Building Surgical Skills with 3D Printed Practice at University of Michigan Medical School
 As with any profession that has immediate, real life consequences that are starkly set out in terms of life and death, the more practice that a surgeon can get before actually performing a procedure, the better it is for everybody. The way in which surgeons historically would have gotten the hands on experience necessary to allow them to build their skills would have been by working with human cadavers, animals, and, finally, actual patients.
As with any profession that has immediate, real life consequences that are starkly set out in terms of life and death, the more practice that a surgeon can get before actually performing a procedure, the better it is for everybody. The way in which surgeons historically would have gotten the hands on experience necessary to allow them to build their skills would have been by working with human cadavers, animals, and, finally, actual patients.
Clearly, the more practice, the better. Recent studies have demonstrated that there is a lapse in surgical skills that results when long periods of time intervene between opportunities to practice particular, highly advanced surgical techniques. Even for those who have years of surgical experience, there are incidences in which the time between opportunities to perform a particular procedure are long, or the particulars of a case are so strikingly unusual that practice is highly desirable.

Three-dimensional models based on real human cases like these allow hands-on experience for surgeons in training. [Image: Michigan Medicine]
The ability of 3D printers to produce lifelike models for surgical preparation is being adopted by an increasing number of medical training programs. Documentation of ifs effectiveness as a learning tool is emerging from a multitude of sources, most recently in an article published in Otolaryngology–Head and Neck Surgery by a team or researchers at University of Michigan. In an interview with Science Daily, lead author Dr. David Zopf of C.S. Mott Children’s Hospital explained the benefits that 3D printing is bringing to the preparation of the next generation of surgeons:
“3D printing is bringing a whole new meaning to hands-on experience for surgeons in training. Hands-on experience is critical for acquiring and improving surgical skills, especially of new and complex procedures. This is an exciting tool that not only offers trainees exposure to opportunities they otherwise wouldn’t have but that also allows them to demonstrate proficiency of skills before being performed on children.”
The particular procedure undertaken by Zhao, along with 18 of her fellow students, as part of her training was in an otolaryngology head and neck surgery dissection course and represented a case of severe tracheobronchomalacia, a condition in which the windpipe periodically collapses, thereby not allowing for the child to breathe normally. These kinds of interventions require the carving of cartilage from the patient’s ribs and grafting it into place, as Dr. Zopf described:
“Airway reconstruction for specialized cases is a technically demanding procedure that often involves carving cartilage to support and expand a reconstructed trachea. Currently, a surgeon in training has scarce opportunity to carve cartilage graft for this type of procedure. We want to see if 3D printing can accelerate and enhance surgical training.”
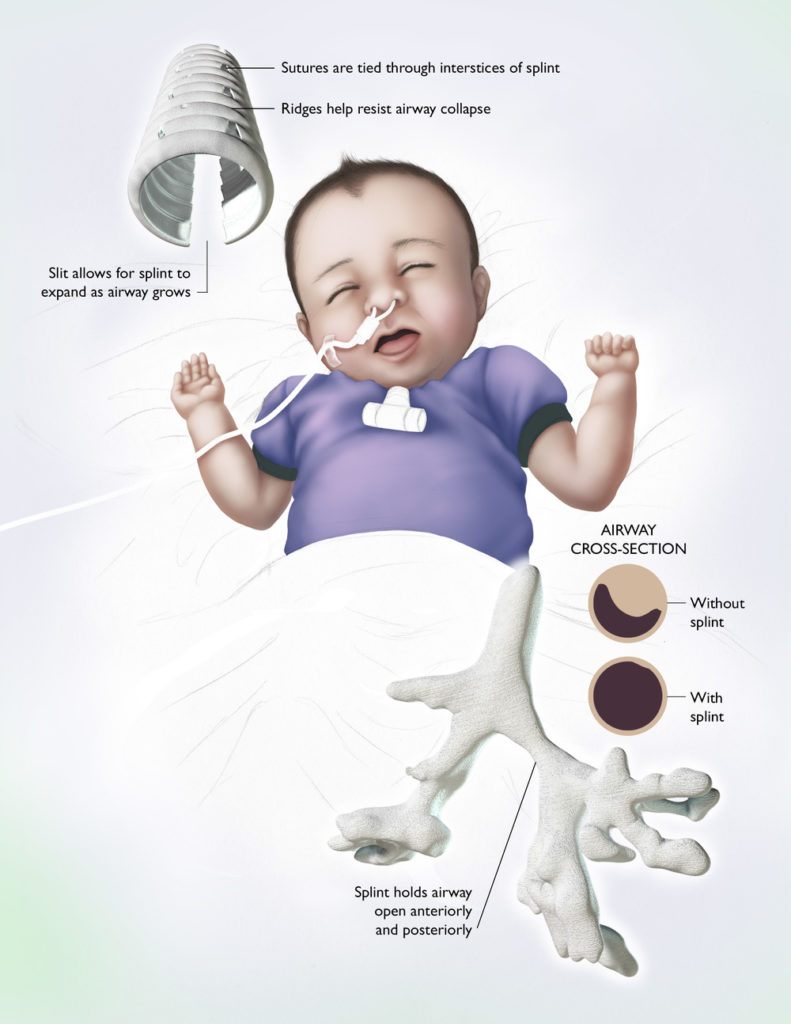
Illustration of condition of tracheobronchomalacia and splint used in treatment. [Image courtesy of Lumedia]
“You only get one chance to carve a harvested graft from a patient’s rib, so you have to do it perfectly the first time. It takes years of practice to learn the technical skills to do it. This was a very realistic experience and what’s great is you can keep printing dozens of these models at a time so you can practice over and over again.”
The use of 3D printed models gives not only new surgeons practice before performance, but helps experienced surgeons maintain those skills, especially when dealing with particularly rare types of procedures that may not occur with sufficient frequency for their regular practice. While it may seem intuitive that 3D printed models are a benefit to the training of medical students and the ongoing maintenance of skills for practitioners, very little is done on a broad scale in medicine without a significant amount of research done in support. As such, articles such as the one just published by the team at the University of Michigan are slowly, but surely, building the case for the integration of 3D printing into a wide variety of aspects of the practice of medicine. Discuss in the University of Michigan forum at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Printing Money Episode 38: Additive Manufacturing Deal Analysis with Rajeev Kulkarni
Welcome to Printing Money Episode 38. Rajeev Kulkarni returns for this episode, and we find it hard to believe it’s been nearly two years since his first appearance. In the interim,...
3D Printing News Briefs, May 14, 2026: Project Calls, Reseller, Reconstructive Surgery, & More
We’re starting off today’s 3D Printing News Briefs with two new Project Calls from America Makes. We’ll move on to some more business, with Axtra3D expanding its presence in North...
Fabric8Labs & University of Illinois Collaborate on 3D Printed Copper Cold Plates for Data Centers
Collaboration between emerging technology enterprises and research universities is one of the most consistently winning tactics for any nation building (or rebuilding) an industrial ecosystem. It’s an especially constructive approach...
3D Printing News Briefs: May 7, 2026: Metal Powder Bed Fusion, Surgical Plates, & More
In today’s 3D Printing News Briefs, we’ll start with a strategic collaboration to advance next-generation metal additive manufacturing (AM), before moving on to funding for surgical research. We’ll end with...
















































