Continuing to further the progress between 3D printing and electronics within the medical field, authors Robert Herbert, Saswat Mishra, Hyo-Ryoung Lim, Hyoungsuk Yoo, and Woon-Hong Yeo explore a new method for creating stretchable, wireless electronics for monitoring blood flow to monitor and thus prevent cerebral aneurysms.
Details of their study are outlined in the recently published ‘Fully Printed, Wireless, Stretchable Implantable Biosystem toward Batteryless, Real-Time Monitoring of Cerebral Aneurysm Hemodynamics,’ explaining how their novel, optimized fabrication system allows for multilayer printing of a capacitance flow sensor which can be deployed by a catheter and then inserted into a blood vessel.
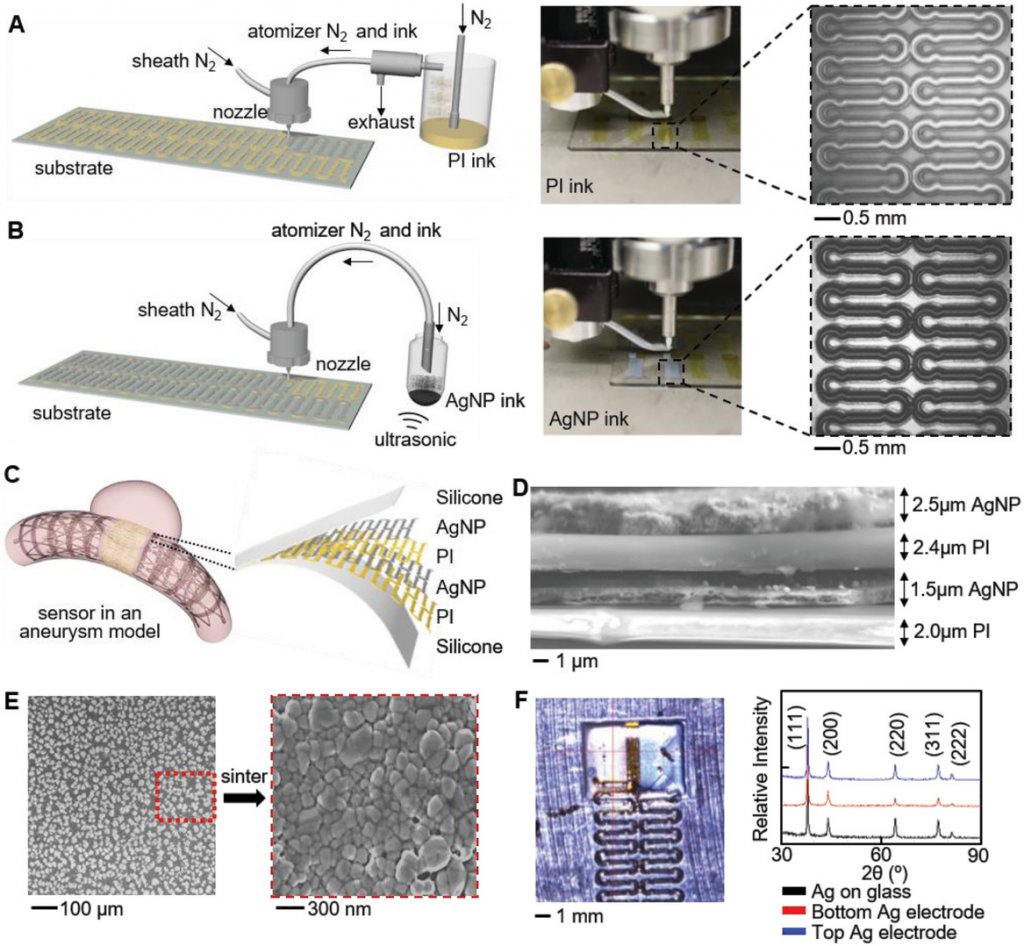
AJP fabrication and material characterization. A) Illustration and image of AJP deposition of PI using a pneumatic atomizer (left). Enlarged view shows a printed PI trace (right). B) Overview of Ag deposition with an ultrasonic atomizer (left) and enlarged view of a patterned Ag on PI (right). C) Illustration of the AJP‐enabled fabrication of an implantable flow sensor in an aneurysm model. Inset shows the multilayered structure of the sensor package. D) Cross‐sectional SEM image displaying multilayered sensor structure. E) SEM images of AgNPs as printed (left) and after a sintering process, showing clusters (right). F) X‐ray diffractometer characterization of a sintered AgNPs on glass slide, bottom Ag electrode on PI, and top Ag electrode on PI. No change in crystalline structure is observed for the three cases.
