Health professionals who treat burn victims are acutely aware of the necessity to treat burn injuries, particularly severe ones, as rapidly as possible. As one journal article explains it, “In severe burn injuries where both the epidermal and dermal layers of skin are destroyed, prompt wound closure is critical for favourable [sic] patient outcomes and reduced mortality rates.”
A team of biomedical and mechanical engineering graduate students at the University of Toronto have developed what may at the least be considered a preliminary–but certainly extremely technologically advanced–solution to the problem of critical, temporal health intervention for burn patients. For their PrintAlive Bioprinter, which, according to a recent press release, is “a 3D printer that produces artificial skin grafts for burn victims,” Arianna McAllister and Lian Leng have been awarded “the top prize in the Canadian leg of the 2014 James Dyson Award, an international student product design contest.”
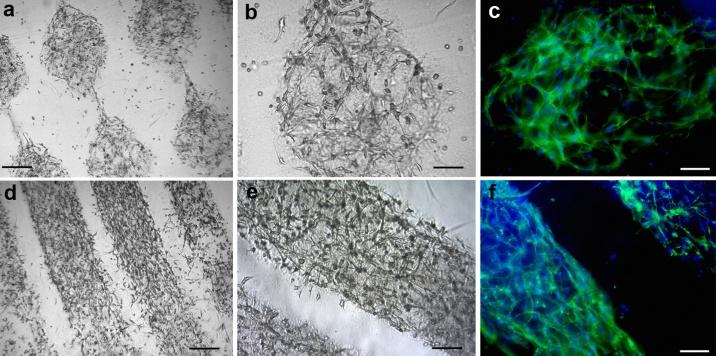
According to its inventors, the PrintAlive Bioprinter “could significantly speed burn victim recovery time.” It does so by making it possible to print what McAllister and Leng refer to as “a kind of living bandage.” The bioprinter does not create 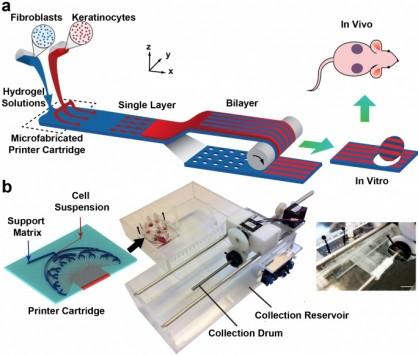 “a human skin graft in the traditional sense.” What it does is construct a 3D, skin-like material–”a biopolymer infused with human keratinocytes,” the most common cells in the epidermis (comprising 90%), the outer layer of skin tissue, and “fibroblasts,” which maintain the structural integrity of connective tissues.
“a human skin graft in the traditional sense.” What it does is construct a 3D, skin-like material–”a biopolymer infused with human keratinocytes,” the most common cells in the epidermis (comprising 90%), the outer layer of skin tissue, and “fibroblasts,” which maintain the structural integrity of connective tissues.
3D printing is especially useful, explained the innovative graduate student team, in mimicking the “hierarchical architectures” of tissues “to organize multiple cell types and substructures.” “This spatial organization,” they noted, “is critical to the biological function of the tissue.” Because the bioprinters that are currently available on the commercial market were inadequate in terms of manufacturing the the complex, layered material McAllister and Leng aimed to produce, they decided to design their own bioprinter to surmount the limitations of existing technology.
The two drew from previous bioprinting technology to create a new device that would facilitate “the formation of cell-populated wound dressings that accurately reproduce key features of human skin in a scalable and high-throughput format.” The process they developed, called “microfluidic cartridge-based technology,” allows the bioprinter to produce “hydrogel sheets with multiple cell types and precisely controlled graft thickness, structure, and composition.”
To reiterate, this isn’t artificial human skin being produced but, rather, a high-tech bandage or, what the inventors call “cell-populated sheets” that are applied to damaged skin (burns) to expedite treatment and healing. McAllister and Leng have tremendous aspirations for improving this technology, noting “As we move toward more complex animal models, we are hoping that our cell-populated sheets and bioprinting approach can one day be used as on-demand custom grafts for patients with severe burns.”
In the interim, the PrintAlive Bioprinter in many ways exceeds current technology. “Compared to the current standard of care,” said McAllister, “this would significantly reduce the amount of donor cells needed and the overall printing and culture time before application to the wound.” It is her hope that, with this new printing process, patients’ own cells could be used, thereby eliminating “immunologic rejection, and the need for painful autografting and tissue donation.”
Could this bioprinter be the future of treating a variety of injury to the skin? Discuss this fascinating new machine in the PrintAlive Bioprinter forum thread on 3DPB.com. Below you will find a video explaining this printer in further detail.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Reinventing Reindustrialization: Why NAVWAR Project Manager Spencer Koroly Invented a Made-in-America 3D Printer
It has become virtually impossible to regularly follow additive manufacturing (AM) industry news and not stumble across the term “defense industrial base” (DIB), a concept encompassing all the many diverse...
Inside The Barnes Global Advisors’ Vision for a Stronger AM Ecosystem
As additive manufacturing (AM) continues to revolutionize the industrial landscape, Pittsburgh-based consultancy The Barnes Global Advisors (TBGA) is helping shape what that future looks like. As the largest independent AM...
Ruggedized: How USMC Innovation Officer Matt Pine Navigates 3D Printing in the Military
Disclaimer: Matt Pine’s views are not the views of the Department of Defense nor the U.S. Marine Corps Throughout this decade thus far, the military’s adoption of additive manufacturing (AM)...
U.S. Congress Calls Out 3D Printing in Proposal for Commercial Reserve Manufacturing Network
Last week, the U.S. House of Representatives’ Appropriations Committee moved the FY 2026 defense bill forward to the House floor. Included in the legislation is a $131 million proposal for...