In a pioneering breakthrough in medical science, researchers from Pennsylvania State University (Penn State) have developed a new method for reconstructing damaged skin and tissues in craniomaxillofacial areas, which include the face and skull. This approach, called intraoperative bioprinting, uses a bioprinter during surgery to apply layers of human adipose-derived stem cells (harvested from a patient’s body fat) and extracellular matrix (ECM) directly onto the wound or damaged area. Currently in the pre-clinical stage, this process has shown promise in animal studies for reconstructing complex skin tissues. It aims to seamlessly integrate with existing skin, potentially promoting hair growth and new fat tissue formation.
“Reconstructive surgery to correct trauma to the face or head from injury or disease is usually imperfect, resulting in scarring or permanent hair loss,” said Ibrahim Ozbolat, professor of engineering science and mechanics of biomedical engineering and neurosurgery at Penn State, who led the international collaboration that conducted the work. “With this work, we demonstrate bioprinted, full-thickness skin that can grow hair in rats. That’s a step closer to achieving more natural-looking and aesthetically pleasing head and face reconstruction in humans.”
Intraoperative bioprinting is a groundbreaking frontier in medical science, where 3D printing and cellular biology converge to heal the human body in new ways. Ideally, during surgery, this process would enable the precise application of biocompatible materials, cells, and growth factors directly onto the patient’s injured tissues. By relying on the regenerative capabilities of adipose-derived stem cells extracted from the patient’s own body fat, this technique paves the way for creating diverse cell types and fostering tissue regeneration on demand. This method is a major advance in personalized medicine and could change how we do reconstructive surgery and heal wounds.

Ibrahim T. Ozbolat, associate professor of engineering science and mechanics. Image courtesy of Tyler Henderson/Penn State.
The Penn State team’s work was explained in a March 2024 publication in the journal Bioactive Materials titled “Intraoperative bioprinting of human adipose-derived stem cells and extracellular matrix induces hair follicle-like downgrowths and adipose tissue formation during full-thickness craniomaxillofacial skin reconstruction.”