The scientists point out that microfabrication techniques have allowed for much greater strides in creating miniatured electronics, along with:
- Soft materials
- Stretchable devices
- Biosensors
- Low form factors
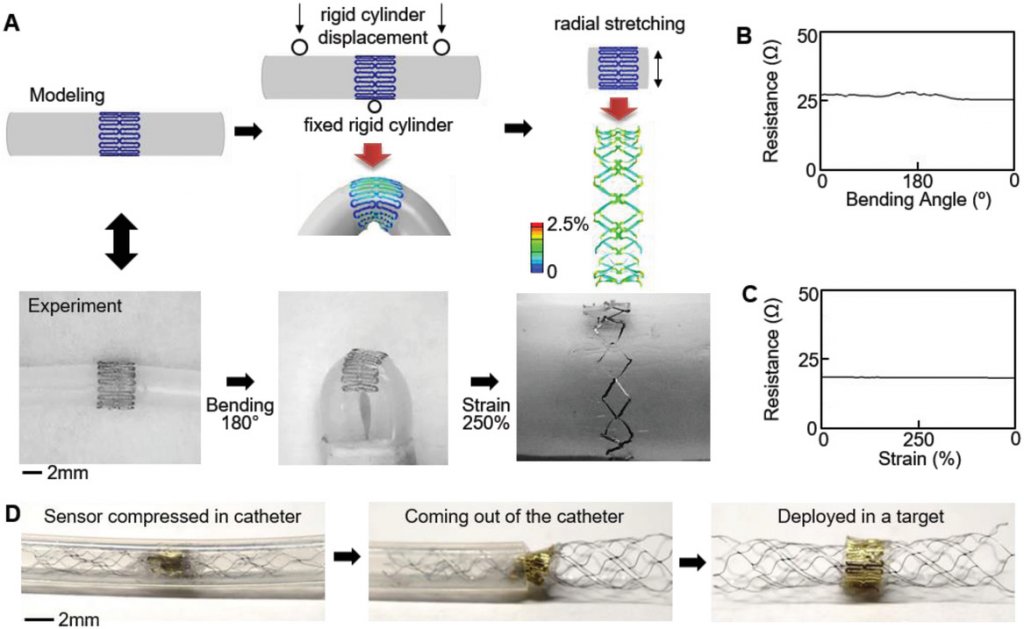
Mechanics modeling, fabrication, and reliability of a printed biosensor for a catheter‐based deployment in a target vessel. A) Design of a highly stretchable sensor via finite element modeling and comparison with the fabricated sensor. B,C) Measured electrical resistance of the printed sensor under a cyclic bending and radial stretching, showing negligible change of resistance under both loading conditions. D) Catheter‐based deployment of the fabricated sensor in a target blood vessel, enabled by the highly flexible and stretchable structure.
Electronic implants, however, may still be inferior in terms of interrogation distances. The authors predict that future devices will be stretchable and wireless—without the rigid components we still see today.
“These rigid components are incompatible with implantation in soft tissues or blood vessels due to mechanical mismatch and bulky packaging,” state the researchers.
Wireless monitoring will depend on further progress with integrating components that are highly conductive. For the prevention of cerebral aneurysms, inserting implants has been challenging historically due to narrow arteries; however, monitoring is critical due to the potential for fatalities upon the rupture of aneurysms.
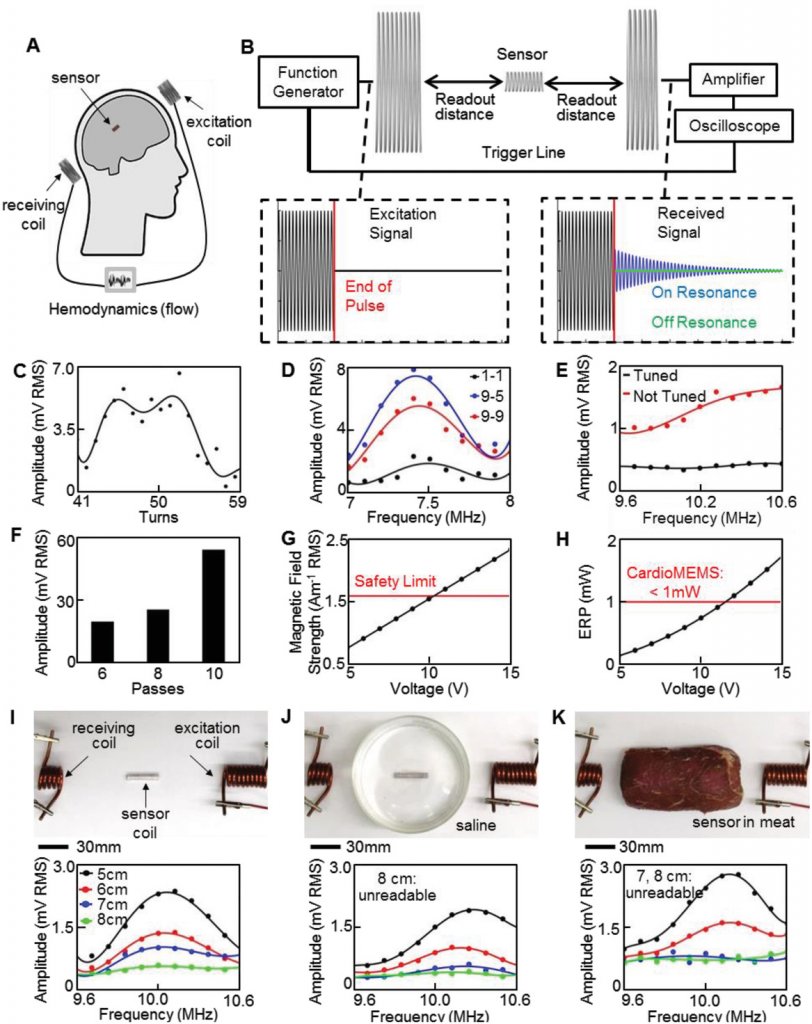
Parametric study and optimization of an inductive coupling method. A) Schematic overview of the batteryless wireless system with an implantable flow sensor and two external antenna coils. B) Equipment overview and example excitation signals. Received transient sensor signals differ for on and off resonance cases. C) Experimental validation of optimal number of sensor coil turns to increase amplitude at resonance. D) Signal amplitude according to the frequency showing the largest resonance with a 9‐turn excitation coil and 5‐turn receiving coil (blue curve). E) Minimized noise due to tuning of antenna coils at the frequency range of interest. F) Signal amplitude showing that sensors with thicker Ag (multiple passes) transmitting a larger resonant peak. G) Comparison of excitation magnetic field strength 1 cm away from excitation coil and averaged over a projected area of 20 × 20 cm2 with safety limit of 1.6 A m−1. H) CardioMEMS HF system operates with an ERP greater than that used in this work with 5 V. I) In vitro test of the sensor coil and ceramic capacitor in different conditions, including frequency sweeps of sensor coil through air, readable up to 8 cm, J) sensor coil readable up to 7 cm when placed in saline solution, and K) sensor coil with the detection range to 6 cm in meat.
