When Ariana Garcia was six weeks old, she suddenly stopped breathing. When she went limp in her father’s arms, her parents rushed her to the emergency room. They sat in the waiting room for hour after agonizing hour until finally a doctor could finally explain what was happening. Her mother, Anne Garcia, recalls that experience in great detail:
“I didn’t know if she was going to make it. We went into a conference room where our doctor sat down with us and he started drawing a picture of a heart and he explained to us that Ari had been born with a critical congenital heart defect and that the only thing that we could do was an emergency, open heart surgery to save her.”
 Compounding the difficulty of the delicate situation is the fact that every heart is different and so a surgeon doesn’t really know what they are going to find until they have opened up the heart. While clearly familiar with the basics of the human heart, not being able to study the idiosyncrasies of any particular case before the patient is on the operating table puts the surgeon at a distinct disadvantage.
Compounding the difficulty of the delicate situation is the fact that every heart is different and so a surgeon doesn’t really know what they are going to find until they have opened up the heart. While clearly familiar with the basics of the human heart, not being able to study the idiosyncrasies of any particular case before the patient is on the operating table puts the surgeon at a distinct disadvantage.
“Pediatric heart surgery is the hardest thing that I can imagine a person doing. A surgeon doesn’t know what he’s going to see until he opens a child’s chest. Every heart is different and every cardiopathy is different,” said Garcia. “A baby’s heart is the size of a walnut, and surgeons need to go in and move around structures that are as small and thin as a human hair; and they’re doing it with their own two hands. And all of this is occurring against a ticking clock.”
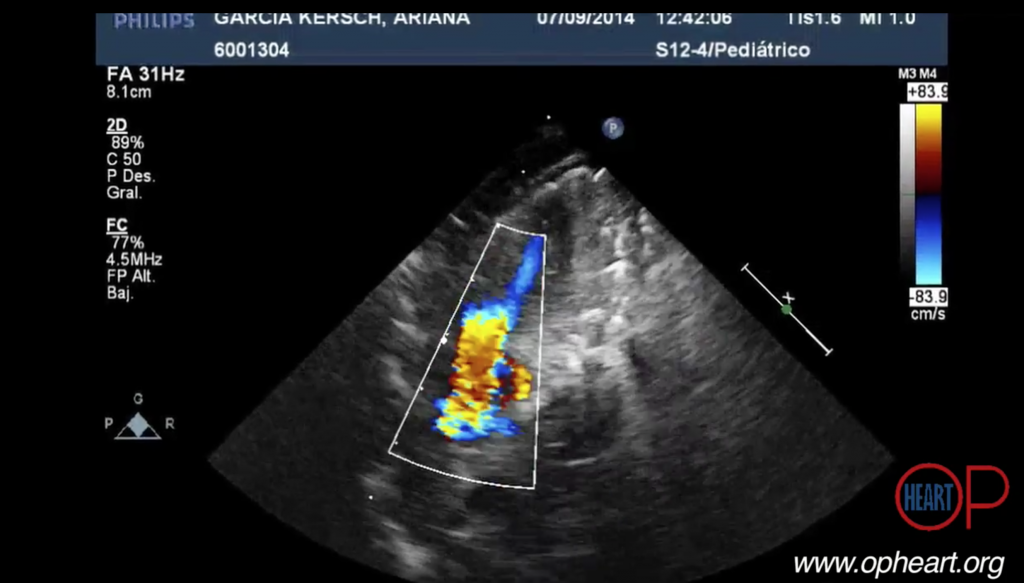 It seemed very clear to Anne Garcia that there must be a better way. When her surgeon mentioned to her that having a model of a patient’s heart to study before surgery would be worth a million dollars, Garcia decided to find out exactly what it would take to make such a thing possible. It turns out, it’s slightly less than $200. Dr. Mark Fogel, Senior Cardiologist and Director of MR at the Children’s Hospital of Philadelphia, described the incalculable value of such a model:
It seemed very clear to Anne Garcia that there must be a better way. When her surgeon mentioned to her that having a model of a patient’s heart to study before surgery would be worth a million dollars, Garcia decided to find out exactly what it would take to make such a thing possible. It turns out, it’s slightly less than $200. Dr. Mark Fogel, Senior Cardiologist and Director of MR at the Children’s Hospital of Philadelphia, described the incalculable value of such a model:
“Having something in your hands, and being able to turn it any way you want, and to be able to cut and open it up and see the inside; and to be able to physically hold it, to feel it, is something that can’t be replicated in a computer.”
 Having worked in product development for the past few years, Garcia had seen what 3D printers were capable of and began investigating the possibilities for creating models for pediatric cardiologists to use before an operation. She began by asking surgeons from around the country what they thought of the idea. To say that their response was overwhelmingly positive is an understatement. The value of this idea was immediately apparent.
Having worked in product development for the past few years, Garcia had seen what 3D printers were capable of and began investigating the possibilities for creating models for pediatric cardiologists to use before an operation. She began by asking surgeons from around the country what they thought of the idea. To say that their response was overwhelmingly positive is an understatement. The value of this idea was immediately apparent.
Ariana has been doing well since her operation, but Anne Garcia wasn’t ready to let this idea go just because her daughter had already recovered from the surgery. She knew that there were many, many other parents out there going through exactly what she had experienced and children whose lives could not only be benefited but possibly even saved by getting such a tool integrated into the regular preparation done by pediatric surgeons.
