University of Rochester Medical Center: New 3D Printed Medical Models for Training Even Bleed
 Throughout the centuries, medical students (and their teachers) have had to be very creative in finding ways to train for surgeries, as well as the most elementary procedures like stitching up wounds. From using cadavers—a rather gruesome but helpful practice—to use of a variety of models with different textures, obviously the best experience is in actually performing procedures on humans in the medical setting.
Throughout the centuries, medical students (and their teachers) have had to be very creative in finding ways to train for surgeries, as well as the most elementary procedures like stitching up wounds. From using cadavers—a rather gruesome but helpful practice—to use of a variety of models with different textures, obviously the best experience is in actually performing procedures on humans in the medical setting.
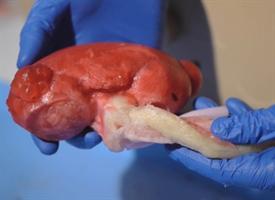
3D printed medical models are offering great new opportunities for those in training, however, along with surgeons learning how to perform procedures that have never been done before. Now, doctors at the University of Rochester Medical Center (URMC) have found a way to 3D print even further progressive models of organs and different parts of the human anatomy that even bleed when they are cut, offering an incredibly realistic experience, along with allowing the student to get a much better feel for what would happen in real world applications.
It is expected, according to a recent news release by the University of Rochester Medical Center, that these 3D models may soon be used in ‘rehearsals’ for intricate surgeries, an increasingly popular idea among those studying human anatomy and surgical needs. This particular program, Simulated Inanimate Model for a Physical Learning Experience (SIMPLE), has been headed up by Ahmed Ghazi, M.D., M.Sc., an assistant professor in the Department of Urology, and Jonathan Stone, M.D., a Neurosurgery resident already with a degree in biomedical engineering too.The researchers are using MRIs or CTs to convert images into digital designs that can be 3D printed and then used for training purposes—offering all of the positives in learning and none of the negatives if they make a mistake.
“Very few surgical simulations are successful at recreating the live event from the beginning to the end,” said Dr. Ghazi. “What we have created is a model that looks, feels, and reacts like a live organ and allows trainees and surgeons to replicate the same experience they would face in the operating room with a real patient.”
The team began working on making 3D printing models for medical training over two years ago. Dr. Stone had access to a 3D printer, and upon collaborating with Dr. Ghazi, they began fabricating the innovative training devices by creating molds from the 3D data, and then injecting them with hydrogel for a more realistic model as the texture simulates the human body very closely. Working with the University of Rochester Department of Biomedical Engineering, the team tested their models to see how similar they really were to human tissue, and found that there was a very strong correlation.
“We think of it as a science and engineering, although at its heart it is really arts and crafts because at the end day we are creating sculptures that just happen to be anatomical,” said Dr. Stone.

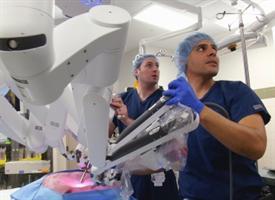
Medical students removing a gall bladder on a model patient [Image: University of Rochester via New Atlas]
“Simulation is one of the fundamental things that we need in surgery to allow us to improve what we do every day,” states Jean Joseph, M.D., MBA, Department of Neurology.
“As an experienced surgeon, when I am working with these simulations it is often hard to tell that it is not a real patient.”
The models need to feel and respond just like real organs. Along with their success in creating simulated tissue, the researchers are also able to 3D print bone-like structures for practicing surgeries pertaining to the skull or the spine. And this is only the beginning. The research team is on a mission to see that eventually all those in training will be able to comprehensively practice for surgeries, training on the entire anatomy and learning how to perform exercises such as:
- Guiding surgical instruments into place
- Moving organs out of the way
- Clamping blood vessels
- Resecting and removing tumors
“We have had times when we are doing these simulations in the OR when nurses or other physicians have looked in the window and thought we were doing the real thing, and have even gone so far as to scrub and put their masks on before coming in thinking there was a patient on the table,” said Dr. Ghazi.
This 3D printing process should offer further help to surgeons also as they will be able to create models from patient scans showing the actual tumors and health issues, allowing for completely patient-specific practice as well as guiding during surgery. The benefits for students—and ultimately, the patients—are enormous.
“There really isn’t another effective alternative for students,” said Dr. Stone. “Virtual reality hasn’t gotten far enough to feel like they are operating and, as a result, medical surgical education is lacking. This gives them a whole task training model and that not only benefits the students that want to go into surgery, but also those that aren’t interested in it as well because they are able to gain a perspective and appreciation of surgical methods and technologies that they may not otherwise be exposed to.”
Discuss in the 3D Printed Medical Models forum at 3DPB.com.
[Source: University of Rochester Medical Center / Images: URMC via New Atlas]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
You May Also Like
3D Printing Grows to $15.9B in 2024 Amid Shifting Industry Dynamics
The global additive manufacturing (AM) market reached $15.9 billion in calendar year 2024, according to “Q4 2024 3DP/AM Market Data and Forecast” from Additive Manufacturing Research (AM Research). Despite a...
Low-cost “Suzy” Polymer Powder 3D Printer is Faster and Cheaper than Past Models
Polish laser powder bed fusion (LPBF) firm Sinterit has released a follow-up to its predecessors, Lisa and Nils, called Suzy, a $19,490 printer equipped with a 30W fiber diode laser....
BellaSeno’s 3D Printed Breast Implants Keep Shape with 87% Fat Volume, Avoids Silicone Risks
At a medical conference in Austin this week, a new kind of breast implant took center stage. It is not made from silicone but from a 3D printed, fully resorbable...
Australia’s Untapped Potential as a Disruptive Innovator: SPEE3D CTO Steven Camilleri Explains Why He Wants to Make Stuff There
When I first met Steven Camilleri in 2023, the CTO of additive manufacturing (AM) OEM SPEE3D shared a quote with me from Clayton Christensen, the late Harvard professor who popularized...