Aerosol jet printing has been used to solve traditional challenges in, employing the benefits of 3D printing—from fast production and scalable manufacturing, to ease in design, and better control; however, previous to this study, AJP has not been used in creating such electronics. The researchers state that in this study, they offer the very first demonstration of an AJP‐enabled highly stretchable capacitive system:
“The extremely low‐profile and stretchable structure allows the device to be conformally integrated onto a medical stent and deployed via conventional catheter procedures,” stated the authors. “Utilization of a new inductive coupling method to monitor hemodynamics enables a batteryless, wireless detection of the printed sensors at distances surpassing existing devices.”
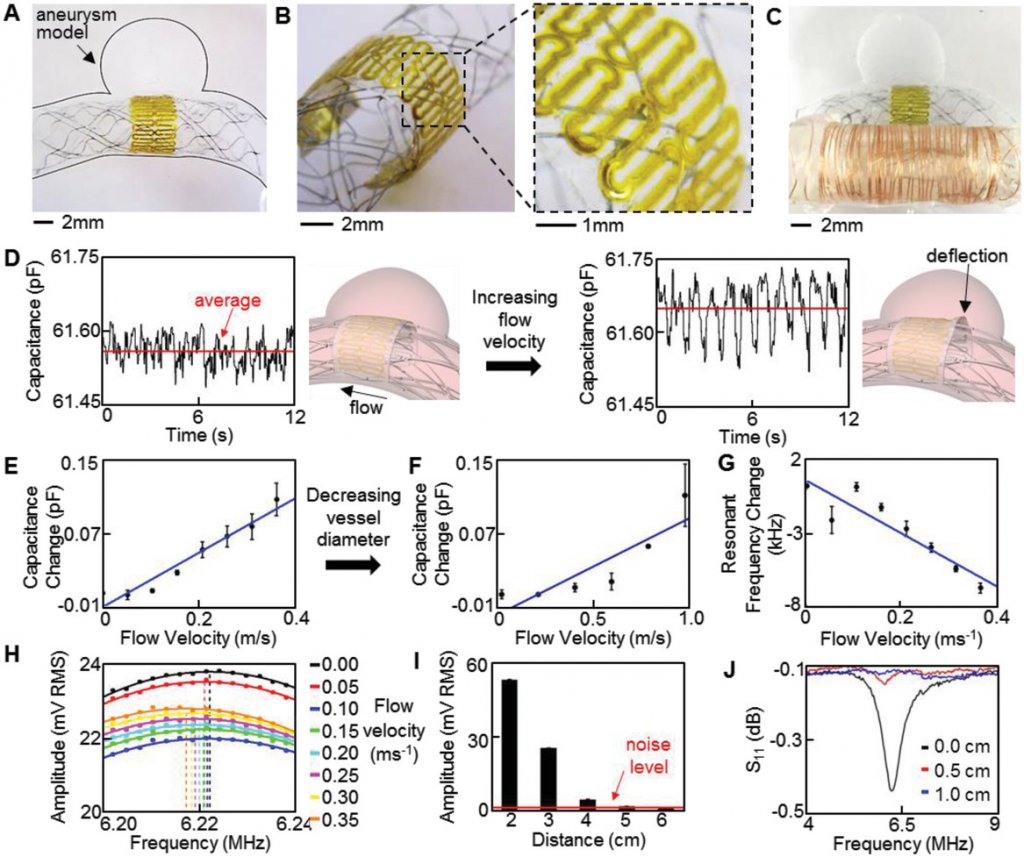
In vitro study of the printed sensor performance in a biomimetic blood vessel model. A–C) Photos of a medical stent‐integrated sensor in an aneurysm model, showing A) a zoomed‐out overview of the sensor, B) tilted, zoomed‐in view of the ultrathin, low‐profile sensor, and C) a copper coil connected sensor for wireless monitoring of hemodynamics in the biomimetic model. D) Pulsatile flow velocity captured by the sensor; average sensor capacitance increases with flow velocities from 0.05 (left) to 0.35 m s−1 (right). Illustration (right) indicates mechanism of capacitance change due to increased flow into aneurysm. E,F) Average capacitance change with the increase of E) flow velocity in the 5 mm vessel and F) higher flow velocities in the 3.5 mm vessel. G) Decreased resonant frequency with increased flow velocity. H) Continuous frequency sweeps, showing the shift in resonant frequency. I) Decreased peak amplitude at resonance with the increased distance; 6 cm interrogation distance is achieved before a resonance peak is not observable. J) Lowered readout distance (less than 1 cm) in monitoring of resonant frequency with a VNA, indicating superiority of the optimized wireless inductive coupling method.
