3D Printing Aids Intracranial Aneurysm Microsurgery Simulation
No one wants to be operated on by a surgeon who has little hands-on training, but throughout history, finding suitable models or cadavers has been challenging for medical students who want nothing more than the luxury of many quiet hours perfecting their procedures as they continue on their way to being experienced doctors.
3D printing has brought a lot to the (operating) table for doctors worldwide, as well as to patients, their families, and medical students and doctors. 3D printed models and guides, whether displaying organs like the kidney, head and neck tumors, or hip fractures, allow for better diagnosis and treatment, as well as offering a comprehensive visual aid for everyone involved.
Simulation devices, while more complex, are also extremely helpful to students and doctors. Now, Swiss medical researchers from the University of Bern have developed a new training method, detailed in the recently published “Neurosurgical simulator for training aneurysm microsurgery—a user suitability study involving neurosurgeons and residents.”
Currently, training for intracranial aneurysms is limited because of the difficulty level involved in such microsurgery. Medical students and surgeons typically gain experience through watching and assisting during procedures, performing surgery under the watchful eye of skilled doctors, as well as studying videos. While there are some types of virtual reality simulation available, the researchers were motivated to improve on the technology with patient-specific models that even include features like blood circulation and pulsatility–something that is very important for training purposes but historically has been lacking.
Considering the delicate nature of intracranial aneurysm microsurgery, it is critical for students to understand the vascular nature of the aneurysm as well as exactly what happens in the case of a rupture. Students and doctors training should understand the surgical process overall, along with learning how to spot occlusions (blockage). It is concerning that because models and other experiential education are so hard to come by, there may just continue to be a lack of trained cerebrovascular neurosurgeons.
The goal of this study was to create a progressive simulator based on a 3D printed model that would be able to train both residents and neurosurgeons in clipping intracranial aneurysms. The materials used are meant to mimic human tissue, including:
- Arterial wall patency
- Thickness
- Elasticity
- Pulsatile blood flow
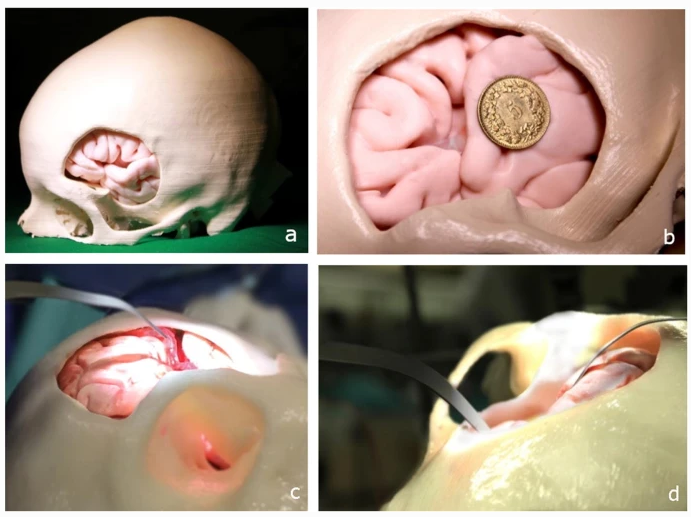
Representation of the model during the training study: a Patient-specific 3D-printed trephined skull with brain model. b MCA aneurysm model located in the left Sylvian fissure. c Pulsating blood vessel and access to the pathology of the model. d Brain retractor during manipulation by resident.
