 There is probably no disease in the world more detrimental to a developing nation’s advancement than malaria. Throughout developing regions in Latin America, Asia and Sub-Saharan Africa the World Health Organization (WHO) estimates that malaria costs over $12 billion a year in healthcare costs and lost wages, not to mention the detrimental effects on tourism and an estimated 800,000 deaths annually. While there are some drugs that ease the symptoms and reduce the likelihood of being infected, there still is no cure or vaccine. And because the disease is spread via mosquito bite, the only real defense against it remains the use of preventative measures like mosquito netting and hyper-vigilance in regards to standing water.
There is probably no disease in the world more detrimental to a developing nation’s advancement than malaria. Throughout developing regions in Latin America, Asia and Sub-Saharan Africa the World Health Organization (WHO) estimates that malaria costs over $12 billion a year in healthcare costs and lost wages, not to mention the detrimental effects on tourism and an estimated 800,000 deaths annually. While there are some drugs that ease the symptoms and reduce the likelihood of being infected, there still is no cure or vaccine. And because the disease is spread via mosquito bite, the only real defense against it remains the use of preventative measures like mosquito netting and hyper-vigilance in regards to standing water.
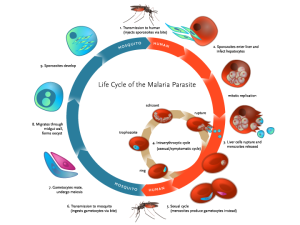
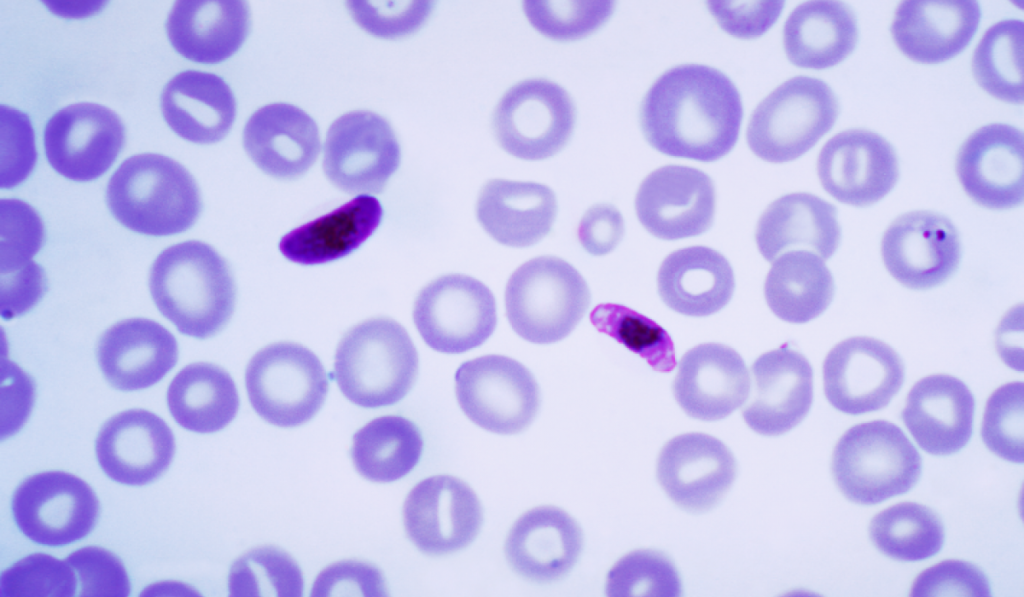
But a spinout company from University College London called MediSieve Ltd. may have stumbled onto a solution to the problem. It turns out that red blood cells infected with a malaria parasite gain slightly magnetic properties. When a red blood cell is infected with malaria, the parasite breaks down the blood’s hemoglobin, which results in a waste byproduct known as haemozoin – also called the “malaria pigment” – that is slightly magnetic. As the parasite multiplies and consumes the cell, the haemozoin builds up and remains stored within it, turning the cell magnetic.
The founder of MediSieve, Dr. George Frodsham, developed 3D printable magnetic blood filters that could potentially remove 90% of a patient’s infected blood cells in less than four hours. The filters only attract the blood cells with magnetic properties, allowing un-infected blood cells to pass through them harmlessly. Because at the time Frodsham was mostly on his own when it came to research and funding, his incredible device simply would never have been created had it not been for affordable RepRap 3D printing technology.