During their research, the authors completed a series of computational calculations to optimize parameters, while in vitro studies offered data regarding performance of the sensor coils in wireless detection. The team used a pulsatile blood pump to test blood flow, with the sensor and stent devices aligned at the opening to allow entrance and exit points through an aneurysm. Ultimately, the results showed ‘feasibility’ for creating ‘high-performance stretchable electronics’ via AJP.
“Overall, this result well agrees with the previous work that related sensor deflection to capacitance change with a computational fluid model. The ultrathin, low‐profile form factor of the sensor avoids disruption to normal hemodynamics,” stated the researchers.
“For wireless monitoring, a copper coil is externally connected to the capacitive sensor. Mean flow velocity in the 5 mm diameter blood vessel is varied from 0 to 0.35 ms−1 at 0.05 ms−1intervals. Initial sensor capacitance is 61.53 pF and increases to 61.63 pF at the maximum flow velocity. This increase in capacitance is a result of flow entering the aneurysm sac and deflecting the sensor.”
Patients today are experiencing a wide range of assistance from medical devices that are 3D printed, from a variety of other monitoring devices and implants too, from cervical implants to spinal implants and even pediatric nasal implants. What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source / Income: ‘Fully Printed, Wireless, Stretchable Implantable Biosystem toward Batteryless, Real-Time Monitoring of Cerebral Aneurysm Hemodynamics’]
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Further Understanding of 3D Printing Design at ADDITIV Design World
ADDITIV is back once again! This time, the virtual platform for additive manufacturing will be holding the first-ever edition of ADDITIV Design World on May 23rd from 9:00 AM –...
3D Printer Maker EVO-tech Reborn as NEVO3D — Once More With Feeling
EVO-tech was a 3D printing service and original equipment manufacturer established in 2013 and based in Schörfling am Attersee, Austria. The company produced high-quality material extrusion systems featuring linear bearings,...
3D Systems Brings 3D Printed PEEK Cranial Implant to the U.S. with FDA Clearance
For more than 10 years, 3D Systems (NYSE:DDD) has worked hand-in-hand with surgeons to plan over 150,000 patient-specific cases, and develop more than two million instruments and implants from its...
CDFAM Returns to Berlin for Second Annual Symposium
The second CDFAM Computational Design Symposium is scheduled for May 7-8, 2024, in Berlin, and will convene leading experts in computational design across all scales. Building upon the first event...































