Splashy headlines are made daily as innovators around the world highlight new 3D designs and 3D printed products eliciting ‘ooohs and aaahs’ as they are unveiled to an interested — and highly impressed — public.
Splashy headlines are made daily as innovators around the world highlight new 3D designs and 3D printed products eliciting ‘ooohs and aaahs’ as they are unveiled to an interested — and highly impressed — public.
High-powered business partnerships are being formed in high profile, with CEOs shaking hands as they come together to designate new international facilities to pump out 3D printed components for industries like aerospace, automotive, construction, and other highly specialized areas. It’s a race to build quality components with a better bottom line and better attention to deadline — and it couldn’t be done without 3D printing. It’s often also about dollars and cents.
There are however, some quieter light bulbs going off, resulting in using 3D printing in a variety of ways in the medical industry, and often helping with mapping out medical solutions and assisting in surgeries — or ruling them out. While surgeries certainly aren’t being ruled out with Kami Sutton, she’d like to avoid having more over time and to correct her current complications. The Marysville, Washington resident has had over 19 surgeries in her life.
Sutton, a grassroots coordinator with the American Heart Association, has a medical condition that most certainly caught great attention on the day she was born nearly three decades ago, when technology was far behind what we have now in nearly every fashion. Nineteen surgeries and one pacemaker later, Sutton, who was born with her heart on the right side of her body, has been investigating the wonders of 3D printing on her own as previous solutions have kept her alive and functioning, but certainly not at maximum capacity. While doctors often tire of patients perusing the internet and coming up with their own diagnoses and cures, this is one idea that raised an eyebrow and put a plan into action.
The congenital defect, with Sutton’s heart on the wrong side, also includes reversal of her heart’s left and right pumping chambers, a hole in between them, and a lack of connection to the lungs. Today, her heart and body are left taxed.
“My ventricles are beating out of sync,” she said. “We’re losing heart function, which is hard. … It’s not as efficient as it could be if they were beating together.”
Doctors believe the key to helping Sutton’s heart function better is with a new pacemaker, but despite so many surgeries, the area surrounding and the anatomy of her heart still remain uncharted territory — meaning they need to proceed with extreme caution. Dr. Stephan Seslar is in charge of working on the new pacemaker idea and hopes that he can bypass complications with Sutton’s condition to insert a new, bi-ventricular pacemaker. Inserting this pacemaker can be complex in patients with normal heart placement. With the bi-ventricular pacemaker, there is a third wire that runs through the back of the heart, assisting with the heart’s impulses, and improving timing.
If the new pacemaker were to work, it means the possibility for Sutton not having to wait and go through the exertion and complication of a heart transplant which is a delicate surgery and process with a more traditional heart. Sutton’s condition, obviously, presents additional concerns regarding a transplant in that it could be even more difficult to find a heart that would not be rejected.
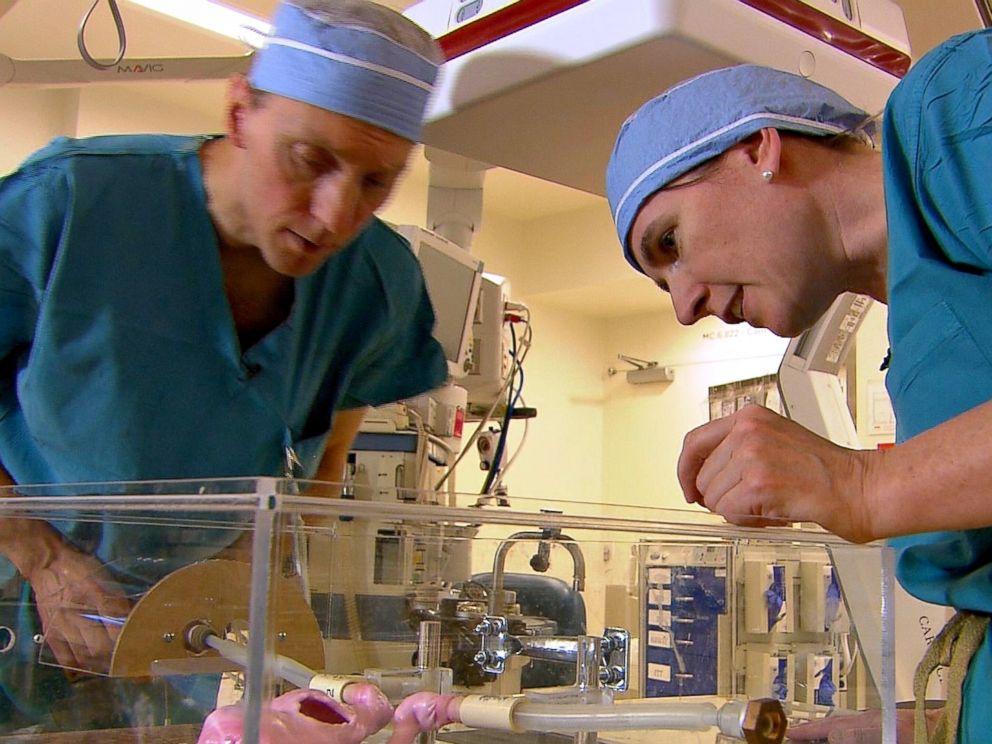 While Dr. Seslar, a congenital heart disease specialist and electrophysiologist at Seattle Children’s Hospital and University of Washington Medical Center, thinks the new pacemaker could be key to helping Sutton, they do have added complications to worry about when it comes to operating on their very unique patient.
