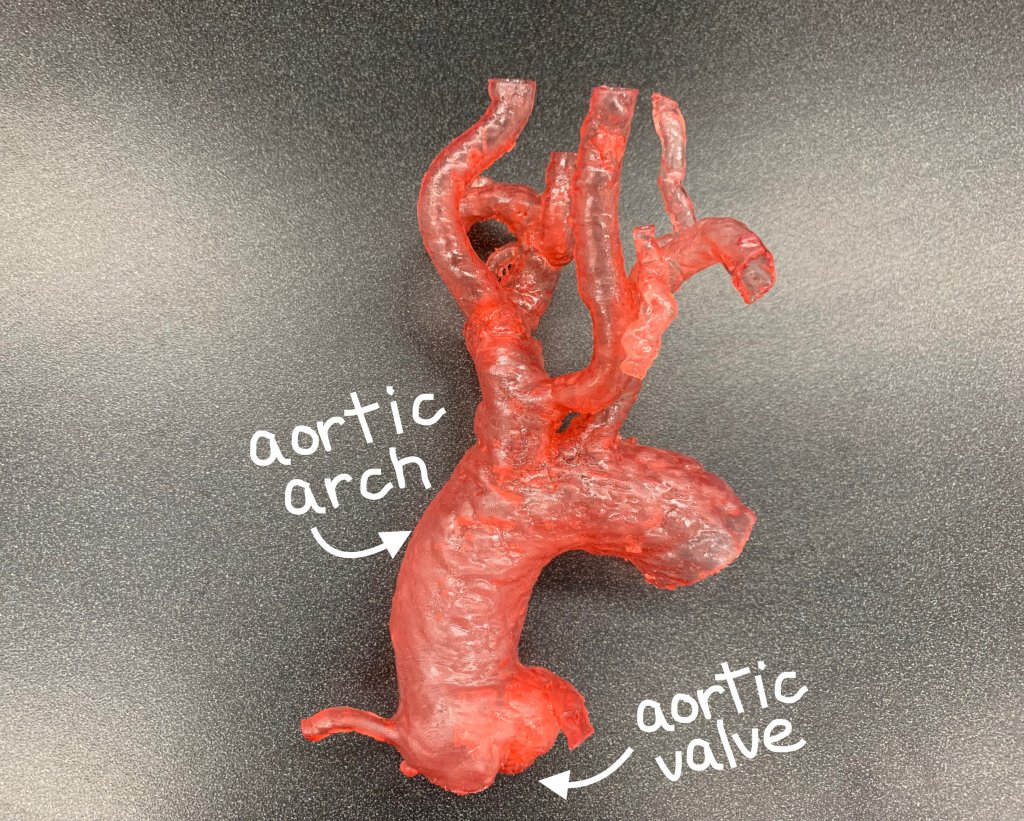
For over one hundred years, treating heart disease meant opening the patient’s chest to access the heart through open-heart surgery. The procedure usually takes between three to six hours and is associated with a lot of pain and suffering as well as possible surgical complications. On top of that, the patient has to be in good health to withstand the operation. However, throughout the last few years, the use of minimally invasive surgery has become extremely important for patients who are at intermediate or higher risk for death or major complications during the procedure. And just last month the U.S. Food and Drug Administration approved the procedure for low-risk patients who need to replace damaged valves. This was a big deal, since aortic stenosis is the most common valvular heart disease in the US, afflicting up to 1.5 million people, and many of them couldn’t or didn’t want to have open-heart surgery, so there were very few options for them. Still, if you thought things couldn’t get any better, try adding 3D printing to the equation. That’s just what the researchers and physicians at the VA Puget Sound Health Care System are doing: using 3D printing to aid in the diagnosis and treatment of complex heart conditions.
Recently, the VA Puget Sound (part of the U.S. Department of Veterans Affairs) and the University of Washington  (UW) School of Medicine announced a two-year partnership to develop new uses of 3D printing that could help cardiologists better visualize the complex anatomy unique to each patient and improve access to new minimally invasive treatments. This type of surgery has already proven to help reduce health care costs by hundreds of millions of dollars every year, also making surgery safer by lowering the suffering associated with surgical complications, and now with 3D printing, things can become easier for everyone involved.
(UW) School of Medicine announced a two-year partnership to develop new uses of 3D printing that could help cardiologists better visualize the complex anatomy unique to each patient and improve access to new minimally invasive treatments. This type of surgery has already proven to help reduce health care costs by hundreds of millions of dollars every year, also making surgery safer by lowering the suffering associated with surgical complications, and now with 3D printing, things can become easier for everyone involved.
The two organizations will share 3D printers, 3D materials, software, and a staff made up of physicians, researchers and engineers, to quickly develop new protocols for planning procedures, such as the creation of patient-specific 3D printed models for treatment of mitral valve disease—a complex heart abnormality that prevents blood from flowing properly out from the heart to the rest of the body.
“3D printing can benefit many aspects of structural heart disease, including disease affecting any of the four valves of the heart (aortic, mitral, tricuspid and pulmonic). Each valve has a different structure and different challenges to an interventional approach, and this is where being able to visualize that anatomy with 3D printing can really make a difference,” explained Beth Ripley, VA Puget Sound radiologist, to 3DPrint.com.
The VA is the largest integrated healthcare system in the United States and has one of the most extensive hospital-based 3D printing networks. The Veterans Health Administration (VHA) 3D printing network is already seeing first-hand the many benefits of 3D printing, everything from model kidneys to informing pre-surgical planning for veterans with renal cancer, and even specialized foot orthotics that help prevent avoidable amputations for veterans with type 2 diabetes. Cardiologists will soon be able to prepare even better for upcoming procedures and help their patients understand what type of treatment and surgery they’ll be getting, via life-sized 3D models of their own heart.
