Testicle Tissues Bioprinted for the First Time to Combat Infertility
A team of scientists working at The University of British Columbia (UBC) ’s Vancouver Prostate Centre have pioneered a new method for bioprinting human testicular cells. The discovery could one day offer a solution for people living with currently untreatable forms of male infertility and has potential for future disease modeling and regenerative opportunities in personalized medicine. Researchers at UBC demonstrated for the first time the feasibility of 3D bioprinting adult human testicular cells and identified promising early signs of sperm-producing capabilities.
Vancouver Coastal Health Research Institute researcher and UBC urology assistant professor Ryan Flannigan is the lead author of a study that explains how the team 3D bioprinted patient-derived testis cells in the February 16 issue of ASRM’s Fertility and Sterility international journal.
“We’re 3D printing these cells into a very specific structure that mimics human anatomy, which we think is our best shot at stimulating sperm production. If successful, this could open the door to new fertility treatments for couples who currently have no other options,” said Flannigan, whose lab is based at the Vancouver Prostate Centre at Vancouver General Hospital.
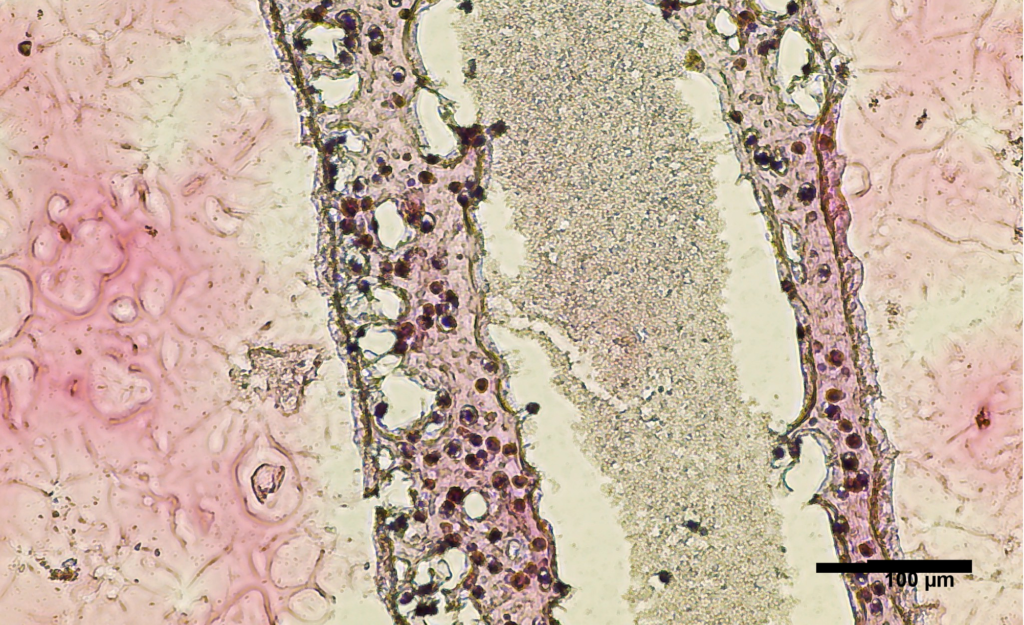
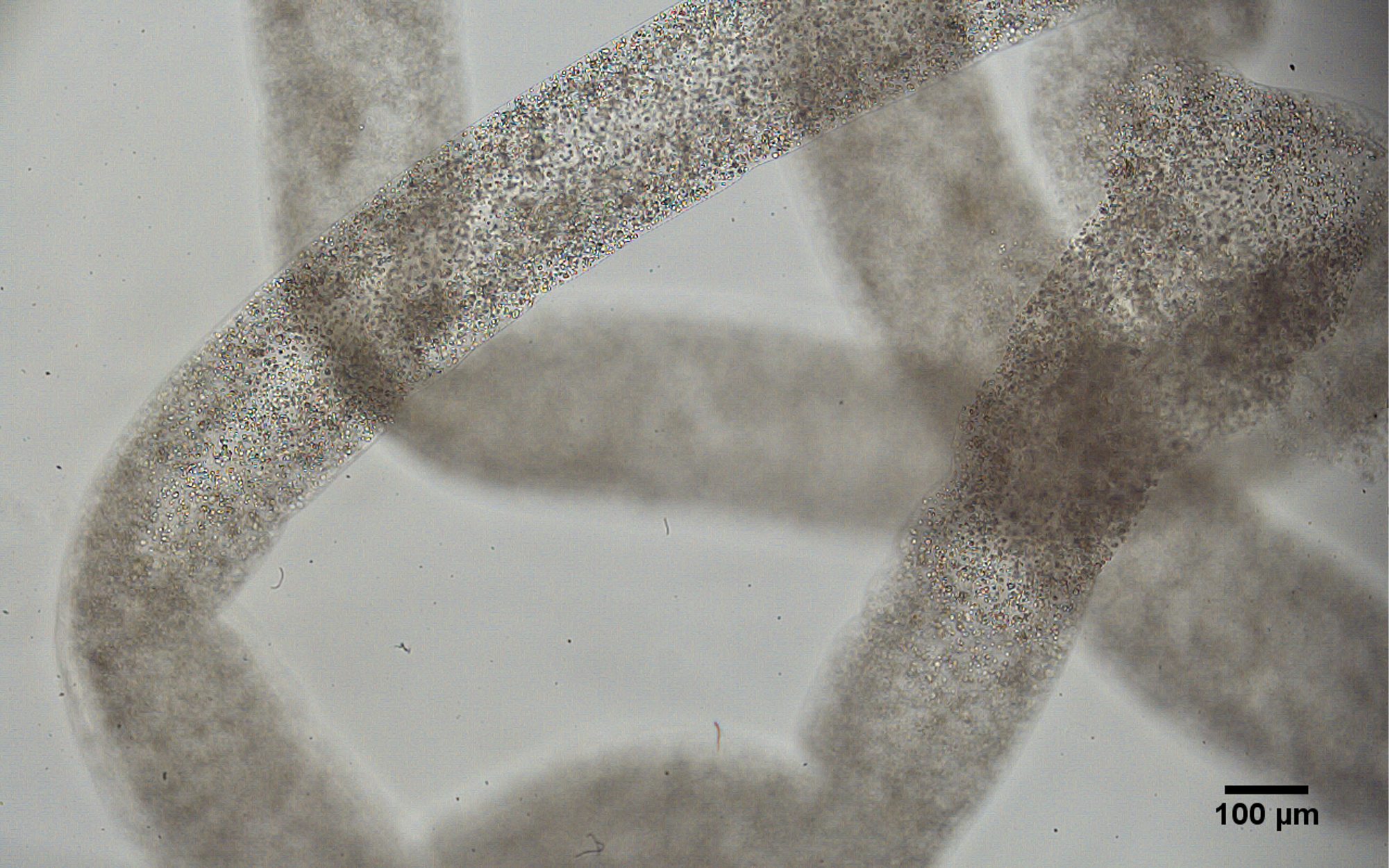
Cross-section of human testicular cells 3D printed into a tubular structure. Image courtesy of the University of British Columbia.
For the study, the researchers performed a biopsy to collect stem cells from the testicles of a 31-year-old patient living with the most severe form of male infertility, known as non‐obstructive azoospermia (NOA). The cells were then grown, and 3D printed onto a petri dish into a hollow tubular structure that resembles the sperm-producing seminiferous tubules.
Twelve days after printing, the team claims they found that the cells had survived. Not only that, they had matured into several of the specialized cells involved in sperm production and were showing a significant improvement in spermatogonial stem cell maintenance––both early signs of sperm-producing capabilities.
With a little help from a bioprinter
For the task, they relied on Aspect Biosystems‘ RX1 bioprinter, one of the brand’s latest additions to its portfolio. Released in 2017, the RX1 bioprinter is a proprietary technology that relies on microfluidic printheads to mix materials rather than using a regular syringe with bioinks. According to the company, the technique allows microscale resolution at high speed while the on-printhead crosslinking procedure permits printing a wide range of materials with high fidelity, including low viscosity bioinks, to mimic soft tissue microenvironments.