Twenty-five neurosurgeons and residents participated in the research study. Sixteen were in their early residencies with less than four years of training in the field of neurosurgery; nine were in late residencies and already board-certified, with anywhere from four to fifteen years of neurosurgical training. The residents and surgeons evaluated the efficacy of the new simulator, using a five-point scale to grade the following:
- Surgical simulation anatomy
- Realism
- Haptics
- Tactility
- General usage
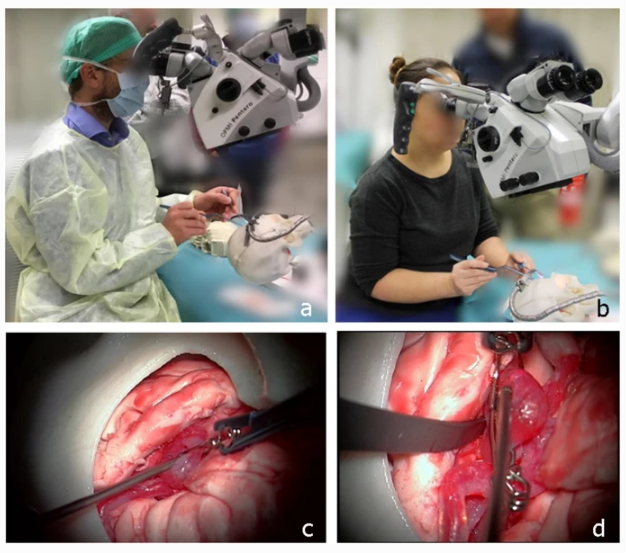
Pictorial representation from the simulator and study participation: a Expert neurovascular surgeon manipulating the aneurysm model in the simulator and trying to clip. b Young resident neurosurgeon clipping. c Attempt to clipping. d Exploration after clipping
In order to evaluate the feasibility of a future validation study on the role of the simulator in neurosurgical postgraduate training, an expert neurosurgeon assessed participants’ clipping performance, and a comparison between groups was done.
See the chart below for results from group A and group B.
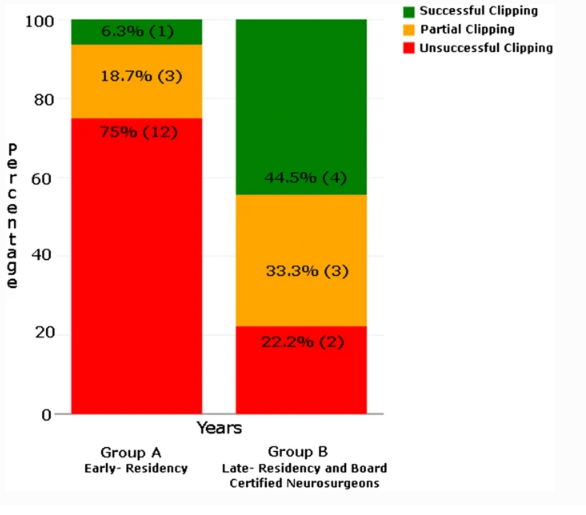
Nature of clipping (successful, unsuccessful, and partially done) vs. years of experience between group A and group B participants.
3D printing, while offering substantial advantages to other industries like aerospace, construction, and energy, has been particularly impressive in changing the face of medicine due to the ability to offer more patient-specific treatment; this study offers good evidence of that in comparison to traditional types of training. Over 80 percent of the participants thought the study “was a good alternative to theoretical and conventional learning.”
[Source / Images: “Neurosurgical simulator for training aneurysm microsurgery—a user suitability study involving neurosurgeons and residents”]“To date, neurosurgeons have been using only one indicator of performance: patient outcomes. Our simulator could incorporate alternative measures to improve and maintain skills,” concluded the researchers.
“Further studies are needed in order to confirm that the present simulator is a valuable clinical tool for measuring, evaluating, and maintaining quality assurance in the training and education of future generations of neurosurgeons.”
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Flashforge Bets on Meshy AI as Desktop 3D Printing Battle Intensifies
Competition in desktop 3D printing is brutal. Whereas before, firms competed through value engineering, Prusa clones now have an integrated hardware, sensor, and software setup that is making all the...
Asia AM Watch: Advantages to the Chinese Way of Doing Business
Timo Göbel, the Head of Additive Manufacturing at the BMW Group, spoke at the AM Forum in Berlin about industrializing additive. He had wise words to share, including that we...
3DPOD 300: Celebrating 300 Episodes with a Look at the Next Year in 3D Printing
In the 300th episode of the 3DPOD, we take a look at what we think will happen over the next 12 months; for instance, what will happen with Bambu’s dominance,...
3D Printing Financials: 3D Systems Returns to Growth in Q1 2026
3D Systems (NYSE: DDD) reported one of its strongest quarters in recent years, showing signs that the company may finally be moving past the tough slowdown that has weighed on...















































