Korea: Researchers 3D Printing Tracheas with Epithelial Cells & Chondrocytes
Korean researchers have been experimenting further in the bioprinting of tracheal implants, publishing recent results in ‘Trachea with Autologous Epithelial Cells and Chondrocytes.’ The team of scientists details their use of polycaprolactone and hydrogel mixed with nasal epithelial and auricular cartilage cells.
After bioprinting an artificial trachea with these materials and tissue, they transplanted them into 15 rabbits, six of which were a control group. The goal was to find a way to overcome tracheal problems due to tumors, the most common of which are adenoid cystic carcinomas and squamous cell carcinomas. Previously there have been substantial challenges in creating viable tracheas that are anatomically correct and can produce a ciliated epithelium. Issues have arisen with infection, implants that become dislodged, have migrated, or experienced obstruction.
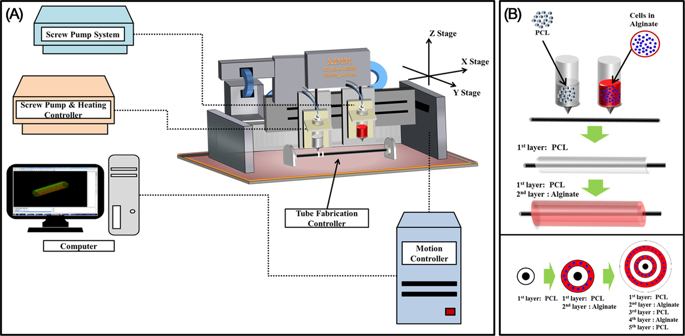
System components and bioprinting process. (A) Schematic graph of 3D bio-scaffold plotting system. (B) Detailed fabrication process of artificial trachea using bio plotting system. First, porous PCL layer; second, cell-laden alginate; third, non-porous PCL layer; fourth, cell-laden alginate; and fifth, porous PCL printing on tube type module.
“The most actively studied method for fabricating artificial trachea is tissue engineering, and biodegradable synthetic polymers are used to make tubular scaffolds,” state the scientists. “A scaffold made using tissue engineering tends to have a smooth vascularization and less obstruction when compared to foreign materials, allografts, and autogenous grafts. Currently, studies are underway in various directions, including those that regenerate tracheal epithelium.”
Materials similar to tracheal cartilage include polycaprolactone (PCL), polyglycolic acid (PGA), polylactic acid (PLA), and poly(lactic-co-glycolic) acid (PLGA). These have all been used in 3D printing and ongoing research. In this study, the researchers 3D printed tracheas as close to the human tracheal structure as possible and assessed them over a 12-month period.
“This study is the first to treat tracheal lesions using 3D printed artificial trachea with autologous epithelial cells and chondrocytes, and there have been few studies examining long-term effects of artificial tissue over one year,” state the researchers. “Respiratory epithelia and cartilage chondrocytes, which play the most important role in the structure of the trachea, were cultured to produce hydrogel for bio-printing. An artificial trachea was produced using 3D printing with a biodegradable polymer. In addition, an artificial trachea was implanted in a well-known trachea scaffold partial resection model, and respiration scoring, x-ray, computed tomography (CT), endoscopy, and histological examination were performed.”

3D printed alginate hydrogel and artificial trachea. (A) Alginate hydrogel being extruded at 300 um nozzle. (B) Optical image of 3D alginate cube type (16 × 16 × 2 mm3). The higher concentration of alginate hydrogel providing more precise and porous cube type. (C) Gross image of the artificial trachea fabricated using a 3D bio-printer. (D) Scanning electron microscopic image. From the bottom: first, porous PCL layer; second, epithelial cell layer; third, non-porous PCL layer; fourth, chondrocyte layer; and fifth, porous PCL layer are clearly seen. (E–G) Fluorescent microscopic images using green dye for the epithelial cells (E) and red dye for chondrocytes (F); and merged image (G) reveals that the 2 hydrogel layers are completely separated.
The emphasis was on creating epithelium and cartilage regeneration, with nasal cells in the internal layer and auricular cartilage cells in the external layer. The researchers stated, however, that the use of two different types of cells in implants has been challenging.
“Nasal epithelial cell cultures were used to transplant trachea-like ciliated epithelial cells without damaging the tracheas of the rabbit before surgery, and epithelial cells were successfully formed in all the experimental groups. We believe that this is the effect of transplantation of epithelial cells into scaffolds and that there is a direct correlation with early survival rate,” stated the researchers.
For these types of bioprinted transplants, cartilage is vital. No formation of cartilage was noted in the 3-month group, although there was some growing at 6 and 12 months.
