After experiencing left hip pain for over a year, a 65-year-old patient, Mr. “Smith,” was scheduled to undergo an operation to a pelvic tumor and thereafter reconstruct the area affected by the resultant bone defect. This required the creation of a patient-specific implant that would replace the bone removed during the procedure while allowing the patient to regain movement that had been lost. In the latest issue of the journal Computer Aided Surgery, the medical team, from the Department of Orthopaedics and Traumatology, Prince of Wales Hospital, Shatin, Hong Kong; and implant engineers from Mobelife NV, Leuven, Belgium, discussed the manner in which 3D technologies were used to create a superior surgical experience.
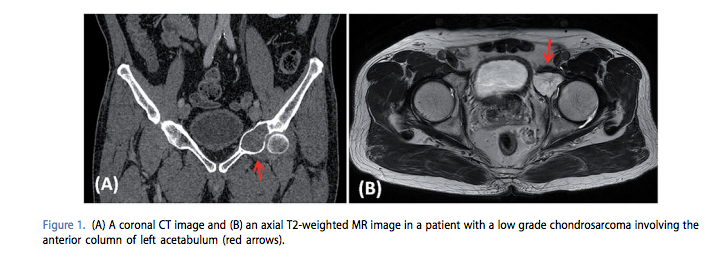 Prior to performing the operation, Mr. Smith underwent a CT guided biopsy to gather in-depth information about the affected area of his pelvis. That data was then imported into a medical image analysis software (Mimics 15.0, Materialise) which they used to develop 3D models of the tumor and surrounding bone. A further model was developed, by implant engineers at Mobelife, based on image data gathered from the right hip, which was then mirrored for the corresponding region.
Prior to performing the operation, Mr. Smith underwent a CT guided biopsy to gather in-depth information about the affected area of his pelvis. That data was then imported into a medical image analysis software (Mimics 15.0, Materialise) which they used to develop 3D models of the tumor and surrounding bone. A further model was developed, by implant engineers at Mobelife, based on image data gathered from the right hip, which was then mirrored for the corresponding region.
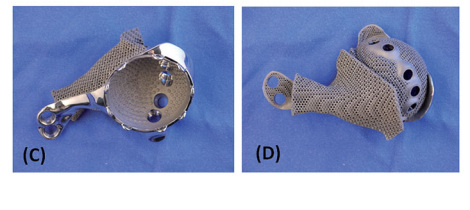
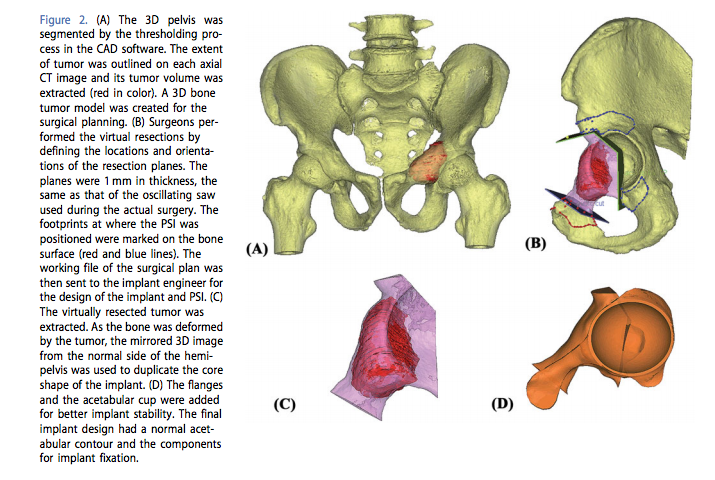 As a result of the information gathered and the power of 3D modeling, the team was able to prepare a supremely accurate model of the implant. The engineers were able to design the implant taking into consideration the surgical approach and the surrounding soft tissues to support the most successful possible outcome of the intervention. Prior to fabricating the implant, the design was biomechanically evaluated using Abaqus, a dedicated engineering software.
