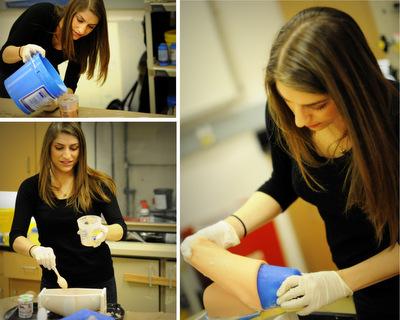
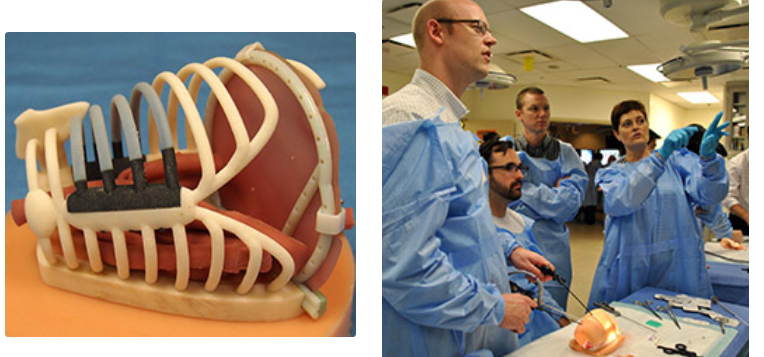
One of the difficulties of training new entrants into the medical field is the leap from text knowledge to hands on care. One of the ways to approach that transition in health education is through the provision of models as a buttress, with students practicing what they have learned on plaster or plastic replicas as part of a long process of qualifying for the honor of practicing on their own. There is no substitute for the experience gained during actual procedures with live patients, but in continuing efforts to make the leap from pre-practice, to practice, cover as small a gap as possible, 3D printing has been utilized to create exquisitely lifelike models.
The recent usage of this increasingly common technique for model production is especially important in the area of pediatric surgery. Much of the preparation for practicing surgery comes through observation and assistance in the operating room. However, in the case of pediatric patients, their diminutive size makes easy observation a pipe dream and their delicate states require extreme precision and mastery from their surgeon.
It was for these reasons that associate professor in Surgery and Medical Education at Northwestern, Dr. Katherine Barsness looked for help from the engineers at the University’s Feinberg School of Medicine’s Innovation Lab and the McCormick School of Engineering and Applied Sciences. She explained the difficulties she was looking to address through the creation of model rib cages to be used in the simulations that pediatric surgeons undergo as part of their training:
“The overwhelming majority of surgeons just train in the operating room. Everybody has a learning curve when they’re developing new skills, a time when they make mistakes while trying to master a certain technique. Unfortunately, a learning curve places patients at risk.”
 In order to help flatten the learning curve to the greatest extent possible, she worked with the team from Feinberg to create life-sized models of an infant’s rib cage that could be used over and over again. The final step came when Barsness combined the 3D printed structure with tissue taken from cows in order to recreate both the look and feel the student would one day experience during real world surgery. She described the benefits of this type of simulation based education in preparing students for practice:
In order to help flatten the learning curve to the greatest extent possible, she worked with the team from Feinberg to create life-sized models of an infant’s rib cage that could be used over and over again. The final step came when Barsness combined the 3D printed structure with tissue taken from cows in order to recreate both the look and feel the student would one day experience during real world surgery. She described the benefits of this type of simulation based education in preparing students for practice:
“Simulation-based education is very, very new in medical education overall. So during my training, we didn’t really do anything in the simulation lab. We learned by what’s called the classical Halstedian model, which is: see one, do one, teach one. [This] is very real. So, the muscle is real muscle, but we also have the constraints of a rib cage, which is created using the 3D printer. So this hybrid model gives you the best of both worlds.”
While this may seem like an obvious, common-sense approach to take in medical education, Barsness sees a number of obstacles that must be overcome before it becomes a regular part of medical training:
“First is dedicated time for education outside the operating room. We need programs to let their trainees leave clinical duties for dedicated simulation-based education. Second, there are very few pediatric surgeons in the world who are trained to conduct this type of education…acceptance is predicated on data. So our next step is to show that using the simulation models really does improve physicians’ performances in the operating room.”
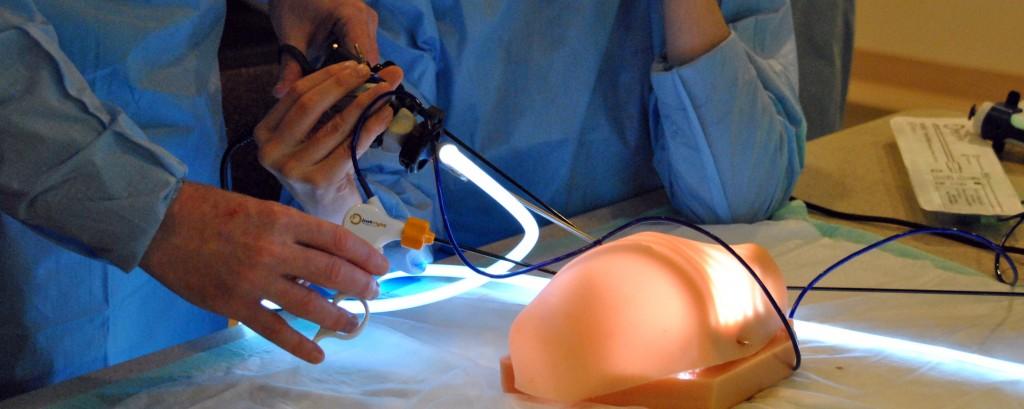 A final hurdle that must be passed is the investment in the technology that will be required in order to produce these models as needed. Each model costs only approximately $200 to produce, but the machinery and expertise required are a much more expensive initial outlay. Given the friendly funding environment created by 3D printing, this may no longer be as great of a difficulty to surmount as it once was.
A final hurdle that must be passed is the investment in the technology that will be required in order to produce these models as needed. Each model costs only approximately $200 to produce, but the machinery and expertise required are a much more expensive initial outlay. Given the friendly funding environment created by 3D printing, this may no longer be as great of a difficulty to surmount as it once was.
Demonstrating that the models are actually improving physician’s abilities to carry out their procedures would most likely open a well of funding from both grant giving institutions and private individuals. After all, it’s hard to resist the plea for help with something that would improve the health of a child. Let’s hear your thoughts on the importance of 3D printing within pediatric surgery in the 3D Printed Rib Cage forum thread on 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Further Understanding of 3D Printing Design at ADDITIV Design World
ADDITIV is back once again! This time, the virtual platform for additive manufacturing will be holding the first-ever edition of ADDITIV Design World on May 23rd from 9:00 AM –...
3D Printer Maker EVO-tech Reborn as NEVO3D — Once More With Feeling
EVO-tech was a 3D printing service and original equipment manufacturer established in 2013 and based in Schörfling am Attersee, Austria. The company produced high-quality material extrusion systems featuring linear bearings,...
3D Systems Brings 3D Printed PEEK Cranial Implant to the U.S. with FDA Clearance
For more than 10 years, 3D Systems (NYSE:DDD) has worked hand-in-hand with surgeons to plan over 150,000 patient-specific cases, and develop more than two million instruments and implants from its...
CDFAM Returns to Berlin for Second Annual Symposium
The second CDFAM Computational Design Symposium is scheduled for May 7-8, 2024, in Berlin, and will convene leading experts in computational design across all scales. Building upon the first event...