...
Astrobotic Tests Rocket Engine Made with Elementum 3D Materials
Astrobotic has completed a series of hot-fire tests for its Chakram rotating detonation rocket engine, with additive manufacturing (AM) playing an important role in how the engine was built. The...
The Additive Chicken Coop, Part I: Million Dollar Petri Dishes
After decades of tinkering with our individual technologies, billions were poured into speculative claims and optimism. Now the attention is gone, and sometimes it can seem like we’re surrounded by...












