Developed to advance research and clinical applications in the bioprinting field, it seems the RX1 is doing just that. Since its launch, the brand’s flagship product has been used by a wide range of companies and universities. Moreover, Aspect Biosystems has partnered with many industry leaders to develop ground-breaking applications, including a team at Japanese firm JSR Corporation to develop an implantable vascularized tissue for kidney regeneration. Similarly, Merck and GSK are using the RX1 Bioprinter to develop a highly physiological, high-throughput tissue model that will enable the elucidation of mechanisms of the tumor microenvironment and ultimately lead to the development of an immuno-oncology model for the accurate and predictive screening of immuno-therapeutics targeting cancers, such as triple-negative breast cancer.
As for the latest study, the focus on infertility is crucial. The disease has become a global public health issue affecting a significant proportion of humanity, which has not displayed any decrease over the last 20 years. However, this new study will boost infertility research.
Infertility affects 15% of couples, and male factors are a contributing cause in at least half those cases, says Flannigan. Moreover, the researcher explained that in the most severe form of male infertility, or NOA, no sperm is found in the ejaculate due to diminished sperm production. While doctors can help NOA patients by performing surgery to find extremely rare sperm in some cases, Flannigan says this procedure is only successful about half the time.
“Unfortunately, for the other half of these individuals, they don’t have any options because we can’t find sperm for them,” pointed out the expert, who highlighted that he hopes to help each one of those patients.
Even though the team knows there is still a long road ahead, this huge milestone makes them hopeful. Led by Flannigan, the scientists are now working to “coach” the printed cells into producing sperm. To do this, they’ll expose the cells to different nutrients and growth factors and fine-tune the structural arrangement to facilitate cell-to-cell interaction.
If they can get the cells to produce sperm, then it could potentially be used to fertilize an egg via in vitro fertilization, providing a new fertility treatment option for couples.
Flannigan’s research program has also shed new light on the genetic and molecular mechanisms that contribute to NOA. They’ve been using various single-cell sequencing techniques to understand each cell’s gene expression and characteristics, then applying computational modeling of this data to better understand the root causes of the condition and identify new treatment options.
“Increasingly, we’re learning that there are likely many different causes of infertility and that each case is very patient-specific,” concluded Flannigan. “With that in mind, we’re taking a personalized, precision medicine approach. We take cells from a patient, try to understand what abnormalities are unique to them, and then 3D print and support the cells in ways that overcome those original deficiencies.”
If the UBC scientists are successful, they could enable treatments for male patients with infertility and have a substantial global impact. Not just for the disease itself, but it could also lead to a better understanding of manufacturing human tissues and, eventually organs. As experts learn how to apply bioprinting technology to specific tissue types, the niche biotechnology segment will start closing the gaps between research and treatment, bridging the way towards the holy grail of creating organs on demand.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
China Becomes Latest Space Power to Demonstrate Metal 3D Printing in Orbit
China has demonstrated metal 3D printing in space as part of its plan to develop manufacturing technologies for future space missions, including Moon construction. The experiment took place aboard the Qingzhou...
AMPulse Asia: APAC 3D Printing Market Roundup
Key Takeaways Coverage window: April 27 to May 10, 2026. Roughly 30 additive manufacturing (AM)-relevant announcements were tracked across eight Asia-Pacific countries. Largest disclosures: Farsoon Technologies (688433.SH) filing a RMB...
3D Printing Financials: Stratasys Bets on Defense and Drones as Printer Sales Slow
Stratasys (Nasdaq: SSYS) started 2026 with lower revenue and a larger loss as customers continued to slow down spending on new 3D printers. Still, the company pointed to stable recurring...
3D Printing Financials: Xometry Surges After Record Quarter and Siemens Deal
Shares of Xometry (Nasdaq: XMTR) surged on Thursday, May 7, after the company reported record first-quarter 2026 results and announced a major partnership with Siemens. The stock climbed as much...