 3D printing is responsible for propagating a host of innovations in every sector, and in virtually every part of the world, thrilling artists, engineers, architects, and designers of all sorts as they realize the infinite opportunities for innovation that have been placed at their desktops and fingertips (and on their factory floors). One can just visualize 3D printers of all shapes, sizes, makes, and models pumping away all over the world with new innovations for making and presenting truly revolutionary art, making a million mechanical components (literally), car parts for celebrities, and even apparel, footwear, and comfort items like fancy insoles.
3D printing is responsible for propagating a host of innovations in every sector, and in virtually every part of the world, thrilling artists, engineers, architects, and designers of all sorts as they realize the infinite opportunities for innovation that have been placed at their desktops and fingertips (and on their factory floors). One can just visualize 3D printers of all shapes, sizes, makes, and models pumping away all over the world with new innovations for making and presenting truly revolutionary art, making a million mechanical components (literally), car parts for celebrities, and even apparel, footwear, and comfort items like fancy insoles.
But just as giddy with excitement are researchers in labs around the world, too. While their machines and materials may sometimes vary from that of the mainstream, researchers also have opened the door to a new world of discovery thanks to the 3D printer, bio-inks, and a host of new innovations on the ground, from 3D printed cellular structures of all sorts to a wide range of 3D printed prosthetics and medical devices.
 One area that is offering many options to researchers is that of converting radiology scans like MRIs and CTs to digital form, often resulting in what has now come to be a wide range of 3D models. But a new project, just outlined in ‘Rapid Prototyping of Inspired Gas Delivery System for Pulmonary MRI Research’ by Fredrick Roscoe Cook, Eric T. Geier, Amran K. Asadi, Rui Carlos Sá, and G. Kim Prisk of the University of California, San Diego, shows us the impact new technology is having on pulmonary research and how they can use those MRIs to even greater benefit now.
One area that is offering many options to researchers is that of converting radiology scans like MRIs and CTs to digital form, often resulting in what has now come to be a wide range of 3D models. But a new project, just outlined in ‘Rapid Prototyping of Inspired Gas Delivery System for Pulmonary MRI Research’ by Fredrick Roscoe Cook, Eric T. Geier, Amran K. Asadi, Rui Carlos Sá, and G. Kim Prisk of the University of California, San Diego, shows us the impact new technology is having on pulmonary research and how they can use those MRIs to even greater benefit now.
Those involved in assessing pulmonary function are very familiar with specific ventilation imaging, which is a type of MRI that helps establish levels of air in the lungs and how they are being distributed. Researchers are able to monitor signal changes as they respond to changes in inspired oxygen concentration, but this current system is not easily transferred to the clinical setting, and the current project aims to simplify SVI measurement.
The paper by University of California researchers discusses how they were able to use 3D printing to achieve the desired simplicity in measuring lung functionality in patients, upon the completion and evaluation of several preliminary prototypes. They found that the technology was indeed ‘well-suited’ for making the MRI-compatible devices.
“The new delivery system was evaluated based on O2 and N2 concentration step responses and validated against the current SVI protocol,” state the researchers in their paper. “The design performed rapid switching of supplied gas within 250 ms and consistently supplied the desired concentration of O2 during operation.”
“It features a reduction in the number of commercial hardware components, from five to one, and a reduction in the number of gas lines between the operator’s room and the scanner room, from four to one, as well as a substantially reduced preparation time from 25 to 5 min.”
3D printed materials were also found to be well-suited for these evaluation devices as in an MRI environment, items placed in the scanner room must be made of plastic or nonferrous metal. The researchers were able to make 3D printed custom hardware for offering rapid gas delivery as well as rapid switching. And in line with all the usual benefits of 3D printing, they were able to customize their work, and do so quite affordably.
“3D printing enabled inexpensive and speedy design iteration compared with traditional machining or purchase and assembly of commercially available products and provided the advantage of fabricating custom-designed hardware with MR safe materials,” state the researchers in their paper. “This resulted in a final design that is a simpler and more robust gas delivery method than the original plumbing system.”
