3D Printing Helps a Five-Year-Old Girl to Dance Again
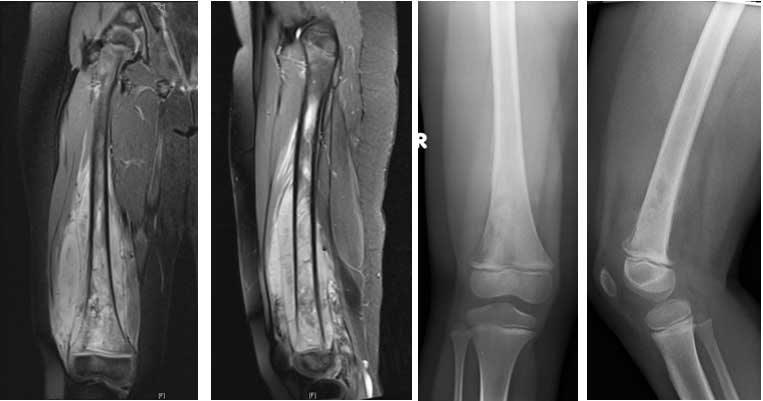
Five-year-old Daria loves dancing, but that was imperiled when she was diagnosed with Ewing’s Sarcoma, a rare malignant bone tumor, in her right leg. The tumor was large, extending almost to her distal femur, so removing it while still allowing her to walk – and dance – normally was a special challenge. Careful planning was required, but thankfully, Daria’s doctors had the tools to do just that.
“With all the soft tissues and skin in the way, what surgeons experience in surgery can be completely different to what they see on a 2D scan,” said Mieke Motmans, Clinical Engineer at Materialise. “Using 3D digital and physical models gives an extra level of information and to work out exactly how best to proceed – it’s like the difference between outlining a journey on a paper map, and using a GPS that tells you exactly where you are going and when you will get there.”
Dr. A.H. Krieg and colleagues at the University Children’s Hospital in Basel, Switzerland had to remove the tumor and reconstruct Daria’s femur using a combination of her own live fibula and a donor bone.
“Endoprostheses (artificial bones) are the usual limb-salvage treatment if the tumor is close to the knee joint or extends to the epiphysis, but this is rarely possible for children as young as Daria – there are high complication rates,” said Dr. Krieg. “Making the reconstruction a success meant using 3D printing to its full potential and working with the right experts.”
Materialise has worked with surgeons to plan for more than 2,000 osteotomy cases, or corrective surgery where a bone is cut to allow realignment. The company has also designed and 3D printed more than 700 custom implants or endoprostheses.
“I’d actually worked with Mieke and her team before, so I knew they could help,” said Dr. Krieg. “The first step was uploading our MRI and CT scans of Daria’s leg to Materialise’s online portal for evaluation.”
Motmans specializes in oncology cases. Her team began by aligning meshes from Daria’s CT and MR scans, checking them in the Materialise Mimics medical imaging processing software and verifying the tumor’s position.
“Finding the tumor outline is where we start,” she said. “Sometimes tumors are only visible in MRI, so Mimics helps us transfer its boundaries to the more accurate CT scans. Then we combine the CT scan ‘slices’ to build the 3D bone geometry model that lets surgeons see the overall picture and zoom in to the detail. Some surgeons have a very clear idea of what they want to do, while others will simply send us the scans and ask us for a solution. Either way, getting to this stage – seeing the 3D model – is often a critical moment. The model’s accuracy lets us verify the planned approach and sometimes it can be very obvious that the initial plan just isn’t going to work.”
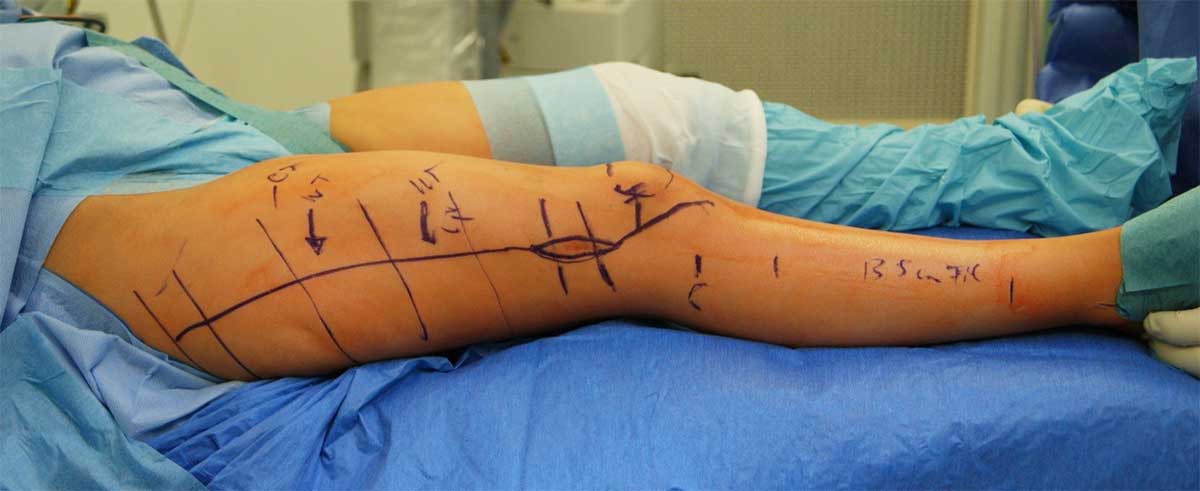
Materialise and the hospital team worked together to map out the surgical procedure and position the resection plains that would be used to show exactly where saw cuts would be needed around the tumor. They had to retain as much bone as possible to keep Daria’s knee joint intact to support the screws for the titanium bridge that would hold the remaining bone, the allograft and fibula as they grew together during osteosynthesis. The margins were tight because the tumor was so big and so close to Daria’s knee.