Central to their study is the custom-designed droplet-based bioprinter produced by MicroFab Technologies, optimized for precision and sterility. According to the paper, this bioprinter was operated within a laminar flow cabinet to ensure a sterile environment for medical applications. The setup included three micro-valve dispensing devices with a removable nozzle, each capable of being individually controlled to dispense specific solutions, facilitating the complex bioprinting process required for this innovative form of tissue engineering. The U.S. Patent and Trademark Office granted the researchers a patent in February for the bioprinting technology developed and used in their research.
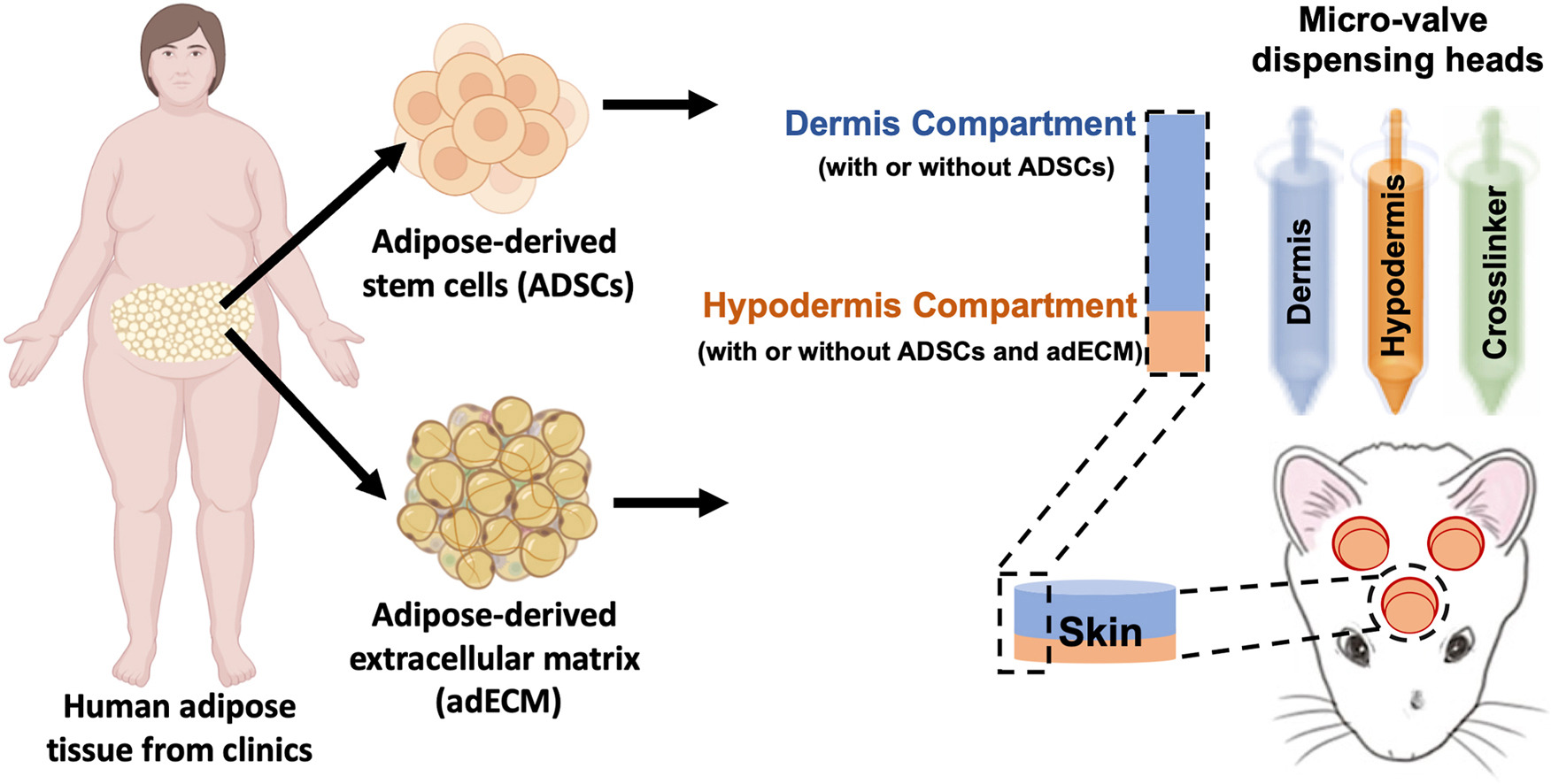
Graphical representation of the Intraoperative bioprinting for full-thickness skin reconstruction. Image courtesy of Penn State University.
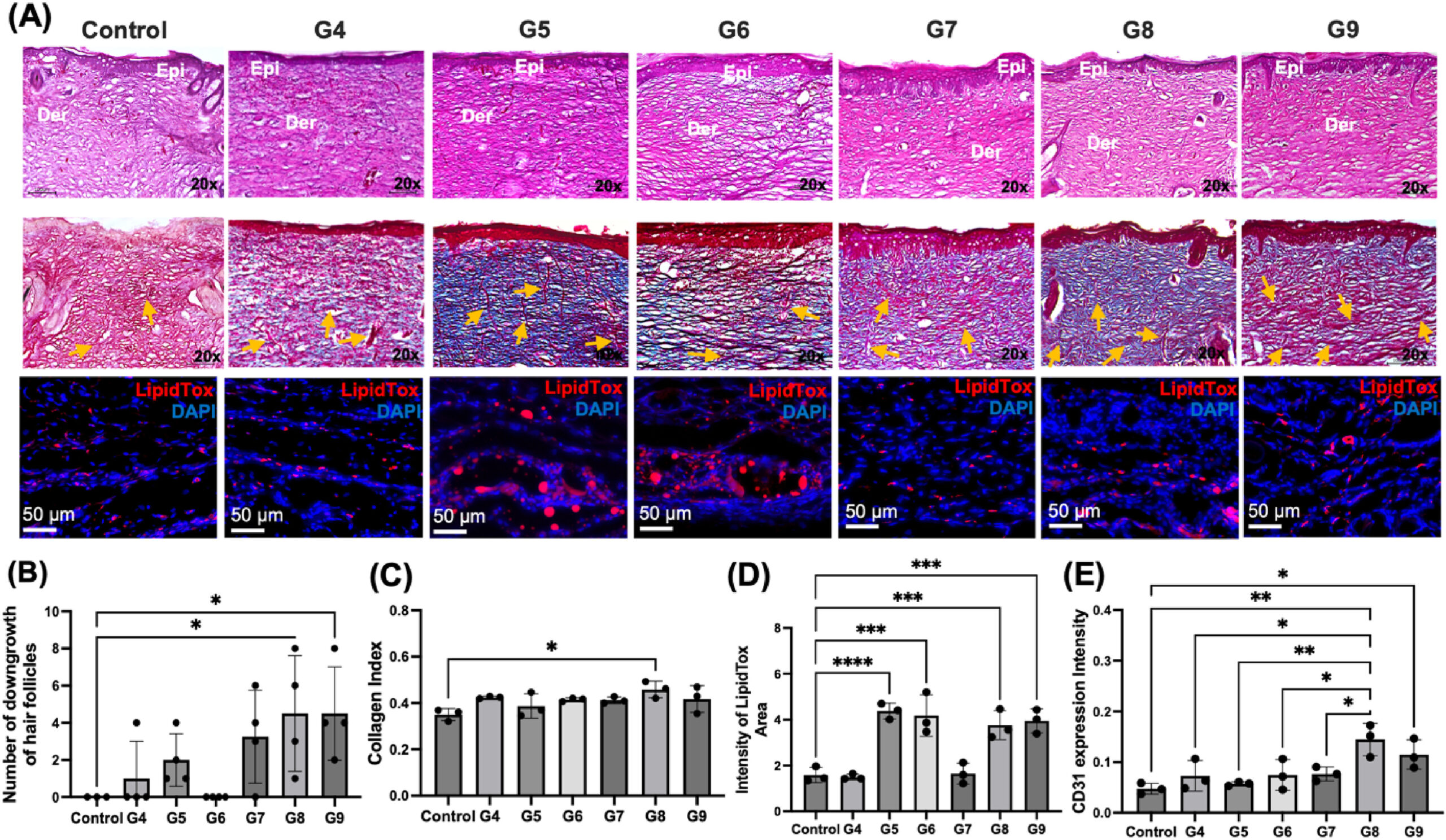
The study conducted by the Penn State team represents a significant stride in the field of regenerative medicine. Their research, primarily conducted on rats, involved the direct bioprinting of skin tissues to repair full-thickness skin defects. This process involves layering human adipose-derived stem cells and ECM to reconstruct the damaged skin, closely mimicking the natural healing process.
For this feat, Ozbolat’s team used their custom bioprinter to deposit these biological materials precisely into the wound site. According to their publication, the experiments showed the successful formation of the skin’s dermal and hypodermal layers, with the outermost epidermis naturally forming over these layers within two weeks post-bioprinting. Although scientists have previously 3D bioprinted thin layers of skin, Ozbolat and his team are the first to intraoperatively print a full, living system of multiple skin layers.
Moreover, the research found that the bioprinted tissues not only facilitated wound closure but also prompted the formation of hair follicle-like structures. This part of the study is exciting as it suggests the possibility of achieving not just “scarless healing” but also the restoration of hair growth on the reconstructed skin, which would represent a key advance for patients suffering from hair loss due to trauma or surgical procedures.
