Barrow Neurological Institute: 3D Printed Spine Models Used for Residency Training
 Researchers from the Barrow Neurological Institute in Phoenix, Arizona, came together recently to author ‘The Barrow Biomimetic Spine: Face, Content, and Construct Validity of a 3D-Printed Spine Model for Freehand and Minimally Invasive Pedicle Screw Insertion,’ exploring the use of a new surgical training platform.
Researchers from the Barrow Neurological Institute in Phoenix, Arizona, came together recently to author ‘The Barrow Biomimetic Spine: Face, Content, and Construct Validity of a 3D-Printed Spine Model for Freehand and Minimally Invasive Pedicle Screw Insertion,’ exploring the use of a new surgical training platform.
For the study, five models were examined for use in training with simulation of both freehand and percutaneous pedicle screw placement. Three of them were designated for freehand pedicle screw training (models A-C) and two for MIS pedicle screw training (models D and E), with all models evaluated and then scored by spine surgeons.
As in so many other fields and industries, 3D printing also brings myriad benefits to medicine and specifically, the world of medical models. They can be made easily, affordably, and quickly. 3D printed medical and surgical models can also be accompanied by inherent haptic feedback, which is often not available with computer based surgical models. The authors point out that while 3D printing has been ‘received enthusiastically by several neurosurgical subspecialties,’ there has been a ‘deficit of research’ into its use for both simulation and training practices.

Three-dimensional rendering of the L3-L5 vertebral bodies taken from a computed tomogram of a patient with normal lumbar spine anatomy. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
With the inception of the 3D printed Barrow Biomimetic Spine model, the team hopes to fill this gap in training with an affordable and anatomically correct device.
“This model has been demonstrated in previous studies to provide high-fidelity gross anatomy, fluoroscopic anatomy, biomechanical performance of pedicle screws, and range of motion for short spinal segments,” state the researchers. “These properties are prerequisites for any high-fidelity training model of pedicle screw insertion, one of the key surgical skills required of any spine surgeon.”
All models were created with Meshmixer software, imported back into Simplify3D software, and then 3D printed on a FlashForge Creator Pro. Affordability is substantial in the fabrication of these models too, which cost around $50-$70. Testing was performed in random order, and directly afterward, each surgeon completed a survey regarding their thoughts on face, content, and construct validities of the models.

(A) Screenshot from 3D printing plan for model A. The L3-L5 vertebral bodies are arranged in the correct anatomical orientation and placed inside a block of material that will simulate the soft tissue exposure of an open posterior approach. (B) Photograph of the 3D-printed model that resulted from the printing plan in Figure 2A. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.

Photograph of model B, which contains the 3D-printed L3-L5 vertebral bodies (green) set into a silicone rubber (pink) up to the level of the transverse processes to show the anatomical landmarks typically visible during an open posterior approach. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
Model C was evaluated overall to have the highest scores in all areas out of the five models; in fact, the surgeons gave that particular model ‘nearly perfect scores’ in the areas of content and construct validity. Model D was given the highest scores in the areas of face, content, and construct validity, although surgeons complained that the soft tissue material was not realistic to work with.
“Since the writing of this article, new work has begun on creating a more realistic soft tissue and operating room environment in hopes of increasing the face validity of these models,” states the research team. “We have also expanded the models to include synthetic thecal sacs and electrically conductive nerve roots. Models of the cervical spine are also under development and include synthetic vertebral arteries in addition to the bony and ligamentous tissue of the spinal column and synthetic thecal sac.”
The team says that they can now use data from the study as a baseline and develop more improved 3D printed models. They state that the models are getting regular use by the residents, from the junior to senior level.
“Our findings have enabled the further development of numerous surgical spine models that are increasingly used by neurosurgery residents interested in improving their surgical skills outside of the operating room. Models like these are likely to become more important to residency and fellowship training programs in the new era of work-hour restrictions,” concluded the researchers.
“With the introduction of the 80-hour resident work week, improvement of off-site tools for resident education are in increasing demand. In neurosurgical practice, 3D printed models for simulation of spinal procedures hold great promise. The Barrow Biomimetic Spine, with incorporated vascularization, improves on existing synthetic spinal models in face, content, and construct validation measures.”
Surgical models and guides have been used in countless other training exercises and surgeries too, including knee replacements, reconstructive jaw surgery, and even shoulder surgeries and hip surgeries. Both patients and their families can also benefit from medical models in becoming educated about the condition. Find out more about use of 3D printing in medical models for the biomimetic spine here.
What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.

Radiographs of model E that demonstrate the negative projection of the vertebral bodies that results from using silicone rubber as a synthetic soft tissue. (A) Anteroposterior view of model E with a Jamshidi needle (Becton Dickenson and Co, Franklin Lakes, NJ, USA) placed in the right L3 pedicle. (B) Lateral view of the same model with a pedicle screw in the right L3 pedicle. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
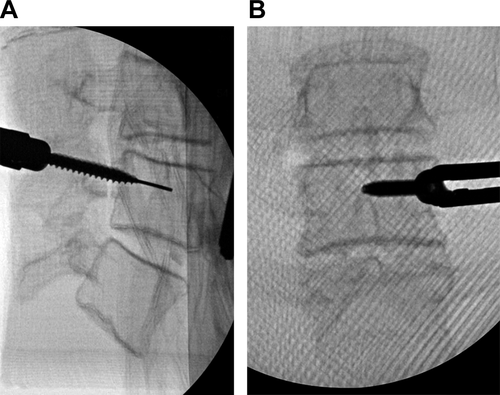
Radiographs of model D that demonstrate the higher fidelity radiographic views of the vertebral bodies when using the Gel-Lay as a synthetic soft tissue. (A) Lateral view of a percutaneous pedicle screw placement in the left L4 pedicle. (B) Anteroposterior view of the same model with a pedicle screw being placed in the left L4 pedicle. Used with permission from Barrow Neurological Institute, Phoenix, Arizona.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Srini Kaza Discusses Strategically Scaling Align’s “Smile-Changing” 3D Printed Aligners
Align Technology‘s Invisalign is a revolutionary method to get you the smile you want through 3D printing. It is also a hugely popular process to go through, a $4 billion...
Analysis: Additive Manufacturing Strategies Spotlights Vertical Value Creation
A slowdown in the industry and particularly a tightening of access to capital following the additive manufacturing (AM) industry’s peak special purpose acquisition company (SPAC) phase in early 2021 is...
Department of Defense Awards PROTECT3D $1.3M for Custom 3D Printed Braces
Custom prosthetics company PROTECT3D has secured a $1.3M Department of Defense (DoD) Small Business Innovation Research contract to develop a platform for creating custom braces for soldiers. The PROTECT3D Platform...
AMS 2025 Highlights Big Changes in 3D Printing with Pivotal Speakers and Panels
2023 was filled with excitement around the potential mergers being pursued by industry stalwart Stratasys (Nasdaq: SSYS), leading to some of the most insightful conversations imaginable at Additive Manufacturing Strategies...










































