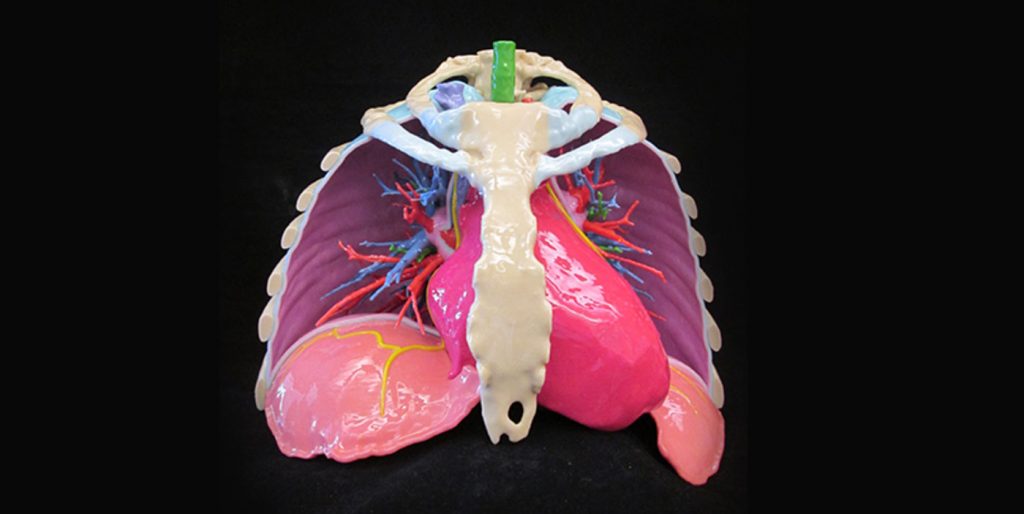
Mayo Clinic Finds 3D Printing Essential Moving Medicine Forward for Complex Surgeries
The Mayo Clinic is probably the single most famous medical facility in the world. It began in 1863 as the medical practice of William Worral Mayo in Rochester, Minnesota and under the direction of his sons William James Mayo and Charles Horace Mayo it became a medical clinic that has since grown to employ nearly 60,000 people in campuses located in Arizona and Florida in addition to the original Rochester location. The clinics see approximately 1.3 million patients each year from over 135 countries around the world and work to address some of the most difficult cases in medicine.
The Mayo Clinic has always been dedicated to understanding the best methods for delivering patient care and, as such, was early to recognize the potential the 3D printing held for the performance of many of these ultra complex surgeries with which its medical staff are confronted. This has been particularly true in the area of 3D printed medical models as was recounted by Dr. Jonathan M. Morris, a neuroradiologist at the clinic, in a keynote speech at the Materialise World Summit. He described the enormous benefits that the production of 3D models has provided to surgical teams as they prepare to perform those complex procedures, as the shift from the unknown to the known. In other words, there were things about the physical circumstances of the procedures that the surgeons could not know before they were in the operating theater, unless they were provided with a 3D model to bring those things from the abstract into the real.
While it is possible to gather more information than ever before through technologies such as CT scans and X-Rays, the act of surgery is one of doing and until the surgeons could hold the models in their hands and examine them real space, there was always a degree of uncertainty and a level of preparation that could not be reached. What Dr. Morris observed when teams were provided with life size, 3D printed models of the area to be addressed was that they almost immediately stopped looking at images, stopped writing on white boards, and gathered around the model to handle and discuss it. This is as close to a practice run as you can get in surgery.
The ability to look directly at the area to be addressed has also been helpful in bridging the disciplinary gaps between groups of surgeons who have to work together during particularly complex procedures. In the case of separating conjoined twins, for example, as many as 60 people might be involved in the procedure, coming from different areas of medicine and speaking in different terminology. The provision of a 3D model provides them with a method for communicating with each other helping them to ensure that they are all coordinated for the enormously complex task ahead of them.
You can see the video of his complete talk, where he discusses cases that he has worked on in which 3D printed models have made an impact and what he has seen to be the benefits of integrating the technology into the regularly performed workflow of surgical preparation.
What do you think of this news? Let us know your thoughts; join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Bambu Lab A1 Used to Directly 3D Print Copper Electroplated Parts
Maker Dzingof was doing tonnes of electroplating of desktop and other 3D prints years ago with his Metalizzr project. I’ve been playing, a lot less successfully, with electroplated 3D prints...
3D Printing News Briefs, October 1, 2025: Bambu Lab Store, Shape-Morphing Materials, & More
In today’s 3D Printing News Briefs, Bambu Lab has opened its first retail store, and Meltio is inaugurating its first international additive manufacturing reference site. A consortium has launched a...
3D Printing News Briefs, August 13, 2025: Public Utility, Rocket Engine, Brains, & More
In today’s 3D Printing News Briefs, AML3D’s large-scale metal 3D printing system is now online at the largest public utility in the U.S. Moving on, Bright Laser Technologies is 3D...
Soft Robotics is Finally Coming Together: Northwestern Researchers Make Strides Towards a Better Actuator
Soft robotics for a long time was a lot of nice videos, papers, and very little in the way of useful technology. It was kind of an engineering Esperanto: a...