3D Bioprinted Placenta Model May Lead to Treatment for Leading Cause of Maternal Death
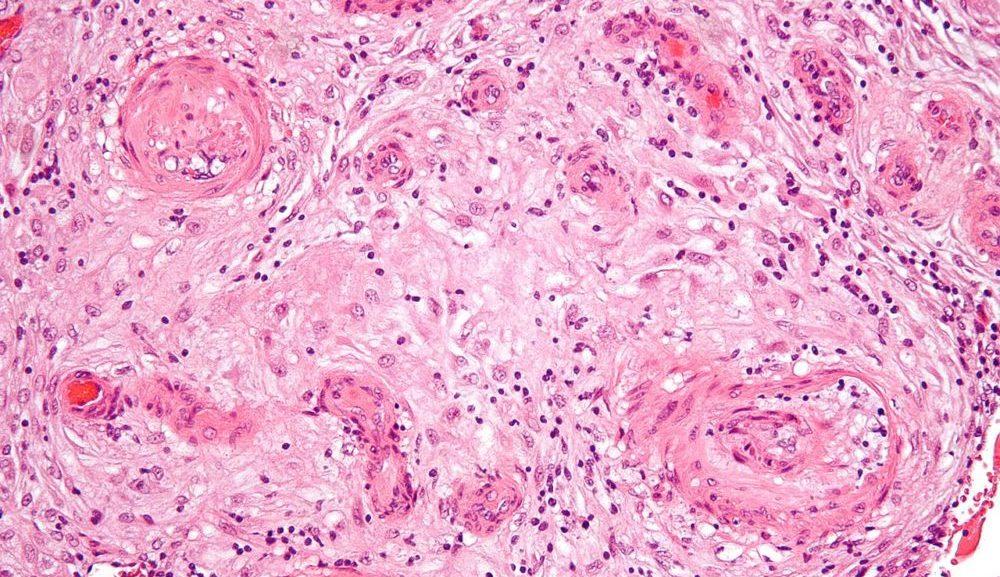
 Despite preeclampsia being the leading cause of death from pregnancy there is a surprisingly little amount of information known about it, what causes it and how to prevent it. The condition occurs in about 5% of pregnancies worldwide, and while thankfully it isn’t always lethal, it does lead to approximately 30,000 deaths each year. Part of the problem with learning more about preeclampsia is the fact that the placenta is an organ that doesn’t really exist until a woman becomes pregnant, making it difficult to impossible to accurately study without putting the mother and fetus in jeopardy. Additionally, the human placenta is different from that in nearly all other mammals, so research and testing on an animal placenta wouldn’t lead to much useful data.
Despite preeclampsia being the leading cause of death from pregnancy there is a surprisingly little amount of information known about it, what causes it and how to prevent it. The condition occurs in about 5% of pregnancies worldwide, and while thankfully it isn’t always lethal, it does lead to approximately 30,000 deaths each year. Part of the problem with learning more about preeclampsia is the fact that the placenta is an organ that doesn’t really exist until a woman becomes pregnant, making it difficult to impossible to accurately study without putting the mother and fetus in jeopardy. Additionally, the human placenta is different from that in nearly all other mammals, so research and testing on an animal placenta wouldn’t lead to much useful data.
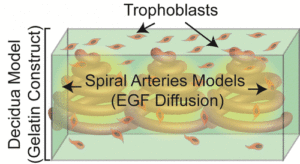
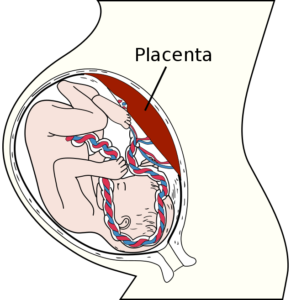 We may be on the road to understanding more about how the placenta works, and what happens when it doesn’t work, thanks to 3D bioprinting. A team of researchers brought together from from the Sheikh Zayed Institute for Pediatric Surgical Innovation at Children’s National Health System and the Tissue Engineering & Biomaterials Laboratory, Fischell Department of Bioengineering at the University of Maryland created the first 3D bioprinted placenta model and successfully used it in a preeclampsia study. Modern bioprinting has advanced to the level that the research team was able to successfully produce a placenta model that would accurately mimic the organ’s highly complex cellular structure. The placenta model provided the researchers with an opportunity to produce groundbreaking research that could lead to new, life-saving treatments for a wide range of pregnancy-related medical complications.
