Using Patient-Specific 3D Printed Surgical Guides for Total Knee Replacement
 While surgery has always, ultimately, been about the patient, it hasn’t always been patient-centered. Historically, patients have not had an easy time of understanding exactly what their surgery entails and have often been treated as if they were ancillary to the surgical problem presented. This can’t all be blamed on uncaring medical staff, as most people involved in medicine do care and care profoundly. Instead, it has largely been a result of resources and standing custom. Surgical procedures are complicated and difficult to understand, hence the reason why experts are the ones who address them, and the pressure and stress involved in going into a procedure largely blind has made it difficult for surgeons to relax and broaden their focus to include the patient beyond the problem.
While surgery has always, ultimately, been about the patient, it hasn’t always been patient-centered. Historically, patients have not had an easy time of understanding exactly what their surgery entails and have often been treated as if they were ancillary to the surgical problem presented. This can’t all be blamed on uncaring medical staff, as most people involved in medicine do care and care profoundly. Instead, it has largely been a result of resources and standing custom. Surgical procedures are complicated and difficult to understand, hence the reason why experts are the ones who address them, and the pressure and stress involved in going into a procedure largely blind has made it difficult for surgeons to relax and broaden their focus to include the patient beyond the problem.
3D technology is making great contributions to medicine, from aiding in research to assisting in the preparation of students to practice medicine to producing the tools necessary to perform better operations. It is being integrated into the surgical theater and changing the face of surgery as we know it. One of the ways it is doing this is through the provision of a greatly improved ability to plan for the procedure. 3D technology not only allows the medical team a sneak preview, 3D printing can create models of the particular areas to be addressed and allow surgeons to study them in advance. This helps minimize surprises and therefore reduces the stress on both the patient and the medical staff.
The staff at Orthoparc in the Netherlands has figured out another way to help create and deliver the best in patient centered care. Using 3D technology, they have developed a method of patient-centered total knee replacement that allows a patient to walk in, in the morning, and walk out that same day. Such a possibility requires a highly interconnected team of specialists working together to ensure that not only does the patient get the knee replacement they need, but their psychological, nutritional, and whole health needs are met as well.
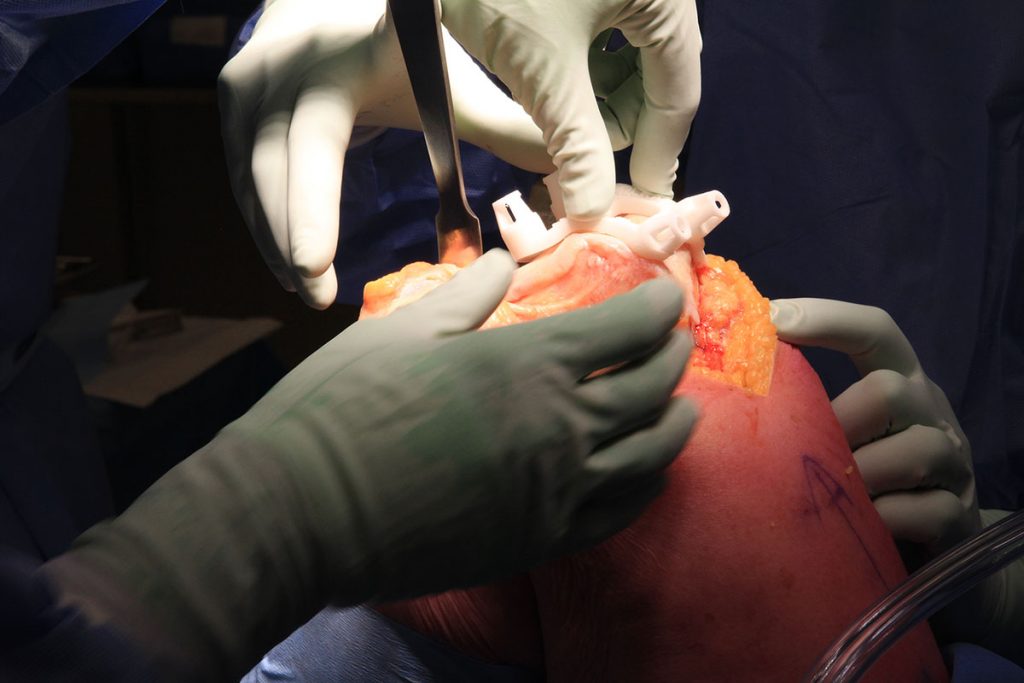
One component of this is the integration of 3D printed, patient-specific surgical guides that take the uncertainty out of the procedure itself. These surgical guides are produced using data gathered about an individual patient’s knee and are fabricated in-house on a 3D printer. When placed upon the patient during surgery, they guide the surgeon to exactly where cuts need to be made in relationship to where the knee is resting. Dr. Saskia Boekhorst is an orthopedic surgeon at Orthoparc, and she described the impact these guides have had in her experience:
“I’m a big fan of the patient-specific knee guides because this technology allows me to place the components of the knee arthroplasty exactly in the right axis of the leg in all dimensions. The first one hundred cases I’ve double checked by manual measurements, because it was a different approach and I am very careful. But after seeing very nice and consistent results, I became convinced.”
This increase in precision means that the surgery is more exactly what the patient needs and reduces the risk of unnecessary or erroneous incisions. The surgical guides also make the surgery less invasive, removing the need to drill into the femur canal as in traditional knee replacement surgery procedures. They also help decrease the amount of time the patient has to spend in surgery, as Dr. Boekhorst explained:
“The positioning and alignment are already done by me within an interactive planning software in which I can rotate the knee in all directions and see how the prosthesis could be placed for a particular patient. You will never be able to see this in all these dimensions and directions with a real patient because of soft tissue.”
All of this adds up to mean that there is less anesthesia necessary and less powerful post surgery painkillers required. Not only does that reduce the risks associated with such powerful medicines but allows the patient to be more fully cognizant and mentally focused on an increased timeline, something which is necessary for the implementation of a physical therapy regimen.
It’s not just good for the patients, it also makes sense for the surgical team in terms of reducing stress and ensuring they are better prepared for the operation. In addition, using these guides means that fewer surgical tools need to be prepped and sterilized as the knee guides come in a comprehensive ‘knee in the box’ package that includes all the necessary instrumentation and two sizes of preselected implants to treat a single patient. This means less overhead and a reduction in logistics cost, something which allows the medical practice to reinvest its resources elsewhere, such as in its staff and patients.
What do you think of this news? Let us know your thoughts; join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source/Images: Materialise]
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
First Containerized System from AML3D Now Operational at US Navy AM CoE
Shipbuilding giant Austal USA recently announced the launch of the Digital SEA (Secure Exchange for Additive) platform, which should play a major role in expanding accessibility to the sorts of...
3D Printing Financials: Materialise Improves Margins Despite Flat Revenue
Materialise (Euronext and NASDAQ: MTLS) started 2026 with stable revenue, stronger margins, and better operating profit, helped by growth in medical and improved profitability in software. The Belgian 3D printing...
3D Printing News Briefs: May 7, 2026: Metal Powder Bed Fusion, Surgical Plates, & More
In today’s 3D Printing News Briefs, we’ll start with a strategic collaboration to advance next-generation metal additive manufacturing (AM), before moving on to funding for surgical research. We’ll end with...
3D Printing News Briefs, May 2, 2026: Soft Robots, Agricultural Waste, & More
In this weekend’s 3D Printing News Briefs, we’ll start off with a multi-laser metal powder bed fusion 3D printer and post-processing news. We’ll end with research into soft robotics and...