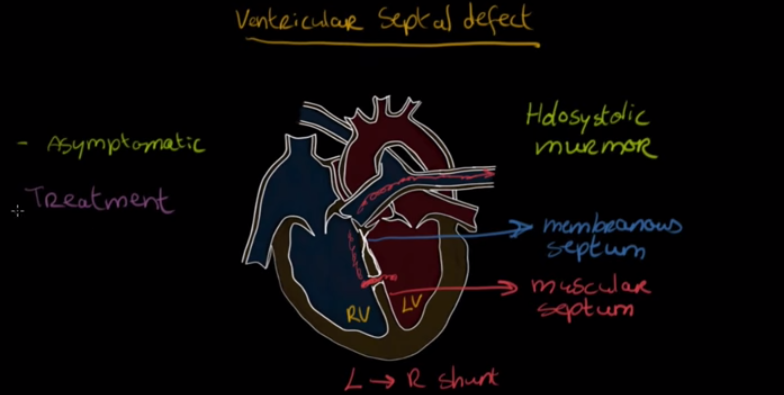
Postinfarction ventricular septal defect, or VSD, is an uncommon — but serious — complication of acute myocardial infarction and it’s often deadly.
Doctors say the event happens within 2-8 days after an infarction and often causes what’s known as cardiogenic shock. The condition requires that patients undergo emergency surgical treatment and coronary artery bypass grafting is often required.
 While improved surgical techniques to repair perforations in different areas of the septum have led to improved results, the current practice is complex and delicate.
While improved surgical techniques to repair perforations in different areas of the septum have led to improved results, the current practice is complex and delicate.
The preferred treatment is known as percutaneous closure , and surgeons say it’s perhaps the most viable treatment strategy. In surgery, the word ‘percutaneous’ refers to any medical procedure intervention done via needle-puncture of the skin rather than by using a scalpel or laser. This percutaneous approach is often used in vascular procedures like angioplasty and stenting, and it uses a needle catheter and a wire placed into a blood vessel.
 Now a group of doctors and technicians at the Bristol Heart Institute say they’re using 3D printed models to better understand the morphology of the defects and improve patient outcomes. They say building a physical, 3D printed representation of these defects will help remedy the relative lack of understanding involved in the defect and improve what they say is a limited range of available closure devices.
Now a group of doctors and technicians at the Bristol Heart Institute say they’re using 3D printed models to better understand the morphology of the defects and improve patient outcomes. They say building a physical, 3D printed representation of these defects will help remedy the relative lack of understanding involved in the defect and improve what they say is a limited range of available closure devices.
The Bristol Heart Institute, a leading center for the treatment of the condition using percutaneous intervention in their catheter lab, say using a physical representation of the defects will prove key in treating the damage.
Evan Ansell, Ian Negus, Margaret Saunders, Mark Turner, Nathan Manghat, and Mark Hamilton at the School of Cellular and Molecular Medicine of the University of Bristol and University Hospitals Bristol say a study they took proved that a 3D printer is ideal to reproduce representations of these ventricular septal defects.
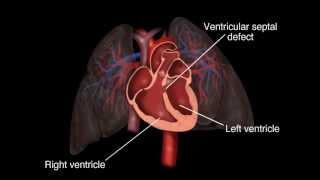 The team say their methodology will be used to review the treatment of VSDs and that 3D printing technology will be applied to visualizing a wide range of cardiac defects, both for later analysis of treatments and as models to aid them in planning surgical intervention.
The team say their methodology will be used to review the treatment of VSDs and that 3D printing technology will be applied to visualizing a wide range of cardiac defects, both for later analysis of treatments and as models to aid them in planning surgical intervention.
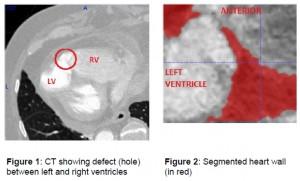
Researchers used a RepRap Mendel printer to build models segmented from CT scans to develop a method to take image data from what’s called CT Coronary Angiography. The data is used to create a 3D print of a VSD, and doctors can then use the models to assess the accuracy of the process and identify any limitations which might exist.
The team says the data was anonymized before software was used to select the area affected by the defect and then create a ‘segmented’ portion of the ventricular wall for review.
Doctors and researchers are now bring the full power of 3D printing technology to bear in their efforts to plan for delicate surgical procedures. Do you know of any ways medical professionals are using 3D printing to improve patient outcomes? Let us know in the 3D Printed Models to Save Lives forum thread on 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Gorilla Sports GE’s First 3D Printed Titanium Cast
How do you help a gorilla with a broken arm? Sounds like the start of a bad joke a zookeeper might tell, but it’s an actual dilemma recently faced by...
Nylon 3D Printed Parts Made More Functional with Coatings & Colors
Parts 3D printed from polyamide (PA, Nylon) 12 using powder bed fusion (PBF) are a mainstay in the additive manufacturing (AM) industry. While post-finishing processes have improved the porosity of...
$25M to Back Sintavia’s Largest Expansion of Metal 3D Printing Capacity Since 2019
Sintavia, the digital manufacturing company specializing in mission-critical parts for strategic sectors, announced a $25 million investment to increase its production capacity, the largest expansion to its operations since 2019....
Velo3D Initiates Public Offering in a Bid to Strengthen Financial Foundations and Drive Future Growth
Velo3D (NYSE: VLD) has been among a number of publicly traded 3D printing firms that have attempted to weather the current macroeconomic climate. After posting a challenging financial report for 2023,...