As a result of the information gathered and the power of 3D modeling, the team was able to prepare a supremely accurate model of the implant. The engineers were able to design the implant taking into consideration the surgical approach and the surrounding soft tissues to support the most successful possible outcome of the intervention. Prior to fabricating the implant, the design was biomechanically evaluated using Abaqus, a dedicated engineering software.
When designing a hip implant, it’s not only the shape that is of importance, but the team also had to take into account the way in which the prosthetic would be integrated with the existing bone and the need for the prosthetic to hold up under weight bearing circumstances. It’s not enough that it can allow for movement if it cannot stand up to the stress placed on it. Therefore, further evaluation was performed in response to patient-specific information regarding weight, height, and gait.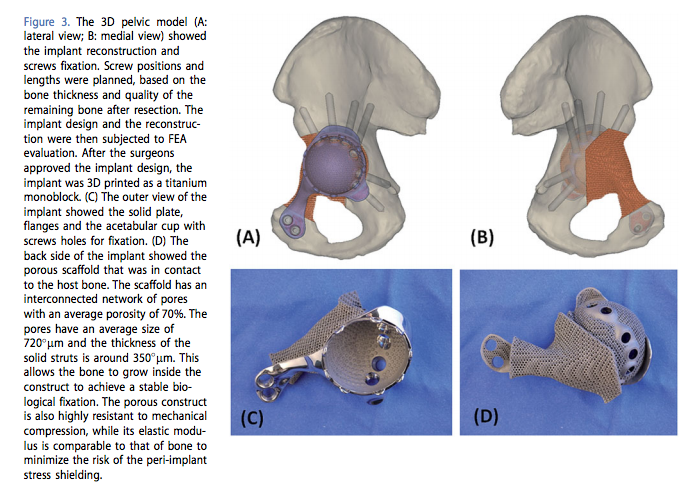
The team noted in their report:
“The stresses in the implant were assessed to ensure the implant integrity. In addition, stress values and strain distribution in the bone were investigated…Strain distribution in the bone was monitored to check that no regions were shielded from the loads. After the patient-specific FEM [Finite Element Model] evaluation, the implant design was found to have adequate implant strength. The bone loading did not exceed the safe range, causing neither bone fracture nor stress shielding.”
Once all were assured that the model was ideal, the implant was then fabricated using medical grade Ti6A14V, a titanium material. At the hospital, the implant was sterilized and prepared for use.
Placing a pre-made implant is no easy task, but in this case the team had a cheat sheet – they were able to perform a hands-on surgical rehearsal using a 3D printed model made from medical grade polyamide prior to having to perform the operation en vivo. During the surgery, bone removal has to occur within a set of very low tolerances for variation in order to ensure that the implant fits correctly. During the procedure, surgeons worked using a ‘roadmap’ to the surgery that had been created using virtual 3D images of the bone and soft tissue. In addition, a custom drill guide was created to ensure accuracy in the placement of the screws that would hold the implant in place.
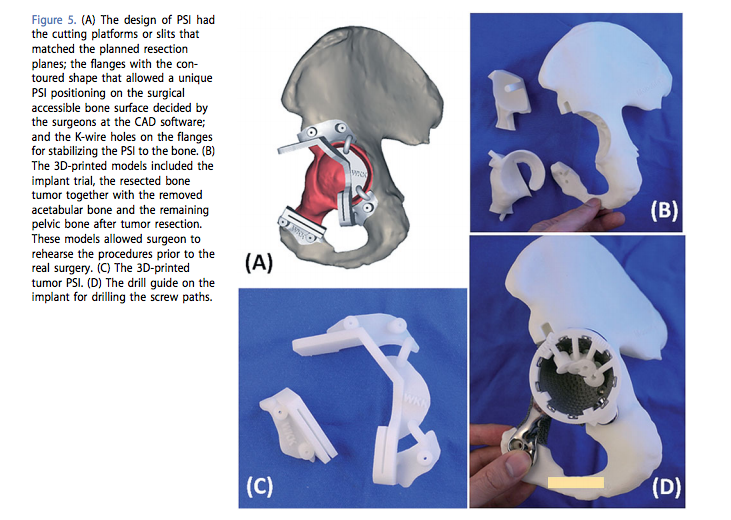
No amount of pre-planning can ever create a 100% guaranteed successful outcome, but the medical field seems to be shaving the number of unexpected events down to as near to 0 as we can hope. The ability of medical professionals to work with engineers and designers harnesses the expertise of both groups and has done a great deal to improve post-surgical outcomes. This has been demonstrated time and again in diverse cases the world over. But the general numbers of successful implementation of 3D printing in surgery sometimes overshadow the real gift that is bestowed upon a particular individual with each advance. Surgeries are being performed with better outcomes, in less time, and with decreased time and post-operative complications.
