3D Printed Skull Models Make Nasal Endoscopy Easier on Everyone
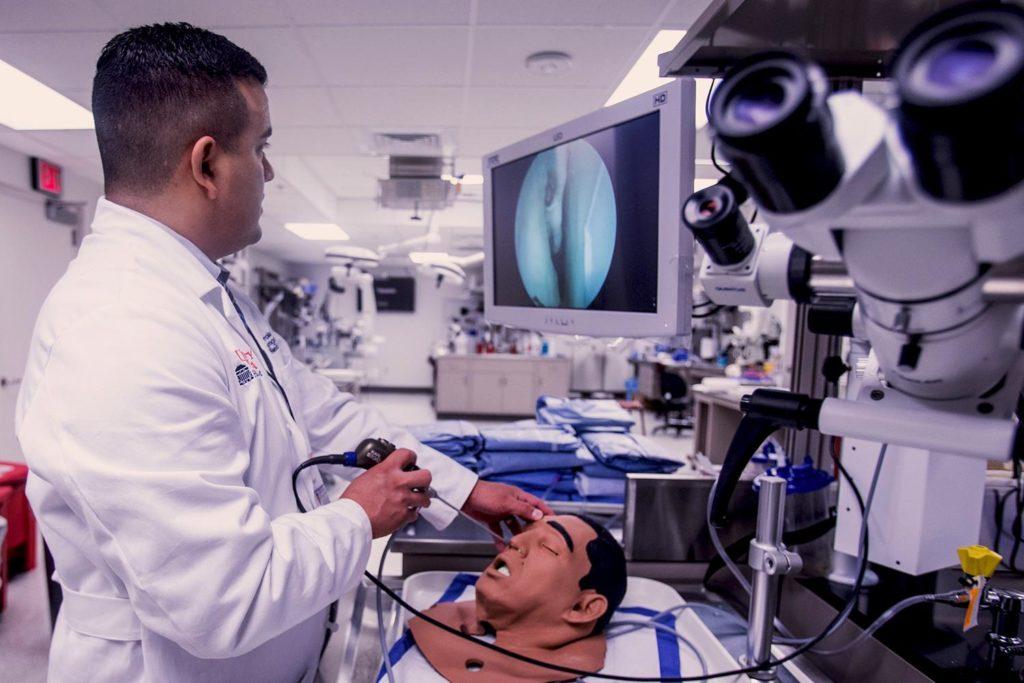
I know a few people who are guilty of ignoring potential health problems because they just don’t want to deal with uncomfortable or painful testing procedures. I get that; I could probably benefit from getting my chronic sinus issues looked into, but the thought of a nasal endoscopy is so odious to me that I’d rather just deal with sinus infections. A nasal endoscopy is a process in which a physician inserts a long scope with a camera at the end into a patient’s nasal cavity to have a look around, and while I will continue to happily opt out, many people with more serious problems don’t have that choice.
Otolaryngology students often don’t get to opt out either. According to Dr. Jose Gurrola II, a rhinologist at the University of Virginia Health System, when he was a resident, he and his fellow students would have to practice endoscopies on each other before they ever had to do one on a patient. Don’t let that prospect dissuade you from going into the otolaryngology field, however, because Dr. Gurrola and a few of his colleagues have developed a way for students to practice endoscopy procedures without subjecting their classmates to their fumbling attempts.
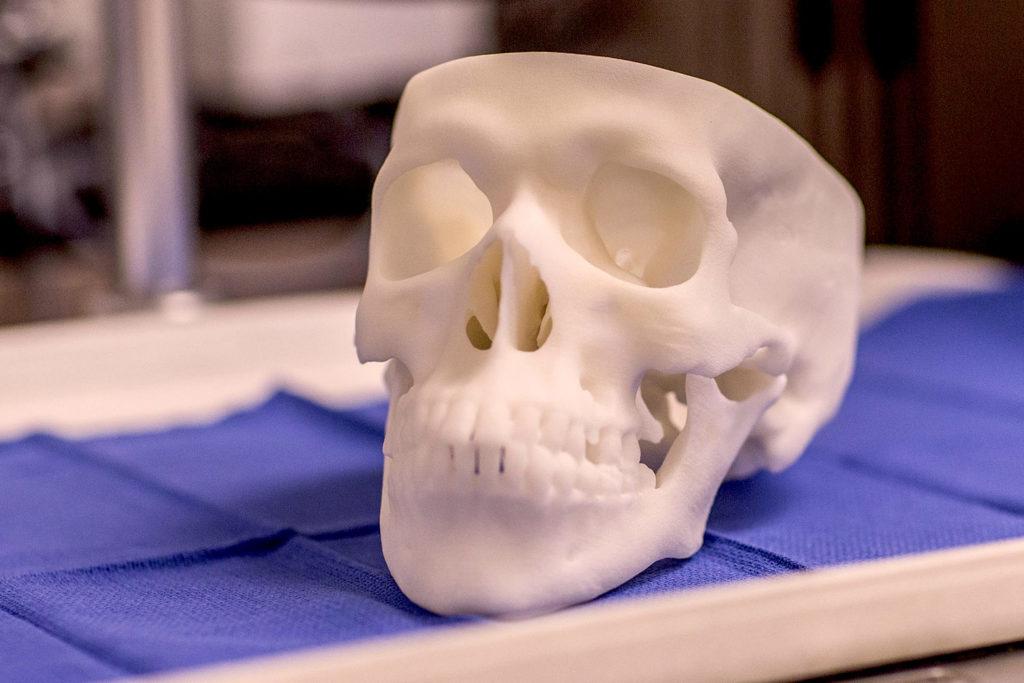 Along with otolaryngology resident Dr. Robert Reed and design lab engineer Dwight Dart of the UVA School of Engineering and Applied Science’s Rapid Prototyping Lab, Dr. Gurrola has created 3D printed skulls that allow procedures such as endoscopy to be practiced and perfected before residents ever have to perform them on a patient. It’s a relief for the students, who don’t have to be subject to the procedure themselves – or worry about maiming a classmate – as well as the patients, who can be assured that their doctor has plenty of experience.
