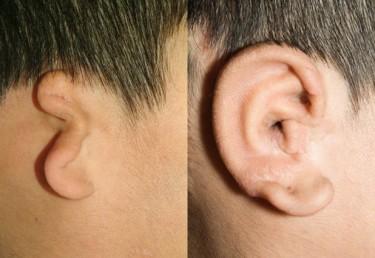
Practice Makes Perfect: Researchers Create 3D Printed Silicone Models for Pediatric Ear Reconstruction
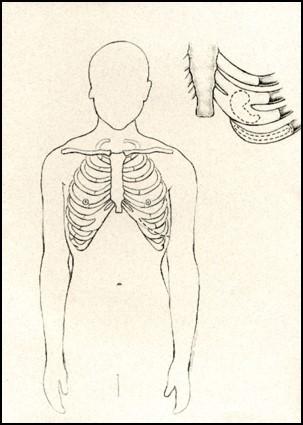
Surgeons use portions of the ribs to reconstruct pediatric ear cartilage. Diagram: University of Washington
Most of us take for granted the ability to hear, to be able to hear ourselves speak and to do so clearly, and even more aesthetic concerns like being able to wear earrings normally, and to well…not think about our ears much on a daily basis or how they appear to others.
For some who face a variety of issues though, as well as deformities, reconstruction is on their minds constantly due to painful health conditions–and painful and very real self-consciousness. It’s left to medical professionals to provide help in performing intricate surgeries, requiring intricate practice ahead of time–especially when it comes to pediatric surgeries aimed at reconstructing delicate ear cartilage in tiny bodies.
And since the beginnings of formal medical training, finding suitable materials to train with has been not only challenging, but even comical as students have been very creative in practicing on everything from traditional cadavers to garden vegetables. This is true for all areas of surgery, but thanks to digital design and 3D printing, those days may be coming to an end, which is good for all involved.
By now, we have followed numerous cases documenting how 3D printing is going to change the game for both students and seasoned surgeons who need to train for surgeries. With the advent of progressive fabrication, today’s researchers are able to make a range of materials that can help, with 3D prints made from multi-material resources to simulate skin for practicing in sutures to now, 3D printed silicone used to practice for auricular reconstruction purposes. Even bioprinting is being explored for the actual 3D printing of ears themselves to be used in the future for transplants.
For now though, practice makes perfect–and there has simply never been a material available to allow repetitive training for ear reconstruction surgeries to happen easily. With that issue in mind, studies are now ongoing regarding the use of silicone in 3D printing to fabricate models for training in reconstruction of the ear, and specifically in pediatrics.
University of Washington researchers have been able to make the 3D models after scanning CTs to make patient specific resources for practice in surgeries, called auricular reconstruction, where ribs are used to rebuild ear cartilage. Once they 3D printed the silicone models made from the CTs, several experienced surgeons were recruited to use the materials prior to surgery for carving and plotting out reconstruction. They deemed the 3D printed silicone models as training devices they would most definitely prefer to use, and would also recommend them as formal training tools for student doctors.
“It’s a huge advantage over what we’re using today,” said Angelique Berens, a UW School of Medicine otolaryngology-head and neck surgery resident.
“You literally take a bar of Lever 2000 while the attending is operating and you carve ear cartilage,” she continues. “It does teach you how to get the shape right, but the properties are not super accurate–you can’t bend it, and sewing it is not very lifelike.”
Berens and her colleagues have just put their findings together for an oral presentation they gave recently at the 119th American Academy of Otolaryngology — Head and Neck Surgery Conference, held in Dallas. (Co-authors on the presentation were Sharon Newman, Research Assistant, University of Washington, Department of Bioengineering; Craig Murakami, M.D., Clinical Associate Professor, University of Washington/Virginia Mason Medical Center; Kathleen C. Sie, M.D. Director, Childhood Communication Center, University of Washington; and David A. Zopf, MD, MS, Assistant Professor, Otolaryngology–Head and Neck Surgery, Pediatric Division, University of Michigan.)
Considering the issues involved with properly training students–and even professionals who are more seasoned–for harvesting rib pieces and then actually integrating them it into the small ears of children, it’s important to have as authentic a procedure for practicing as possible, and the University of Washington researchers think they may have found it.