In the objective, scientific language of the medical world, the paper’s authors described the outcome for Mr. Smith: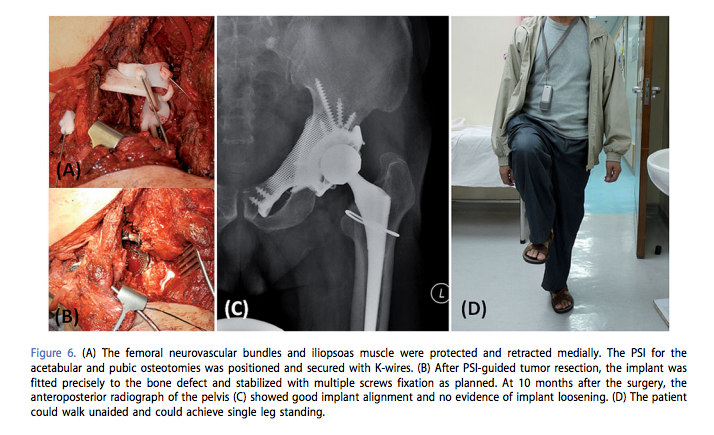
“The postoperative course was uneventful. No neurovascular complications or wound infection was noted. The patient was allowed to walk with protected weight bearing in a hip brace two weeks after surgery. He walked with full weight bearing 4 weeks after surgery. The brace was discarded at 8 weeks after had gained good hip control. By 10 months, he experienced no hip pain and could walk independently without aids. There was no evidence of tumor recurrence. The plain radiograph of the pelvis showed satisfactory implant alignment and no evidence of implant loosening.”
But what that means to Mr. Smith is the ability to move, without pain, and to participate in life’s activities once again. It may be that this is the result of advances in 3D printing technology, but it probably feels more like a miracle.
Have you heard of similar cases? Let us know where you see the future of patient-specific implants heading in the 3D Printed Pelvic Implant forum thread over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Asia AM Watch: China’s 5 Million-Printer Export Year Signals Desktop AM at Scale
For years, a lot of the discussion around China and additive manufacturing has focused on industrial competition. Can Chinese companies move into higher-end markets? Can they challenge Western machine makers...
Creality Launches Filament Maker M1 & Shredder R1, Letting Makers Reuse Waste, Cut Costs, and Create Their Own Filament
From Printing Objects to Shaping Materials Desktop 3D printing has made on-demand creation more accessible than ever. Yet one critical part of the process remains fixed: the material itself. Most...
Bambu Lab 3D Prints Miniature Playground City for Kids in China
Bambu Lab has partnered with meland to open what they describe as China’s first 3D printing creativity center for children. The new space, officially named “meland x Bambu Lab,” launched...
Bambu Lab Says 2025 Was a Breakout Year: 10 Million Monthly Users and Real Business Growth
Chinese 3D printer maker Bambu Lab reported strong results for 2025, showing that the company’s push into community and small-business 3D printing is working. The numbers suggest consumer 3D printing...