Along with otolaryngology resident Dr. Robert Reed and design lab engineer Dwight Dart of the UVA School of Engineering and Applied Science’s Rapid Prototyping Lab, Dr. Gurrola has created 3D printed skulls that allow procedures such as endoscopy to be practiced and perfected before residents ever have to perform them on a patient. It’s a relief for the students, who don’t have to be subject to the procedure themselves – or worry about maiming a classmate – as well as the patients, who can be assured that their doctor has plenty of experience.
Like other 3D printed medical models, the skulls are created by converting CT or MRI scans to 3D models and then printing them. They’re relatively inexpensive to create and can be used again and again; according to Dr. Gurrola, the models are made freely available to students and doctors in affiliated programs such as neurology at UVA.
“The models allow students, residents and doctors to see, feel and understand dimensions of real human geometry,” Dart said.
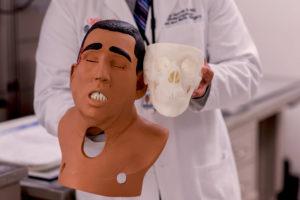
Once the skulls are printed, they are covered with facial masks that, while a bit disturbing-looking, give the students a feel for working on an actual patient. Surgical simulation software further guides them as they go through the procedure. Dr. Gurrola and Dart believe that they can further improve upon the models by adding sensors and fluid flow lines to better simulate the physical reactions that residents might encounter during an endoscopy. It’s a very reasonable goal, as 3D printed surgical models get more and more advanced and realistic.
“For those patient cases that may be unique or different, the 3-D models should be able to provide us with the option of examining that particular anatomy,” Dr. Gurrola said.
 The models are being created thanks to funding from the School of Medicine’s Graduate Medical Education Innovation Grant. They’re the latest in a series of 3D printed medical advancements that have come out of the Rapid Prototyping Lab since it was opened five years ago.
The models are being created thanks to funding from the School of Medicine’s Graduate Medical Education Innovation Grant. They’re the latest in a series of 3D printed medical advancements that have come out of the Rapid Prototyping Lab since it was opened five years ago.
“For the most part, surgical training is still a process where trainees pass through a continuum that still looks a lot like the ‘see one, do one, teach one’ model of old,” said Dr. Reed. “Our hope is that with the continued development of simulations such as this, we can improve upon this model.”
Discuss the topic of these new training models further over in the 3D Printed Skulls for Training forum at 3DPB.com.
[Source: University of Virginia / Images: Sanjay Suchak/University of Virginia]
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
AM & the Military’s Self-Infliction of Rapid Change
I’ve noted before that the additive manufacturing (AM) market for defense has started to evolve so quickly that it’s impossible to even keep track of all the updates in real...
ROBOZE Buys Dimanex Assets to Build “Physical AI” Platform
Dutch firm Dimanex got its start as an MRO platform for the railways. The company had a contract with the Dutch Army in 2018, and later that year signed one...
3D Printing Financials: Nano Dimension Reports Q1 Growth Amid Restructuring and Asset Sales
Nano Dimension (Nasdaq: NNDM) started 2026 with a much larger first quarter business than it had a year ago, mainly because Markforged is now part of the company and included...
3D Printing Financials: Stratasys Bets on Defense and Drones as Printer Sales Slow
Stratasys (Nasdaq: SSYS) started 2026 with lower revenue and a larger loss as customers continued to slow down spending on new 3D printers. Still, the company pointed to stable recurring...