Currently the waiting lists for children to have the reconstructive surgery are as long as a year at Seattle Children’s, reports Kathleen Sie, professor of otolaryngology-head and neck surgery and director of the Childhood Communication Center at the hospital. She too understands that the issue has previously been in challenges to train for such a procedure, resulting in few surgeons who can or will perform the surgery.
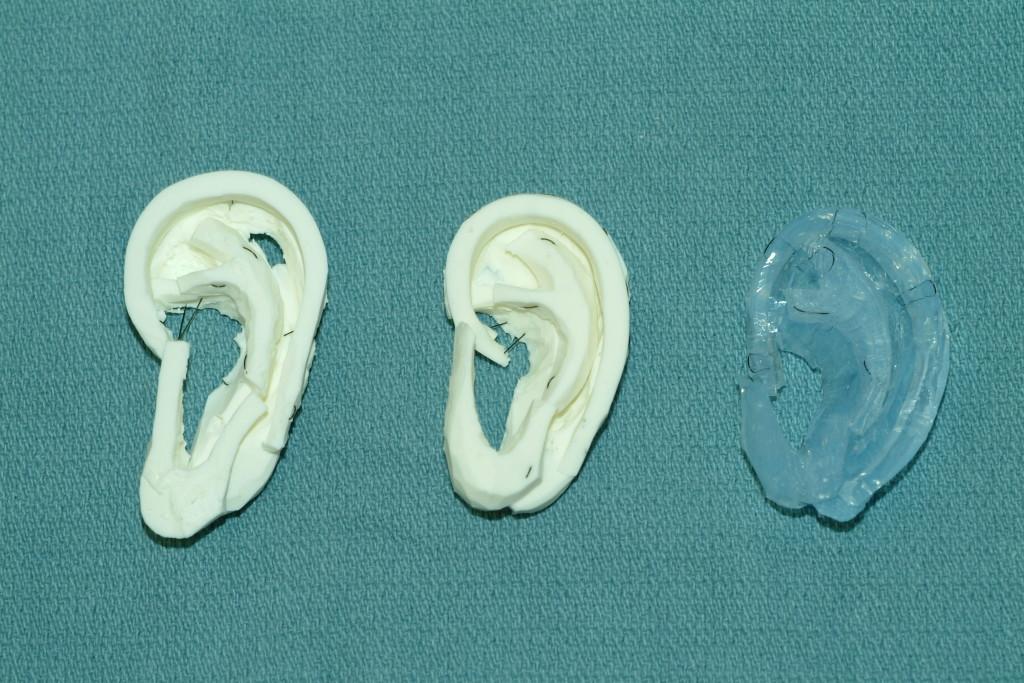
In testing, surgeons preferred training with the 3D printed models, in white, over models made from dental materials (blue). Photo: University of Washington
“It’s a surgery that more people could do, but this is often the single biggest roadblock,” Sie says. “They’re hesitant to start because they’ve never carved an ear before. As many potatoes and apples as I’ve carved, it’s still not the same.”
With the emphasis on using 3D printing technology in the medical arena, this is certainly a trend sure to continue, and will help many talented new and older doctors feel more comfortable about performing procedures that previously they may have wanted to back out of or never attempt at all. As new as the research, development, and testing is for these materials, it should be interesting to see how training procedures and materials evolve–and with 3D printing that can certainly occur at a rapid speed.
Let’s hear your thoughts on this new method of creating custom ear implants in the 3D Printed Silicone Modeled Ear forum thread on 3DPB.com.
[Source: UW Today]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Gorilla Sports GE’s First 3D Printed Titanium Cast
How do you help a gorilla with a broken arm? Sounds like the start of a bad joke a zookeeper might tell, but it’s an actual dilemma recently faced by...
Nylon 3D Printed Parts Made More Functional with Coatings & Colors
Parts 3D printed from polyamide (PA, Nylon) 12 using powder bed fusion (PBF) are a mainstay in the additive manufacturing (AM) industry. While post-finishing processes have improved the porosity of...
$25M to Back Sintavia’s Largest Expansion of Metal 3D Printing Capacity Since 2019
Sintavia, the digital manufacturing company specializing in mission-critical parts for strategic sectors, announced a $25 million investment to increase its production capacity, the largest expansion to its operations since 2019....
Velo3D Initiates Public Offering in a Bid to Strengthen Financial Foundations and Drive Future Growth
Velo3D (NYSE: VLD) has been among a number of publicly traded 3D printing firms that have attempted to weather the current macroeconomic climate. After posting a challenging financial report for 2023,...