When Dr. Michael Slag was diagnosed with a rare tumor, he immediately knew the risks of the surgery that would be needed to remove it. The Pancoast tumor sitting at the top of his right lung is such a rare type of cancer that the Mayo Clinic, where Dr. Slag went for treatment, has only seen 60 cases in the last 20 years.
The potential complications were many. The tumor was wrapped around the top of his rib cage and intertwined with several critical nerves and blood vessels, which meant that its removal carried a high risk that Dr. Slag would lose at least part of the function of his right arm. For an endocrinologist whose job requires some very delicate work, even a minor loss of function could have been catastrophic.
To minimize the risk, a lot of preparation was needed, and that’s what 3D printed models are for. The surgical team that would operate on Dr. Slag was fortunately armed with Mimics Innovation Suite software from Materialise.
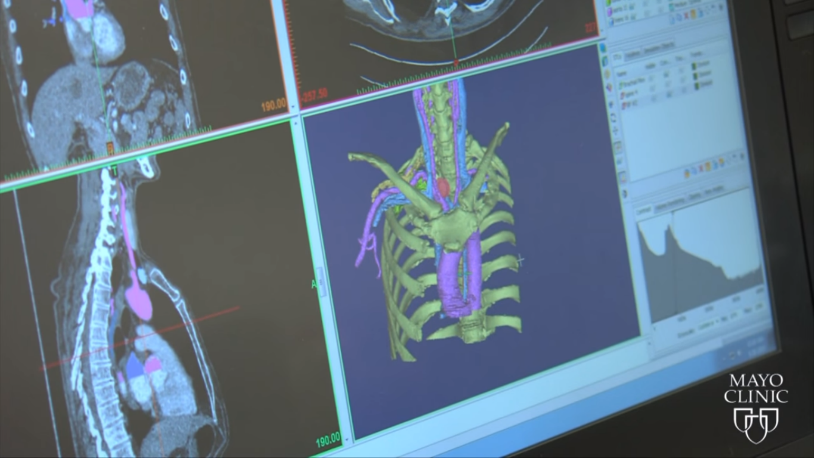
Using Dr. Slag’s MRI and CT scans, the team created a 3D model of the tumor and its surrounding area. The model, which took 70 hours to print, allowed the doctors to see the exact positioning of the tumor and how it interfered with the blood vessels and nerves.
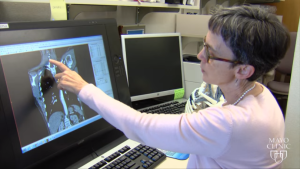
Dr. Jane Matsumoto from Mayo Clinic studies a 3D model in Mimics
“We frequently may have a plastic surgeon, an orthopedic surgeon, a vascular surgeon, and myself: all involved in a Pancoast tumor resection,” said Dr. Shanda Blackmon, a thoracic surgeon at Mayo Clinic. “And when that’s the case, there’s nothing better than having a model, for the whole team to meet around and plan the case…Clearly everyone’s tumor is different, and it’s always in a different location.”
With a 3D map in front of them, the surgical team knew the precise location of Dr. Slag’s tumor, and were able to plot their course ahead of time, virtually eliminating any surprises that may otherwise have come up during the surgery. Only a few years ago, a procedure like this one would have involved fully opening up the patient’s chest, resulting in a long, painful recovery and lots of potential complications. With the preparation that the 3D software and printed model allowed, the surgery was reduced to a quick, minimally invasive laparoscopic procedure.
“So the surgery that we performed was basically putting a camera in the side of the chest through a small hole that was created,” said Dr. Blackmon. “We had two additional ports, that are basically tubes that we put in between the ribs, that we passed instruments through. And that was all we did to resect his tumor.”
Dr. Slag left the hospital three days after the surgery, with almost no pain, and with both arms and hands fully functional.
“It’s unbelievable,” he said. “In fact, I was walking the first night after the surgery.”
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Hyliion CEO Thomas Healy on 3D Printing’s Role in the KARNO Generator
While the electric vehicle (EV) market faces an uncertain future, there’s no uncertainty about the fact that greenhouse gas emissions are drastically changing the climate on Earth. Thanks to its...
Attending the ASTM F42/ISO TC 261 Meetings: The Nitty-Gritty of Additive Manufacturing
I never thought I’d be so excited about an event focused on additive manufacturing (AM) standards, but here we are! When I learned that the recent biannual ASTM F42/ISO TC...
World’s Largest Polymer 3D Printer Unveiled by UMaine: Houses, Tools, Boats to Come
The University of Maine has once again broken its own record by unveiling the largest polymer 3D printer in the world. Surpassing its 2019 achievement, the new Factory of the...
Gorilla Sports GE’s First 3D Printed Titanium Cast
How do you help a gorilla with a broken arm? Sounds like the start of a bad joke a zookeeper might tell, but it’s an actual dilemma recently faced by...