“I first came to 3D printing due to a resource issue, during my PhD we had relatively little funds but a clear idea of what I wanted to do and the answer was to buy a RepRap machine. I used it to make some early prototypes in-house and it made a huge difference because it meant I was able to iterate designs and try them out for a really low cost, really quickly. When I was happy with the design I was able to produce the numbers I needed to run my experiment, mass manufacture is a strong word but it wasn’t far off,” Frodsham explained to tct Magazine.
The blood filtering process works similarly to kidney dialysis, the patient’s blood is filtered through an external loop where the infected cells are separated from the healthy cells that are allowed to return to the patient’s body. The results for the patient are almost immediate, as the severity of the symptoms quickly begin to lessen, and the possibility of death is reduced to almost nothing.
Here is a video demonstration of the blood filtering process:
Frodsham earned his PhD in biochemical engineering from UCL, where he developed his magnetic haemofiltration device. While the company is still in the early stages of development, his work has still managed to attract a considerable amount of financial support. He received an enterprise fellowship from the Royal Society of Edinburgh, a grant that he used to get his company up and running. He also received an Enterprise Fellowship from the Royal Academy of Engineering’s Enterprise Hub for his work developing his first prototype filter. The early success of his prototypes allowed him to raise over $540,000 (£350,000) in early funding that will enable him to develop clinical prototypes and run safety trials. And according to Frodsham, 3D printing will be with him throughout the development process.
“I ended up using the RepRap not only for my project but to support a number of other research groups to make early prototypes, custom experimental apparatus, adapters for microscopes. Sometimes these things costs hundreds even thousands of pounds and you can print them for basically nothing. It adds huge value to the product development process when you’re talking about the development of new medical devices but also as a lab tool. For me it is an essential piece of lab equipment right now, I recommend 3D printing to everybody I speak to. We’re still looking at using 3D printing to produce the clinical prototypes, but we’ll be looking towards injection moulding when we scale up to manufacturing. This is a product that we’re hoping to help hundreds of thousands of people with, with those kinds of volumes I personally don’t feel like 3D printing is the most efficient way of doing it,” Frodsham says.
The timing of Frodsham’s device couldn’t come at a better time, as infectious disease researchers are becoming increasingly worried about the growing number of drug-resistant strains of malaria. There are currently three of these strains spreading across Cambodia, Laos, Thailand, Vietnam and Myanmar, and if they continue to spread they could cause a devastating epidemic.
Frodsham research and his resulting magnetic haemofiltration process may have a wider impact on the science of infectious diseases than just reducing the cost of malaria. Medical science typically focuses on chemical or pharmaceutical solutions to diseases, which has served us well for over a century. But the widespread use of drugs are causing unintended side effects by actually making parasites and viruses stronger and leading to drug resistant “super-virus” strains that are becoming more and more of a problem. However using his background in physics and nanotechnology, Frodsham instead looked for a physical, drug-free solution that would reduce the need for pharmaceutical treatments, giving the malaria parasites less opportunities to develop resistance.
Let’s hear your thoughts on this research and in the 3D Printing a Cure for Malaria forum thread on 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Ceramitec 2026 3D Printing Wrap Up
I was surprised by just how many 3D printing companies and 3D printing projects there were at Ceramitec this year. I came away from the show convinced that the ceramics...
RusselSmith Brings Additive to Ghana’s Maritime Sector
Nigerian firm RusselSmith is in talks with Ghana’s Maritime Authority (GMA) to bring 3D printing to Ghana’s maritime sector. The Commonwealth Enterprise and Investment Council (CWEIC) helped make the discussion...
The Blueprint for Industrial Serial Production
Lithoz is kicking off the 2026 trade fair season with a powerful showcase of real-world applications of ceramic AM serial production capabilities alongside new material upgrades. The company is stepping...
Fraunhofer ILT Tests 3D Printed Titanium Reactors to Generate Hydrogen Onboard Heavy Vehicles
The Aachen-based Fraunhofer Institute for Laser Technology (Fraunhofer ILT) is to research titanium aluminide hydrogen reactors and heat exchangers. The hope is that lightweight, better-performing 3D printed components will make...