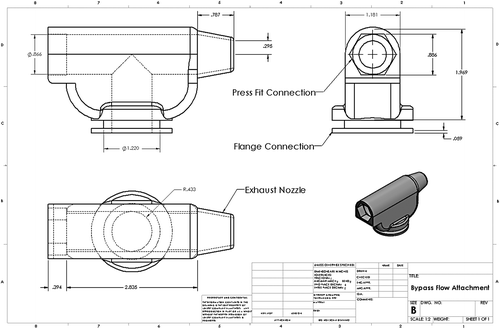
In the original system, the following components were to be found: inspiratory and expiratory tubing, remotely operated switching valve, and T-shaped three-way valve. According to the researchers, at least four lines of large-bore and small-bore tubing are passed through the wall of the MR scanner room. In the new, 3D printed system, the components are simplified in number to a mere one valve and one ‘pass through’ line.
“The new design utilizes bypass flow to supply a stream of gas for subjects to breathe from during operation,” state the researchers. “To our knowledge, there are no commercial components readily available that perform this specific function and are MR compatible.”

(A) The bypass flow attachment printed in PLA. (B) The facemask and bypass flow attachment worn by a subject. The supplied gas flows across the facemask for the subject to breathe from and exhausts into the environment. PLA, polylactic acid.
Using SolidWorks, the team was able to model the bypass flow attachment, then slice and prepare it in G-code using the MakerWare software that accompanied their MakerBot Replicator 2 printer. The settings used for printing were 0.2 mm layer height, 15% internal fill, and a wall thickness of two shells (0.8 mm). They used 45 g of PLA, and the printing time was just over three hours.
In conclusion of the very fruitful study, researchers noted that the new design was successfully used in multiple breath washout and SV procedures, and prep time for an experiment was nearly eliminated, going from 25 to 5 minutes, using the improved gas delivery system.
Price difference from traditional materials was duly noted by the researchers. For the bypass flow attachment to be machined out of polyetheretherketone (PEEK), the expense would be approximately $890, with two weeks to be factored in for delivery. Amazingly, with 3D printing, the attachment can be fabricated with $2 of materials and delivered overnight.
The design can also be customized to the specifications of the patient, like children, who would need a smaller size, and it’s extremely versatile overall.
“The inspired gas delivery system can be implemented in any research study involving rapid switching of inspired gasses while in the MRI,” state the researchers in conclusion. “It is MR safe, being constructed from PLA and nonferrous metals, and is manually operated without pneumatic remote control valves or other electronic equipment. The new gas delivery system improves safety by allowing normal breathing with and without supplied gas flow, and also adds the ability to perform SVI and multiple breath washout procedures simultaneously in the MR scanner.”
Overall, the researchers were quite happy to conclude that they found a very successful replacement method for delivering inspired gas to research subjects in the MRI environment. This is due to their study and resourcefulness as well as all the advantages offered by 3D printing—from customization allowing for better delivery by the attachment, to speed in production, greater affordability, and versatility.
“The design can also be easily modified, using computer-aided design software, to fit different equipment, making the technique of 3D printing an advantageous alternative to fabrication by machining or purchase of commercial hardware,” state the researchers.
Are you surprised that 3D printing has an impact in this area of research? Discuss in the 3D Printed Gas Delivery System forum over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Consolidation in AM: How 2025 Is Shaping the Industry’s New Normal
The first half of 2025 has been marked by a clear shift in the additive manufacturing (AM) industry. Companies are no longer just focused on developing new tech by themselves....
Etsy Design Rule Change Reduces Selection of 3D Printed Goods
Online marketplace Etsy has implemented a rule change requiring all 3D printed goods on the site to be original designs. The update to the site’s Creativity Standards states, ¨Items produced using...
U.S. Congress Calls Out 3D Printing in Proposal for Commercial Reserve Manufacturing Network
Last week, the U.S. House of Representatives’ Appropriations Committee moved the FY 2026 defense bill forward to the House floor. Included in the legislation is a $131 million proposal for...
Transforming From Tourist to Native: Duro CEO Michael Corr Explains Why the Company Rebuilt its PLM Software on AI
In these early innings of the AI boom, many market analysts have expressed concern that AI spend has gotten too far ahead of the technology’s proven ability to deliver significant...
