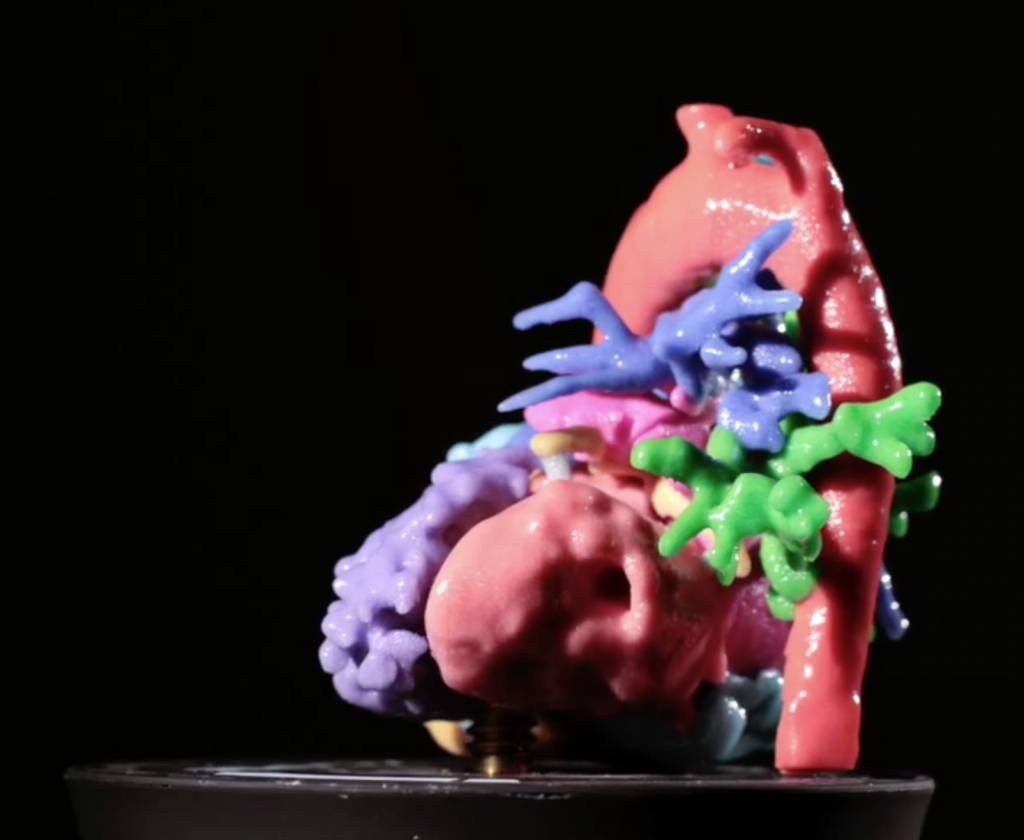 So, she began OpHeart as a way to advance this idea and to provide a platform for parents to better advocate for their children. The Houston-based nonprofit aims to put a 3D printed model of each patient’s heart into the hands of their surgeon before they undertake the operation. This takes time, of which there is never enough, and money, for which OpHeart engages in fundraisers, grant writing, and bids for donations.
So, she began OpHeart as a way to advance this idea and to provide a platform for parents to better advocate for their children. The Houston-based nonprofit aims to put a 3D printed model of each patient’s heart into the hands of their surgeon before they undertake the operation. This takes time, of which there is never enough, and money, for which OpHeart engages in fundraisers, grant writing, and bids for donations.
While there is no doubt that surgeons want to have access to this tool, it is complicated by the fact that insurance companies don’t have a code for this type of procedure.  Efforts are therefore underway to demonstrate to the enormous value of such preparation in terms of lowered risk to the patient both during and after the surgery, therefore also meaning long term cost savings for insurance companies. A small clinical trial is currently underway and a larger scale trial is planned for the fall.
Efforts are therefore underway to demonstrate to the enormous value of such preparation in terms of lowered risk to the patient both during and after the surgery, therefore also meaning long term cost savings for insurance companies. A small clinical trial is currently underway and a larger scale trial is planned for the fall.
In the meantime, Ariana continues to make progress towards recovery and OpHeart continues to pave the way for healthier future for pediatric patients.
Let us know your thoughts on the benefits of 3D printed surgical models in the OpHeart forum thread over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Gorilla Sports GE’s First 3D Printed Titanium Cast
How do you help a gorilla with a broken arm? Sounds like the start of a bad joke a zookeeper might tell, but it’s an actual dilemma recently faced by...
Nylon 3D Printed Parts Made More Functional with Coatings & Colors
Parts 3D printed from polyamide (PA, Nylon) 12 using powder bed fusion (PBF) are a mainstay in the additive manufacturing (AM) industry. While post-finishing processes have improved the porosity of...
$25M to Back Sintavia’s Largest Expansion of Metal 3D Printing Capacity Since 2019
Sintavia, the digital manufacturing company specializing in mission-critical parts for strategic sectors, announced a $25 million investment to increase its production capacity, the largest expansion to its operations since 2019....
Velo3D Initiates Public Offering in a Bid to Strengthen Financial Foundations and Drive Future Growth
Velo3D (NYSE: VLD) has been among a number of publicly traded 3D printing firms that have attempted to weather the current macroeconomic climate. After posting a challenging financial report for 2023,...
































