Researchers 3D Print Lifelike Aortic Valve Model with Built-in Sensors
In order to help surgeons prepare to perform procedures on patients (say that three times fast), training with 3D printed medical models has been shown to help improve the overall outcome of the surgery. A team of researchers from the University of Minnesota (UMN) published a paper in the peer-reviewed Science Advances journal about their work using multimaterial 3D printing to create extremely lifelike, patient-specific models of the aortic valve of the heart.
The abstract states, “Minimally invasive surgeries have numerous advantages, yet complications may arise from limited knowledge about the anatomical site targeted for the delivery of therapy. Transcatheter aortic valve replacement (TAVR) is a minimally invasive procedure for treating aortic stenosis. Here, we demonstrate multimaterial three-dimensional printing of patient-specific soft aortic root models with internally integrated electronic sensor arrays that can augment testing for TAVR preprocedural planning.”
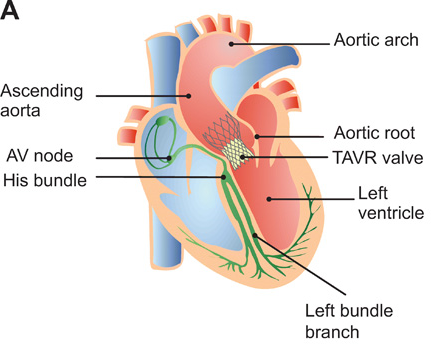
Schematic of the heart with implanted TAVR prosthesis in the aortic root region. AV, atrioventricular.
The team made the organ models, which also include the structures surrounding the aortic valve, with a customized 3D printing process and specialized inks. Combined with integrated soft sensor arrays, the 3D printed models replicate the look and feel of an actual human aorta.
“Our goal with these 3D-printed models is to reduce medical risks and complications by providing patient-specific tools to help doctors understand the exact anatomical structure and mechanical properties of the specific patient’s heart. Physicians can test and try the valve implants before the actual procedure. The models can also help patients better understand their own anatomy and the procedure itself,” said Michael McAlpine, one of the study’s senior researchers and a UMN mechanical engineering professor who knows a little something about 3D printing sensors and organ models.
Medtronic funded the research, with help from the National Institute of Biomedical Imaging and Bioengineering of the National Institutes of Health, the Minnesota Discovery, Research, and InnoVation Economy (MnDRIVE) Initiative, and a University of Minnesota Interdisciplinary Doctoral Fellowship and Doctoral Dissertation Fellowship awarded to Ghazaleh Haghiashtiani, co-first author and a recent UMN mechanical engineering PhD graduate who now works at Seagate. The rest of the team consisted of:
- Kaiyan Qiu, co-first author and a former mechanical engineering postdoctoral researcher who is now an assistant professor at Washington State University;
- Jorge D. Zhingre Sanchez, a former biomedical engineering PhD student who worked in the UMN’s Visible Heart Laboratories and is now a senior R&D engineer at Medtronic;
- Zachary J. Fuenning, a mechanical engineering graduate student;
- Paul A. Iaizzo, a professor of surgery in the university’s Medical School and the founding director of the Visible Heart Laboratories;
- Priya Nair, senior scientist at Medtronic;
- Sarah E. Ahlberg, director of research & technology at Medtronic

Patient-specific organ models, which include integrated 3D printed soft sensor arrays, were fabricated using specialized inks and a customized 3D printing process. Such models can be used in preparation for minimally invasive procedures to improve outcomes in thousands of patients worldwide. (Image courtesy of McAlpine Group, University of Minnesota)
This organ model was created for a very specific procedure: a Transcatheter Aortic Valve Replacement (TAVR). Used to treat aortic stenosis, which is when the aortic valve narrows and reduces or blocks blood flow from the heart into the main artery, TAVR consists of placing a new aortic valve inside a patient’s existing one. This cardiovascular condition is one of the most common among the elderly, affecting roughly 2.7 million adults over 75 years of age in North America, and TAVR is a far less invasive choice for fixing the valve than turning to open heart surgery.
The researchers used CT scans to 3D print the part of the aorta that’s attached to the heart, called the aortic root. This is made up of the openings for the coronary arteries and the aortic valve, the latter of which features three flaps, or leaflets, that are surrounded by a fibrous ring. The ascending aorta and left ventricle muscle were also included in the model. By using an ink that’s reminiscent of the spackling paste used to fix plaster and drywall, the specialized 3D printers at the university were able to make a model that replicates the organ’s soft tissue components and the hard calcification found on the valve flaps. Additionally, special silicone-based inks allowed the 3D printed model to match how soft real heart tissue feels.
Integrated sensors, which were 3D printed within the aortic valve model, can provide surgeons with electronic pressure feedback, which helps them guide and optimize the best anatomical position of the actual valve device in the patient.
“We evaluated the efficacies of the models by comparing their geometric fidelities with postoperative data from patients, as well as their in vitro hemodynamic performances in cases with and without leaflet calcifications. Furthermore, we demonstrated that internal sensor arrays can facilitate the optimization of bioprosthetic valve selections and in vitro placements via mapping of the pressures applied on the critical regions of the aortic anatomies,” the researchers wrote in their paper.

Anatomical fidelity analyses of the 3D printed aortic root models and comparison to patient postoperative data. (A) CT scan of the 3D printed aortic root model. (B) Calibrated distance map comparing the anatomical fidelity of the 3D printed aortic root model with the patient’s anatomy. (C) Histogram of the calibrated distances between the surface points of the 3D printed aortic root model and the patient’s anatomy. (D) Comparison of the implanted TAVR prosthesis in the 3D printed model with the patient’s postoperative data. RCA, right coronary artery; LCA, left coronary artery. (E) Comparison of changes in frame diameters of the implanted valve in the 3D printed model with the patient’s postoperative data at nine different node levels.
While this aortic valve model is pretty great, McAlpine is sure that these 3D printed organ models can only continue to get better.
“As our 3D-printing techniques continue to improve and we discover new ways to integrate electronics to mimic organ function, the models themselves may be used as artificial replacement organs. Someday maybe these ‘bionic’ organs can be as good as or better than their biological counterparts,” he said.
(Source: University of Minnesota)
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
nScrypt’s Ken Church on Why Additive Electronics Is Finally Finding Its Fit
For years, additive manufacturing (AM) has promised to reshape electronics. The idea has always been to print circuits directly where they are needed, add them into parts, and move beyond...
Harvard’s Jennifer Lewis Lab Is 3D Printing Artificial Muscles That Twist and Bend on Demand
Researchers at Harvard John A. Paulson School of Engineering and Applied Sciences (SEAS) have developed a new way to 3D print materials that can move on their own, bending, twisting,...
3D Printing News Briefs, May 2, 2026: Soft Robots, Agricultural Waste, & More
In this weekend’s 3D Printing News Briefs, we’ll start off with a multi-laser metal powder bed fusion 3D printer and post-processing news. We’ll end with research into soft robotics and...
Harvard SEAS Engineers Develop 3D Printing Method for Soft Robotic Components with Programmable Shapes
The world of soft robotics is still largely in its pure research phase, but the R&D landscape has started to produce examples of early-stage commercialization. Researchers have started to refine...















