“Where to cut the tumor influenced the size of the hole, which in turn governed the required shape of the donor bone,” said Motmans. “We couldn’t print anything until the whole planning stage – where to resect the tumor and allograft, the plate size, the position of the screws – was complete.”
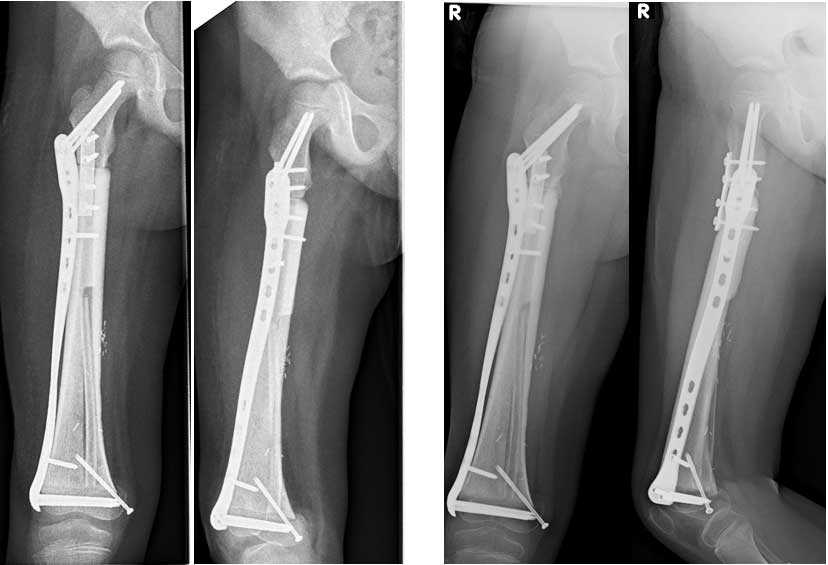
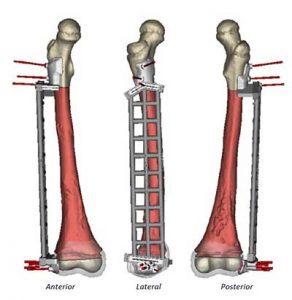 The surgeons had to trim their normal safety margins and sacrifice the lower epiphyseal plate which contains live growing bone tissue, but they were finally able to set their resection planes. Materialise then 3D printed the models and the three cutting guides. Slots in these templates, two for the femur and one for the allograft, would be used to precisely position the surgeon’s saw blade, with carefully positioned holes directing the drill to ensure correct screw positions and insertion angles. The allograft guide defined the channel where the fibula would be inserted. Motmans used models showing pre- and post-operative bone geometry to check that each cutting guide and plate fitted precisely.
The surgeons had to trim their normal safety margins and sacrifice the lower epiphyseal plate which contains live growing bone tissue, but they were finally able to set their resection planes. Materialise then 3D printed the models and the three cutting guides. Slots in these templates, two for the femur and one for the allograft, would be used to precisely position the surgeon’s saw blade, with carefully positioned holes directing the drill to ensure correct screw positions and insertion angles. The allograft guide defined the channel where the fibula would be inserted. Motmans used models showing pre- and post-operative bone geometry to check that each cutting guide and plate fitted precisely.
“The operation lasted ten hours, involved seven surgeons and was a great success,” said Dr. Krieg. “Although Daria still has a long way to go in rehabilitation, she now has the chance to make a nearly full recovery and use her leg without major restrictions.”
“The skilled teams that perform these operations are amazing,” said Motmans. “To be able to help them is a privilege. 3D printing means surgeons can plan ahead, allowing them to deal with problems before they even enter the operating room, and so avoid surprises during surgery. That’s an outcome that’s great for everyone.”
Discuss this and other 3D printing topics at 3DPrintBoard.com or share your thoughts below.
[Source/Images: Materialise]
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
You May Also Like
3D Printing Financials: 3D Systems Looks to Bounce Back in 2025
After a challenging year for the industry, 3D Systems (NYSE: DDD) ended 2024 with results pointing to a reset, laying the groundwork for future profitability. The company didn’t post strong...
Printing Money Episode 27: Q4 2024 Public 3D Printing Earnings Review with Troy Jensen, Cantor Fitzgerald
Q2 2025 has already begun, but public markets reporting has only just finished with Q4 2024. To tie a bow on Q4 2024, we are thankful to have Troy Jensen...
3D Printing News Briefs & Events Roundup: March 15, 2025
In this weekend’s combined 3D Printing News Briefs and Webinars/Events Roundup, we’re covering news about automotive and construction 3D printing, along with AM Forum, TCT Asia, the Experience Stratasys Tour,...
3D Printing Software Market to Hit $6.78B Revenues by 2033
Additive Manufacturing Research (AMR) has released a new edition of its flagship market study, “AM Software Markets 2025: Analysis, Data and Forecast,” offering deep insights into the 3D printing software...