The day of an ultrasound can be one of the most exciting pre-birth connections a parent makes with his/her child. Even though the pictures don’t hold a candle to those taken outside of the womb, there is something amazing about giving form to the life growing in the womb, and they are the first glimpses of the tiny being who will change your world forever. In some cases, however, the information provided by the ultrasound goes beyond the simple introduction of baby to parent and reveals important information about problems that need medical attention. This was the case with an ultrasound performed on expectant mother Caitlin Veitz when she was 20 weeks pregnant.
 The ultrasound she received that day would fill the parents with fear and anxiety for their child as it revealed that their baby’s heart was growing outside of the chest wall, a condition that is so rare, it was difficult for the doctors to offer reasonable assurances that they could address the problem. Luckily for her and baby-to-be Kieran, Veitz had access to some of the most highly skilled doctors in the world through the Mayo Clinic. The medical team attending to this special case needed to do everything possible to prepare what Kieran would need, as her very survival was at stake.
The ultrasound she received that day would fill the parents with fear and anxiety for their child as it revealed that their baby’s heart was growing outside of the chest wall, a condition that is so rare, it was difficult for the doctors to offer reasonable assurances that they could address the problem. Luckily for her and baby-to-be Kieran, Veitz had access to some of the most highly skilled doctors in the world through the Mayo Clinic. The medical team attending to this special case needed to do everything possible to prepare what Kieran would need, as her very survival was at stake.
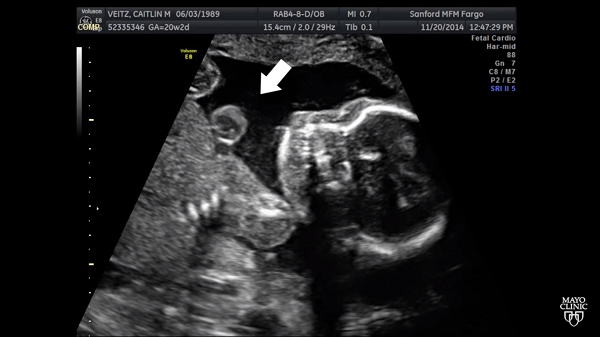 An early step in the preparation consisted of the creation of a 3D printed model of Kieran’s anatomy developed from ultrasound data using the Materialise Mimics Innovation Suite. Dr. Jan Matsumoto, radiologist and co-director of the Mayo Clinic’s 3D Anatomic Modeling Lab, then color coded and segmented all of Kieran’s major organs and determined the location of her body in relationship to the placenta, uterus, heart, and liver. It was determined, after working with a life size 3D printed model, that in fact Kieran’s liver and intestines were developing on the outside of her body as well as her heart.
An early step in the preparation consisted of the creation of a 3D printed model of Kieran’s anatomy developed from ultrasound data using the Materialise Mimics Innovation Suite. Dr. Jan Matsumoto, radiologist and co-director of the Mayo Clinic’s 3D Anatomic Modeling Lab, then color coded and segmented all of Kieran’s major organs and determined the location of her body in relationship to the placenta, uterus, heart, and liver. It was determined, after working with a life size 3D printed model, that in fact Kieran’s liver and intestines were developing on the outside of her body as well as her heart.
 The multiple surgeries that would be necessary to remedy these anomalies presented grave danger of over-stressing the little girl, and so a decision was made to focus first on safely moving the heart back into her chest cavity. Using the model, the medical team prepared for a post-partum operation to occur after a C-section.
The multiple surgeries that would be necessary to remedy these anomalies presented grave danger of over-stressing the little girl, and so a decision was made to focus first on safely moving the heart back into her chest cavity. Using the model, the medical team prepared for a post-partum operation to occur after a C-section.
Even this planning wasn’t sufficient as Veitz’s blood pressure rose dramatically and the baby’s vital signs weakened several days before the planned C-section, and an emergency surgery had to be performed in order to deliver the baby. The Mayo Clinic is equipped to handle just such alarming developments and within 90 minutes had assembled a team of 60 doctors and nurses who would be involved with the entire process from birth to heart surgery. The delivery itself took place in the cardiac surgery operating room, not a typical location, but one that was chosen because of the immediate surgical needs the baby would bring with her.
 Despite the early arrival of Kieran, the detailed preparation conducted by the medical team in relation to her particular condition meant that despite the change in date, they were well versed in the intricacies of the procedure and her surgery was a categorical success. After four and a half months of treatment and observation in the pediatric intensive care unit, it was finally time for Kieran’s parents to bring her home. Currently six months old, Kieran is on par with growth expectations for babies her age, and what could have been a tragedy is a story of strength, technology, and a bright future for a beautiful little girl.
Despite the early arrival of Kieran, the detailed preparation conducted by the medical team in relation to her particular condition meant that despite the change in date, they were well versed in the intricacies of the procedure and her surgery was a categorical success. After four and a half months of treatment and observation in the pediatric intensive care unit, it was finally time for Kieran’s parents to bring her home. Currently six months old, Kieran is on par with growth expectations for babies her age, and what could have been a tragedy is a story of strength, technology, and a bright future for a beautiful little girl.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
U.S. Navy Lab Uses 3D Printing to Reduce Tooling Lead Time By Over 90%
The F-35 Lightning II Joint Program Office (JPO), responsible for life-cycle management of the key fifth-generation joint strike fighter (JSF) system used by the U.S., its allies, and its partners,...
Etsy Design Rule Change Reduces Selection of 3D Printed Goods
Online marketplace Etsy has implemented a rule change requiring all 3D printed goods on the site to be original designs. The update to the site’s Creativity Standards states, ¨Items produced using...
Honeywell Qualifies 6K Additive’s Nickel 718 for 3D Printed Aerospace & Defense Parts
6K Additive is renowned for manufacturing sustainable additive manufacturing (AM) powder, and offers a wide portfolio of premium metal and alloy powders that include titanium, copper, stainless steel, and nickel,...
MetalWorm Sells WAAM Systems to Research Institutes in Brazil and Malaysia
Turkish WAAM firm MetalWorm has sold a system in Malaysia and another in Brazil. This is an excellent example of a few emerging trends in additive. Firstly, WAAM was experimented...

































