![]() What does the spleen actually do? Is this one of those organs that we even actually need? You can sometimes stump even the most degreed and intellectual people with this question. The answer is that the spleen is actually a valuable organ and functions in multiple important, valuable capacities–and yes, it can be removed, but it’s surely better to have one.
What does the spleen actually do? Is this one of those organs that we even actually need? You can sometimes stump even the most degreed and intellectual people with this question. The answer is that the spleen is actually a valuable organ and functions in multiple important, valuable capacities–and yes, it can be removed, but it’s surely better to have one.
The spleen actually plays a major and beneficial role in your body as a busy center not only for the recycling of red blood cells but also for storing white blood cells. It is known as a blood filter. This organ, located in the upper part of the abdomen under the rib cage, is also important in that it fights bacteria that cause life-threatening illnesses like meningitis.
With all of these considerations in mind, when it came to one patient’s spleen, Dr. Michael Itagaki from the Department of Interventional Radiology at the Swedish Medical Center in Seattle, Washington decided that, rather than removing the organ, he would attempt to save it by going the route of 3D printing.
The patient in question was experiencing multiple splenic artery aneurysms, which are prone to rupturing and can be potentially fatal. To remove the aneurysm, generally the entire spleen has to be removed along with it, but in this case Dr. Itagaki was against removal of the spleen due to the fact that it is beneficial and if one can be saved it’s so much better for the body. He suggested a splenic artery embolization to the patient, who informed him that she wanted neither that procedure nor to have her spleen removed. Quite simply, she wanted the doctor to find an alternative method and she wasn’t settling for anything less.
“Everybody said the spleen couldn’t be saved. It was ‘impossible.’ She either had to have her spleen removed or her splenic artery embolized,” stated Dr. Itagaki in his blog. “Do nothing and it was just a matter of time until an aneurysm ruptured, probably killing her.”
“I was greatly moved by my patient’s doggedness. She wasn’t willing to accept the limits of conventional medical treatment, so I didn’t think I should either. I kept searching for solutions.”
Dr. Itagaki read of a treatment that had been successful with brain aneurysms. He had hope that he could apply it to his patient’s condition, by a similar placement of metallic coils through a catheter, causing blood to clot, reducing pressure, and eliminating the chance of it rupturing.
“Could the specialized coils and catheters designed to treat aneurysms in the brain work in the splenic artery? Nobody seemed to know,” said Dr. Itagaki. “The patient’s splenic artery had an unusually large number of loops, which would complicate any procedure. A search of the published medical literature did not produce any useful results. There were many variables that were different.”
“I discussed my thoughts with the patient. I thought there might be a way to treat her aneurysms while sparing her spleen using this specialized brain aneurysm equipment. But the only way to know if the equipment would work would be to try it during an actual procedure. She gave me a puzzled look. ‘Well isn’t there a way for you to practice?’ she asked.”
Dr. Itagaki, inspired by this courageous and very stubborn patient, decided that perhaps he could practice with a 3D printed model. Having used 3D printing several times before for several simple prints, he had some basic knowledge of the technology, but no access to the technology and lacked anyone who had gone before him to act as a guide, aside from those who had performed the procedure on the brain, which is what it was developed for originally.
Hours of study, practice, and trials with software and hardware ensued before Dr. Itagaki decided to use a software mixture of Osirix and Blender for designing the detailed splenic artery model from the patient’s CT. Rather than purchasing expensive equipment, he merely sent his 3D design to a 3D printing service bureau.
“I paid for everything out-of-pocket,” said Dr. Itagaki. “When the models arrived in the mail I couldn’t believe it. They were precise full-scale replicas of the patient’s splenic artery.”
At that point, Dr. Itagaki was able to garner the enthusiasm of other medical professionals who had experience performing the procedure (sans practicing with 3D printing thus far) in brain aneurysms. For his practicing on the model, they not only donated all the equipment he would need, but even came to his home to help with the actual practicing.
Dr. Itagaki cut through all the necessary red tape to do the surgery, and used the 3D printed model repeatedly throughout the surgery. Due to his pre-surgical practice, he not only had the knowledge required to navigate through the procedure, but his time was nearly cut in half in performing the surgery.
“Even without having to try out different equipment combinations, the procedure was still very difficult and took five hours,” said Dr. Itagaki. “If I hadn’t had the ability to practice the procedure in the 3D printed model and preselect my equipment, it easily could have taken twice as long; that is, assuming I didn’t collapse from exhaustion and dehydration before finishing it. More importantly, the opportunity to practice the procedure beforehand gave me confidence that I could be safe and successful in doing something that had never been done before.”
