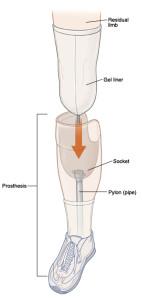
Patients who are missing limbs are generally prescribed socket-type prostheses that are custom-made to fit over their missing arm or leg. Despite two million people in the United States living with the loss of a limb, very little has changed about prosthetic technology over the years. While standard socket prosthetic devices are common, they are not without their flaws and drawbacks. The cost can often be tens of thousands of dollars, much of which is not covered by most healthcare plans. And there also tends to be a lack of stability when the prosthetic is used, which can result in falls or accidents. Ill-fitting prosthetics can also lead to complications like painful sores and ongoing, chronic pain. Curiously, 3D printing may be able to provide solutions to both of these issues.
The high cost of prosthetic devices is caused by the need for each device to be custom made for the patient. A socket that attaches to the amputee’s missing limb needs to be fit exactly and held in place with painful straps or braces. Even with a professional fit, sores and wounds are a common occurrence to those wearing the device. 3D scanning has greatly improved the ability to have prosthetic devices made for a specific patient however, and 3D printing is threatening to drop the price of prosthetic devices to a fraction of the cost of traditionally made prosthetics. 3D printing is also being explored as a way to make custom-fit prosthetic implants that are surgically implanted directly into the patient’s bone, so uncomfortable or improperly fit sockets are eliminated and the prosthetic will attach directly to the patient’s body.
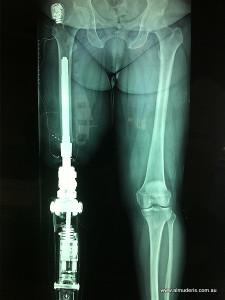
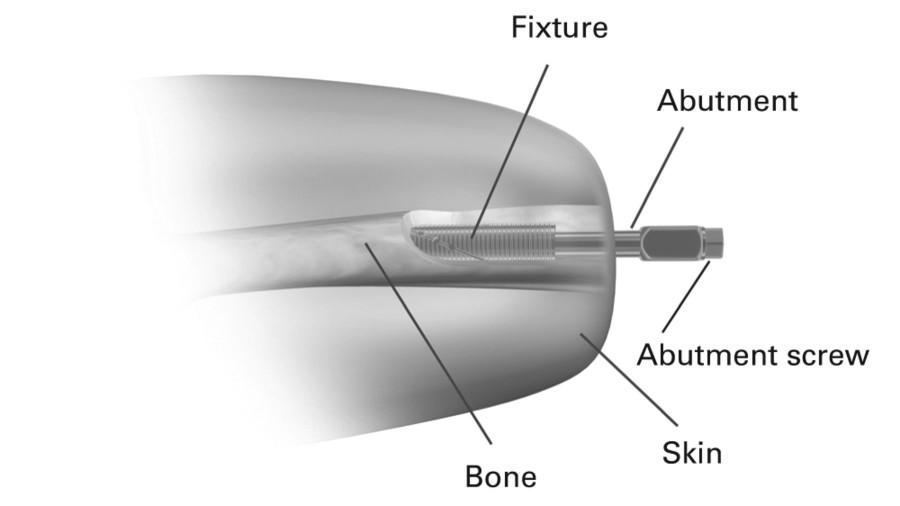
Research into osseointegration, the surgical integration of prosthetic implants with the amputee’s’ remaining bone structure, or direct skeletal prosthesis, has been explored for a few years now, but recently it has begun gaining popularity again. The implant will penetrate the skin and connect directly to the bone, so a prosthetic limb can physically be attached to the patient’s body. But the socket would be the only permanent implant, meaning the limb could easily be removed as needed. This direct prosthesis-to-bone connection offers a more stable connection to the patient’s body giving them greater control of the prosthesis and virtually eliminates any lingering pain or sores that traditional prosthetics can cause. It also offers the user more sensory feedback, so they can more directly interact with their environment.
“Unfortunately, these implants face several challenges which prevent their approval by the FDA outside of clinical trials. The implants need to conform to patient’s’ specific anatomy; the skin penetration of the implant is susceptible to infection; and a 12 month rehabilitation period is required to produce a stable bone-implant interface,” explained University of North Carolina at Chapel Hill and North Carolina State University researcher David Ruppert.
Sadly, the FDA has not approved implanted prosthetic sockets for general use; they have only granted exceptions for research purposes. The primary reasons are because of the various complications, which prohibitively cause the patient stress, and leave them open to ancillary injuries. Ruppert and his fellow researchers are focusing their efforts on addressing these drawbacks however, and hope to find ways to reduce the rehabilitation period and eliminate the worry over infection. They are also focusing heavily on finding ways of merging the implant and the patient’s’ specific anatomy, and 3D printing is looking to be a viable option.
“Our findings showed that rough textured implants created through 3D printing exhibit stronger bone integration than machine threaded counterparts. This highlights the superiority of using 3D printing to not only produce custom designs, but also custom surfaces that interface with amputees’ residual bones,” Ruppert continued.
Here is an animated video of how ssseointegration works:
The research team is also focusing on exploring the effects of using a therapeutic process called low intensity pulsed ultrasound (LIPUS) on the implant/bone connection. The process involves exposing the patient’s entire body to low-magnitude and high-frequency vibrations at a very specific amplitude range. Preliminary research has shown that this can increase the density of the bone around the implant, and to minimize the loss of bone during the rehabilitation process.
Ruppert and his fellow researchers recently presented their findings at the Annual Meeting of the Orthopaedic Research Society, an international organization that seeks to study, support and advocate for new musculoskeletal research findings. The Orthopaedic Research Society was founded back in 1954, and is currently the world’s largest forum for presenting musculoskeletal breakthroughs. Do you think use of these medical devices will become mainstream in the near future? Discuss in the 3D Printed Prosthetic Implants forum over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
BLT Touts 100,000 Copper Parts Made
With the significant volume of copper used in electronics, semiconductors, aerospace, defense, and beyond, copper additive has had immense promise from the early days of copper 3D printing at Beamit...
3D Printing News Briefs, March 28, 2026: TCT Asia, Distribution Agreement, FDA Clearance
We’re starting 3D Printing News Briefs this weekend with some news out of TCT Asia, and then moving on to a metal AM distribution agreement between MULTISTATION and WAAM3D. We’ll...
3D Printing Moves Deeper Into Production as Parts Near $110B by 2034
A new report takes a closer look at how much 3D printing is actually being used in real production. The numbers point to a market that is already growing at...
AM Applications Expected to Reach $110B in 2034, New Report Finds
Additive manufacturing may still be a relatively young industry, but the number of real parts being produced with 3D printing is growing quickly. According to a new report from Additive...