While the study was performed on animal models, the successful demonstration of “hair follicle-like downgrowths” and “adipose tissue formation in bioprinted skin” suggests a promising future for human applications. The researchers believe this technology could eventually be used in dermatology, hair transplant procedures, and extensive reconstructive surgeries, offering more natural-looking and aesthetically pleasing results.
As this research moves closer to human clinical trials, the exciting possibility of using intraoperative bioprinting to transform reconstructive surgery becomes more realistic. It prints living tissue that blends perfectly with the body’s tissues and can even grow hair and fat, marking a huge step forward in medical science.
The Penn State team continues refining this technology, looking to control the density, directionality, and hair growth in the bioprinted tissues. Their ultimate goal is to produce a fully automated bioprinting system that can be used in clinical settings, offering a new era of personalized and regenerative treatment options.
This isn’t science fiction anymore; it’s science fact. The pioneering work, supported by the National Institutes of Health (NIH) and the Scientific and Technological Research Council of Türkiye, opens up new paths in medical research and brings hope to millions of patients worldwide. These patients might soon see more natural and effective ways to heal and reconstruct their bodies after injuries.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Further Understanding of 3D Printing Design at ADDITIV Design World
ADDITIV is back once again! This time, the virtual platform for additive manufacturing will be holding the first-ever edition of ADDITIV Design World on May 23rd from 9:00 AM –...
3D Printer Maker EVO-tech Reborn as NEVO3D — Once More With Feeling
EVO-tech was a 3D printing service and original equipment manufacturer established in 2013 and based in Schörfling am Attersee, Austria. The company produced high-quality material extrusion systems featuring linear bearings,...
3D Systems Brings 3D Printed PEEK Cranial Implant to the U.S. with FDA Clearance
For more than 10 years, 3D Systems (NYSE:DDD) has worked hand-in-hand with surgeons to plan over 150,000 patient-specific cases, and develop more than two million instruments and implants from its...
CDFAM Returns to Berlin for Second Annual Symposium
The second CDFAM Computational Design Symposium is scheduled for May 7-8, 2024, in Berlin, and will convene leading experts in computational design across all scales. Building upon the first event...