We may be on the road to understanding more about how the placenta works, and what happens when it doesn’t work, thanks to 3D bioprinting. A team of researchers brought together from from the Sheikh Zayed Institute for Pediatric Surgical Innovation at Children’s National Health System and the Tissue Engineering & Biomaterials Laboratory, Fischell Department of Bioengineering at the University of Maryland created the first 3D bioprinted placenta model and successfully used it in a preeclampsia study. Modern bioprinting has advanced to the level that the research team was able to successfully produce a placenta model that would accurately mimic the organ’s highly complex cellular structure. The placenta model provided the researchers with an opportunity to produce groundbreaking research that could lead to new, life-saving treatments for a wide range of pregnancy-related medical complications.
There are some medical theories that suggest that one of the causes of preeclampsia lies with a type of special cell in the placenta called trophoblasts. In a healthy placenta, the trophoblasts attach themselves to the uterine wall and then start to grow into the tissues of the uterus during the first stage of pregnancy, essentially bonding both organs together. At that point they connect to the mother’s blood vessels, which plays a vital role in helping to nourish and encourage growth in the fetus. The theory is that if the trophoblasts do not migrate normally it could lead to poor placental perfusion, the insufficient blood flow between a placenta and a uterus that causes preeclampsia.
In a new study that was published in American Chemical Society (ACS) Biomaterials Science & Engineering, the scientists detail their research which involved using the bioprinted model to observe the migration of trophoblasts cells form the placenta to the uterus. The bioprinted placenta model created by the research team contained key cellular, biochemical, and extracellular matrix components that accurately simulated the process of trophoblast migration. This is the first time scientists were able to successfully 3D bioprint a placenta and test cell migration of this type, and it could lead to several life-saving medical treatments.
“Our study provides a proof of concept that a 3D bioprinted placenta model is a viable way to study and understand the dynamics of cell migration in the formation of the placenta. What we have learned from this initial study is a significant step toward understanding the cause of preeclampsia and a potential therapy,” explained the chair of the Fischell Department of Bioengineering and the University of Maryland, John P. Fisher.
The team was able to successfully use the 3D bioprinted placenta model to track the results of introducing epidermal growth factor (EGF), a peptide that stimulates cell growth, proliferation, and differentiation, on trophoblast migration. The results strongly suggest that introducing the EGF to the placenta had a positive effect on the migration of the trophoblasts. While there is still more testing required, it seems that EGF may be a potential therapeutic treatment for preeclampsia. The reason that the 3D bioprinted model was able to provide such valuable data is the fact that the scientists were able to learn far more about the dynamic behavior of the trophoblast cell movements than more traditional 2D models.
When a 2D model is used researchers can only tell that a cell has moved, but with the 3D model they were able to see how it moved, where it moved and if a group of cells moved together. According to their research paper, the 3D bioprinted placenta model is a promising first step to developing a more sophisticated placenta model that could be bioengineered as a powerfultesting and research tool. Being able to accurately simulate the biological workings of an organ like a placenta could help them develop new treatments for preeclampsia and other similar placenta-related conditions including placenta accreta and placenta previa.
The study, ‘Development of a 3D Printed, Bioengineered Placenta Model to Evaluate the Role of Trophoblast Migration in Preeclampsia‘, was authored by Che-Ying Kuo, Avinash Eranki, Jesse K. Placone, Kelly R. Rhodes, Helim Aranda-Espinoza, Rohan Fernandes, John P. Fisher, and Peter C. W. Kim.
Do you know anyone who suffered from preeclampsia who would find this information interesting and helpful? Let’s discuss over in the 3D Printed Bioengineered Placenta Model forum thread at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
3D Printing News Briefs, May 9, 2026: Financials, Large-Format Printer, Steels, & More
In 3D Printing News Briefs this weekend, 6K Additive has appointed a new COO and released its Q1 financials. Rolls-Royce opened a new AM Development Cell, and MODIX launched its...
LOOP 3D Reveals 3D Printer Designed for Industrial Uptime
LOOP 3D has released the LOOP PRO X+ TURBO Gen2. This version has been improved to meet the needs of manufacturing clients. The printer is meant to be a production unit...
3D Printing News Briefs, April 25, 2026: Competition Winners, AI Platform, X2D Printer, & More
In this weekend’s 3D Printing News Briefs, AMUG announced the winners of its Technical Competition, and Authentise launched AI platform Whisper at RAPID. Bambu Lab wasn’t at RAPID, but launched...
HP Continues to Lower Barriers to Adoption with Compact MJF 1200 & Other RAPID + TCT Announcements
This week at RAPID+TCT in Boston, HP Additive Manufacturing Solutions is celebrating ten years in the AM market. The company launched its Multi Jet Fusion 3D printing technology in Barcelona...