Researchers Develop and Test 3D Printed Simulator for Neuraxial Anesthesia Training To Help Make Your Next Epidural or Surgery Safer
Procedural training for anesthesiology residents typically takes place as a part of patient care – not when the primary objective is actually learning the procedure. This is probably extremely nerve-wracking for both the patient and the student, and while there are commercially available simulators and phantoms for neuraxial (spinal and epidural) anesthesia training, they’re too expensive to implement on a widespread basis.
But a group of researchers from hospitals and universities all over the world has been working to change this, and recently published a paper, titled “Low-cost three-dimensional printed phantom for neuraxial anesthesia training: Development and comparison to a commercial model,” about their work developing an inexpensive, 3D printable neuraxial anesthesia phantom through the use of free/libre/open-source (FLOS) software, and comparing the phantom to a commercially available simulator model.
The paper’s abstract reads, “Neuraxial anesthesia (spinal and epidural anesthesia) procedures have significant learning curves and have been traditionally taught at the bed side, exposing patients to the increased risk associated with procedures done by novices. Simulation based medical education allows trainees to repeatedly practice and hone their skills prior to patient interaction. Wide-spread adoption of simulation-based medical education for procedural teaching has been slow due to the expense and limited variety of commercially available phantoms. Free/Libre/open-source (FLOS) software and desktop 3D printing technologies has enabled the fabrication of low-cost, patient-specific medical phantoms. However, few studies have evaluated the performance of these devices compared to commercially available phantoms. This paper describes the fabrication of a low-cost 3D printed neuraxial phantom based on computed tomorography (CT) scan data, and expert validation data comparing this phantom to a commercially available model.”
The thing that makes simulating neuraxial anesthesia so tricky is that it is based mainly on tactile feedback, supplemented with ultrasound imaging from before the procedure. So any simulators, 3D printed or otherwise, need to be pretty realistic to do any good. The team used data from CT scans to create a 3D model of the lumbar spine, which was then modified, put inside a digitally designed housing unit, and 3D printed out of PLA on a desktop system.

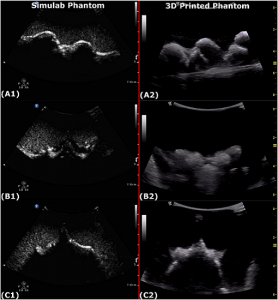
Creating echogenic components of the 3D printed epidural simulator. (A) 3D printed neuraxial phantom with inset showing enlarged view of one interspace. (B) Modeling the ligamentum flavum with silicone paste with inset showing enlarged view of a single level. (C) Total submersion of spine with echogenic gelatin solution (9.0% w/v).
“Simulation has the potential to improve procedural training by allowing trainees to acquire proficiency in a realistic environment where the only consequence of error is learning,” the researchers wrote. “This allows trainees to become “experienced novices” before clinical procedural practice.”
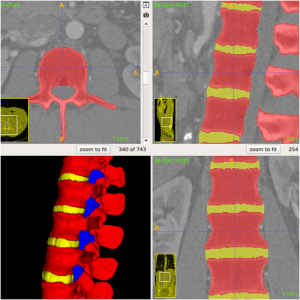
ITK-SNAP interface after segmentation of the spine with the automated active contour tool.
Each colour represents a different layer-mask indicating different regions for the segmented 3D model.
The team filled the model with an echogenic solution of gelatin with psyllium fiber, and once it had been properly heated up and cooled down a few times to increase stiffness, 22 staff anesthesiologists performed a spinal procedure and an epidural, first on the 3D printed simulator and then on a commercially available Simulab phantom, then evaluated the tactile and ultrasound imaging fidelity of each.
The researchers concluded, “Low-cost neuraxial phantoms with fidelity comparable to commercial models can be produced using CT data and low-cost infrastructure consisting of FLOS software and desktop 3D printers.”
However, it was noted that the study does have a few limitations, including the fact that the participants could not be blinded due to the obvious differences in appearance between the models. Additionally, only experienced faculty members were able to test the 3D printed simulator, not trainees.
“The 3D printed phantom also had three major limitations,” the researchers wrote. “First, there was a lack of realism in surface palpitation due to the softness of the gelatin solution used. Second, the perishable nature of the gelatin and psyllium media means that a new batch of gelatin would need to be created repeatedly—a time consuming process. Third, needle track marks persisted in the models after use. These issues will likely be addressed by the substitution of a ballistic gel (Clear Ballistics, Fort Smith, AR, USA) in place of gelatin.”
While ultimately, the 3D printed phantom was less realistic than the Simulab phantom to surface palpation because of how fragile the silicone was, it had far better fidelity in terms of dural puncture, ultrasound imaging, and loss of resistance.
In addition, it only cost $13 to 3D print the neuraxial phantom, with 25 hours of non-supervised 3D printing and two hours to assemble it – much less money and cost than it takes to fabricate the Simulab phantom.
Co-authors of the paper are Azad Mashari, Mario Montealegre-Gallegos, Jelliffe Jeganathan, Lu Yeh, Joshua Qua Hiansen, Massimiliano Meineri, Feroze Mahmood, and Robina Matyal.
Discuss this story and other 3D printing topics at 3DPrintBoard.com or share your thoughts below.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
China Becomes Latest Space Power to Demonstrate Metal 3D Printing in Orbit
China has demonstrated metal 3D printing in space as part of its plan to develop manufacturing technologies for future space missions, including Moon construction. The experiment took place aboard the Qingzhou...
AMPulse Asia: APAC 3D Printing Market Roundup
Key Takeaways Coverage window: April 27 to May 10, 2026. Roughly 30 additive manufacturing (AM)-relevant announcements were tracked across eight Asia-Pacific countries. Largest disclosures: Farsoon Technologies (688433.SH) filing a RMB...
3D Printing Financials: Stratasys Bets on Defense and Drones as Printer Sales Slow
Stratasys (Nasdaq: SSYS) started 2026 with lower revenue and a larger loss as customers continued to slow down spending on new 3D printers. Still, the company pointed to stable recurring...
3D Printing Financials: Xometry Surges After Record Quarter and Siemens Deal
Shares of Xometry (Nasdaq: XMTR) surged on Thursday, May 7, after the company reported record first-quarter 2026 results and announced a major partnership with Siemens. The stock climbed as much...