Ripley went on to say that “3D printed medical models can facilitate patient understanding and informed consent, training of physicians, diagnosis of disease and surgical planning. The next frontier will be exploration of patient-matched implants and surgical cutting guides. Finally, we are exploring bioprinting, which is 3D printing of structures that can support or are composed of living cells.”
Both UW Medicine and VA Puget Sound use Materialise Mimics 3D printing software, which is medically cleared, and GE Advanced Workstation Volume Share software. Both institutions have a wide variety of 3D printers at hand. The VA Puget Sound is equipped with:
- Stratasys F370 FDM printer
- Stratasys Mojo FDM printer
- Stratasys Objet 30 Prime polyjet printer
- Stratasys Objet 350 Connex3 polyjet printer
- Formlabs Form2 vat photopolymerization (SLA) printer
At the UW School of Medicine, Research Scientist Dmitry Levin manages a nationally recognized 3D printing lab that has produced more than 100 patient-specific models to guide the decisions of cardiologists and surgeons. In order to carry out their projects, the researchers at the UW lab use the following 3D printers:
- Dremel FDM printer
- Formlabs Form2 vat photopolymerization printer
- UNIZ SLASH pro vat photopolymerization printer
- NewPro 3D vat photopolymerization Printer
- Prusa i3 FDM printer
- Z Corp Zprinter 250 color 3D Printer
By joining with the VA, Levin said that they are merging “all of our collective expertise into a unified effort to offer patients personalized cardiac care based on their unique needs.”
“Now that the FDA has expanded a catheter-based approach to aortic valve replacement (TAVR) availability to patients at low surgical risk, we’ll see more cases that can benefit from 3D printed models for TAVR planning,” Levin added back in August when the institution announced the new partnership. “Beyond improving our understanding of a patient’s anatomy, (3D printing) allows us to know which catheters and replacement valves will fit, and how best to approach the particular structure. That knowledge turns into costs savings for the patient in terms of devices and procedure duration.”
Both VA Puget Sound and the UW Medicine were early adopters of 3D printing technology and are seen as leaders in their fields. Developments from this research agreement are expected to not only benefit VA’s 9 million enrolled patients and UW Medicine’s broad geographic patient base but also to reach patients outside of these hospital networks. According to VA Puget Sound, innovations from the collaboration are expected to inform future research, development, and scalability of 3D printing applications to advance treatment approaches to address the complexities of heart disease globally.
“VA Puget Sound Health Care System provides comprehensive care to more than 110,000 Veterans enrolled at one of its nine facilities in the Pacific Northwest (two divisions in Seattle and Tacoma; seven Community Based Outpatient Clinics in Bellevue, Bremerton, Chehalis, Federal Way, Mount Vernon, Port Angeles, and North Seattle). As the VA’s fifth-largest research program, VA Puget Sound has research in virtually every major clinical department, including: TBI & multiple blast exposures; memory improvement and Alzheimer’s Disease; PTSD and deployment health; Parkinson’s Disease, diabetes; cancer; substance abuse; lower limb prosthetics; genomics; and Health Services. Additionally, we have seven nationally recognized Centers of Excellence, in areas from limb-loss prevention and prosthetic engineering to primary care education and substance abuse treatment,” Ripley stated.
Ripley also reflected about the next frontier for the VA Puget Sound. She believes they will soon be moving into bioprinting, creating living, vascularized bone.
“Currently, when a bone has to be removed due to cancer or chronic infection, it must be replaced with bone taken from another source, often the patient’s own bone. This means a second surgical site and the loss of bone from that site. The goal of printing living, vascularized bone is to provide a means of replacing diseased bone without the morbidity of harvesting it from the patient. Patients with cancers affecting the bone or chronic infections (such as can occur with diabetes) will benefit the most. Success will also lay important groundwork for creation of other living tissues, such as organs.”
Like her colleagues in the VA, Ripley believes that heart disease, diabetes, and cancer are all chronic disease processes that 3D printing is addressing, and in the future, they would like to continue to extend the reach of the technology to address other health concerns. There are 18.2 million veterans in the US that could benefit from the advances in 3D printing, plus all the patients that would indirectly be aided thanks to the advances in research being undertaken. It feels like this is a win-win situation for the patient population of the United States, present and future.
[Images: VA Puget Sound Health Care System and UW Medicine]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Havaianas Collaborates with Zellerfeld to Launch 3D Printed Flip-Flops
The shoe of the summer is undoubtedly the flip-flop. Easy on, easy off, your feet won’t get sweaty because there’s not much material, and they’re available in a veritable rainbow...
UCLA Researchers Develop 3D Printed Pen that May Help Detect Parkinson’s Disease
Diagnosing Parkinson’s disease is difficult. Often, early symptoms of the progressive neurological condition may be overlooked, or mistaken for signs of aging. Early diagnosis can help save lives and improve...
Printing Money Episode 30: Q1 2025 Public 3D Printing Earnings Review with Troy Jensen, Cantor Fitzgerald
Printing Money is back with Episode 30, and it’s that quarterly time, so we are happy and thankful to welcome back Troy Jensen (Managing Director, Cantor Fitzgerald) to review the...
Heating Up: 3D Systems’ Scott Green Discusses 3D Printing’s Potential in the Data Center Industry
The relentless rise of NVIDIA, the steadily increasing pledges of major private and public investments in national infrastructure projects around the world, and the general cultural obsession with AI have...