While Dr. Seslar, a congenital heart disease specialist and electrophysiologist at Seattle Children’s Hospital and University of Washington Medical Center, thinks the new pacemaker could be key to helping Sutton, they do have added complications to worry about when it comes to operating on their very unique patient.
“Kami’s heart is truly one-of-a-kind,” Dr. Seslar said on the Seattle Children’s Hospital website. “Operating on her without understanding the anatomy of her heart better could be very dangerous.”
Sutton brought the idea of 3D printing a model of her heart to help with better understanding the anatomy and proceeding with insertion of the new pacemaker. “His eyes got really wide,” Sutton said of Dr. Seslar’s reaction when she asked if he could use a 3D model of her heart. “When I suggested it, he got really excited.”
Seslar set to work on the project, which involved a CT scan for Sutton and an appointment with a materials engineer who has the task of creating the finely detailed material that actually imitates cardiac tissue.
“Our first attempts produced stiff models that did not feel like human hearts,” Dr. Seslar said. “This model is soft and wet like a real heart inside a person. …We know ahead of time where to maneuver, it allows us to develop a game plan and potentially reduce the surgery time.”
Timing for the surgery is set for later this year with both surgeons and patient hopeful. While all involved know that it could still prove unsuccessful, with the use of 3D printed models to plan ahead and explore, they have a better chance than ever, and the whole process they are initiating now will continue to help patients improve their quality of life — and live — further down the road.
“Technology caught up with me just in time and gave me another chance besides the big [transplant] surgery,” Sutton said. “In the future it won’t take 19 operations over 26 years to fix the condition I was born with.”
We’ve reported on a number of stories regarding the use of 3D printed models for diagnosis and surgical assistance, but never in such a unique case as this. While 3D printing is useful in changing the way industries manufacture and designers create, it’s also helping medical solutions ascend to a much more advanced level — also offering quality, efficiency, and unheard of results for patients.
Have you been in a situation where a doctor or medical professional has used a 3D printed model to explain a procedure or diagnosis to you? How do you think 3D printed medical devices and models will advance medicine even further? Tell us your thoughts in the 3D Printed Model of Heart for Pacemaker Surgery forum thread over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
BLT Touts 100,000 Copper Parts Made
With the significant volume of copper used in electronics, semiconductors, aerospace, defense, and beyond, copper additive has had immense promise from the early days of copper 3D printing at Beamit...
3D Printing News Briefs, March 28, 2026: TCT Asia, Distribution Agreement, FDA Clearance
We’re starting 3D Printing News Briefs this weekend with some news out of TCT Asia, and then moving on to a metal AM distribution agreement between MULTISTATION and WAAM3D. We’ll...
3D Printing Moves Deeper Into Production as Parts Near $110B by 2034
A new report takes a closer look at how much 3D printing is actually being used in real production. The numbers point to a market that is already growing at...
AM Applications Expected to Reach $110B in 2034, New Report Finds
Additive manufacturing may still be a relatively young industry, but the number of real parts being produced with 3D printing is growing quickly. According to a new report from Additive...