“Other studies using rabbit ear chondrocytes for tracheal grafts also revealed a cartilaginous island similar to that of the native trachea at 6 months, but it did not produce a complete c-shape,” stated the researchers.
They ended the research realizing that greater methods should be studied to find ways to reduce the amount of time it takes for cartilage regeneration. Further, in conclusion, the research team states:
“In this experiment, an artificial trachea was constructed using a 3D bio-printing technique and was successfully transplanted with two different types of autogenously isolated cells, epithelial cells and chondrocytes. The artificial trachea was successfully engrafted into the partially resected trachea, resulting epithelialization and formation of cartilage islet. This resulted thirteen of fifteen animals’ survival until 12 months without specific respiratory signs in the experimental group, while the control group showed only four of six animals’ survival. Our research could inform that our 3D-printed artificial graft containing autogenous cells is stable enough for a long time about a year and could provide a platform to apply with several different types of cells or suitable biomaterials to treat tracheal diseases.”
The trachea has been the object of bioprinting in the last five years, improving the lives of patients like babies with 3D printed trachial splints, a child in Ireland now able to breathe more normally despite pulmonary alveolar proteinosis, and other medical innovations such as tracheal implants without tissue scaffolds. Find out more about this particular study here.
What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source / Images: Experimental Tracheal Replacement Using 3-dimensional Bioprinted Artificial Trachea with Autologous Epithelial Cells and Chondrocytes]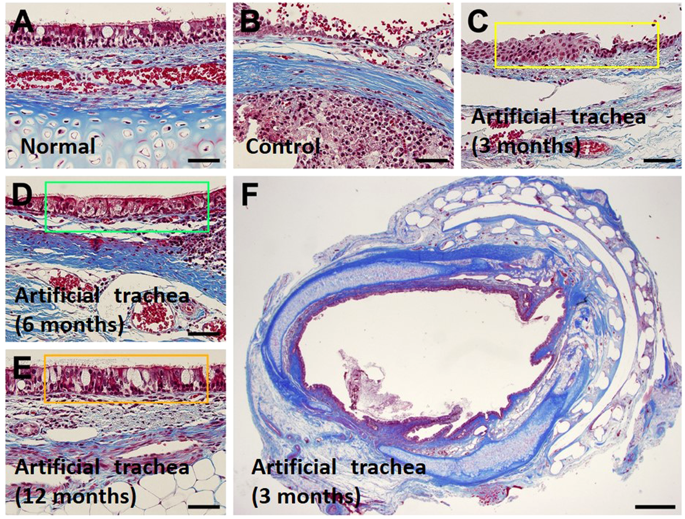
Histopathologic images of epithelial regeneration. Compared with the normal tracheal epithelium (A), the control group (animal no. 5) does not show epithelial regeneration (B). However, the experimental group shows epithelial regeneration at 3 months, and 1 animal shows incomplete epithelial regeneration with squamous metaplasia (C, animal no. 8). The animals at 6 (D, animal no. 14) and 12 months (E, animal no. 21) show complete epithelial cell regeneration. (F) A whole trans-sectional image at 3 months in the experimental group (animal no. 9) also shows complete epithelial regeneration. (Masson’s trichome staining, the bars in subpanels A-E indicate 50 µm and that in subpanel F indicates 1 mm) The epithelial regeneration was pointed with green and yellow boxes in (D,E).
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Mikhail Gladkikh on Digital Inventory: “Think of It as Netflix for Manufacturing”
As manufacturers continue looking for ways to reduce supply chain risk, additive manufacturing (AM) is increasingly being discussed as more than just a production tool. Across aerospace, energy, defense, and...
ROBOZE Buys Dimanex Assets to Build “Physical AI” Platform
Dutch firm Dimanex got its start as an MRO platform for the railways. The company had a contract with the Dutch Army in 2018, and later that year signed one...
MORSAN and LEHVOSS Work on 3D Printing for Food and Beverage
For many years, LEHVOSS has made specialized 3D printing materials such as high-temperature polyamide and high-flow PEEK. Now it has teamed up with MORSAN to develop a 3D printing offering...
3D Printing & Drone Dominance: Speed, Performance, and Derisking the Supply Chain
A shift is underway in drone manufacturing. Government programs like the U.S. Department of War’s Drone Dominance, a $1.1 billion effort to deliver low-cost, one-way attack (OWA) sUAS at scale,...















