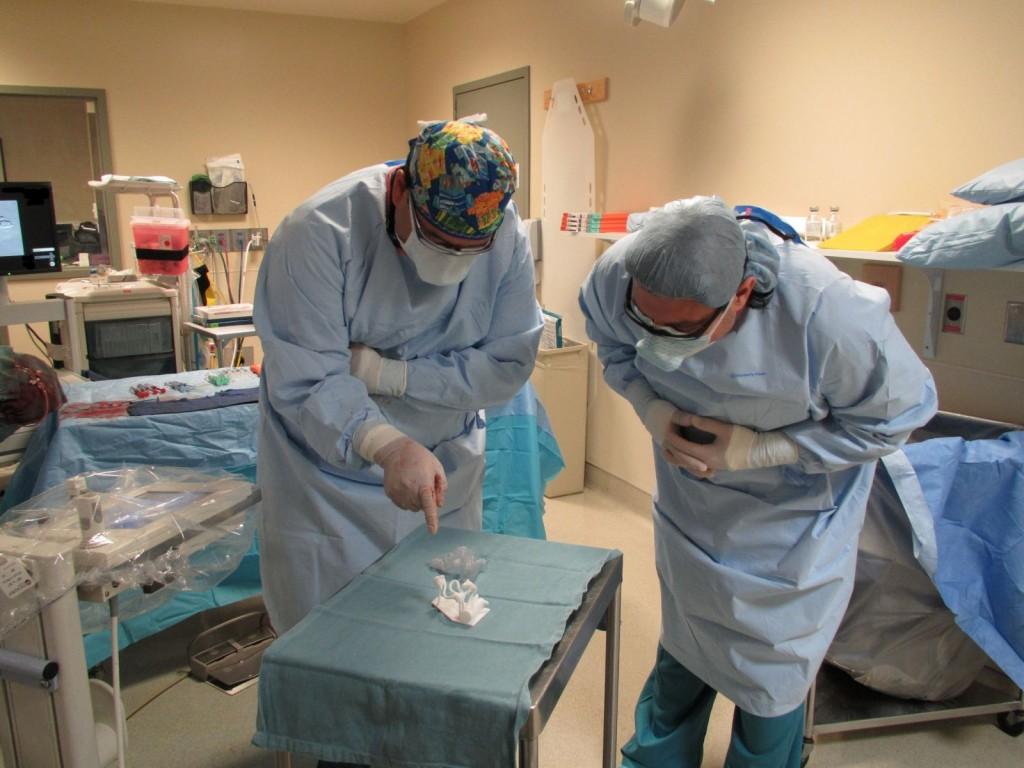
Referring to the 3D model in the operating room
Indeed, Dr. Itagaki was successful, and his patient lives on with her spleen as a wonderful piece of evidence demonstrating the benefits of persistence, surgical expertise and resourcefulness, and the innovation allowed by 3D printing.
“This experience fundamentally changed my perception about the value of 3D printing in medicine,” said Dr. Itagaki. “For safe, easy, and routine medical procedures, 3D printing will probably not have much of an impact in the foreseeable future. It’s too time consuming and costly to make 3D printed models. For complicated or high risk procedures, however, it can be invaluable.”
“No doctor wants to take unnecessary risks or have a bad outcome in surgery. Unfortunately, there are many, many unknowns in surgery, particularly with complex and unusual cases. 3D printing an anatomic model before surgery to study and practice reduces those unknown variables, making risky cases much safer. After my experience, I have no doubt that 3D printing will have a significant impact in improving patient care in all fields of medicine.”
After performing the successful procedure, Dr. Itagaki was inspired to begin a website, Embodi3D, for those who are interested in using 3D printing for biomedical science purposes. His site involves news, a forum for asking questions, and tutorials, as well as 3D medical model files for free download.
Dr. Itagaki also outlined the whole procedure in a paper, ‘Using 3D printed models for planning and guidance during endovascular intervention: a technical advance.’
It was certainly a full-circle team effort in not only saving this particular patient’s spleen but starting with research to trying something new and being able to apply it through the innovation of 3D printing. Dr. Itagaki’s persistence and resourcefulness gained the respect–and enthusiasm–of other medical professionals who wanted to see if the procedure would indeed be possible–and past that, successful.
Discuss your thoughts on this latest technological breakthrough in the 3D Medical Spleen Model forum thread over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
3D Printing News Briefs, April 13, 2024: Robotics, Orthotics, & Hypersonics
In 3D Printing News Briefs today, we’re focusing first on robotics, as Carnegie Mellon University’s new Robotics Innovation Center will house several community outreach programs, and Ugogo3D is now working...
Rail Giant Alstom Saves $15M with 3D Printing Automation Software 3D Spark
3D Spark has entered into a three-year deal with the rail giant Alstom. Alstom, a transport behemoth with annual revenues of $16 billion, specializes in the manufacture of trains, trams,...
Meltio Expands Global Reach with New Partnerships in the Americas and Europe
Spanish 3D printing manufacturer Meltio has expanded its sales network across the globe. With the addition of three new partners in the United States, Brazil, Argentina, and Italy, Meltio aims...
3D Printing Webinar and Event Roundup: April 7, 2024
Webinars and events in the 3D printing industry are picking back up this week! Sea-Air-Space is coming to Maryland, and SAE International is sponsoring a 3D Systems webinar about 3D...

































