China: 3D Printed Vertebral Body Used to Reconstruct Upper Cervical Spine of 9 Patients
Primary osseous spinal tumors make up roughly 5% of all primary bone tumors, and reconstruction is required to restore the spine’s integrity and stability. However, it’s hard to reconstruct this complex section, which is responsible for transitioning the axial loading force from the cranium to the spinal column, and subpar implants can result in complications like migration and nonfusion.
3D printing can be used to fabricate patient-specific porous implants for fixing these bone defects. A group of researchers from Beijing published a study, “Upper cervical spine reconstruction using customized 3D-printed vertebral body in 9 patients with primary tumors involving C2,” where they described “the clinical outcomes of upper cervical spine reconstruction using customized 3D-printed vertebral body,” with “a mean follow-up of 28.6 months” for the patients.
“Patients with primary tumors involving C2 who were treated in our institution between July 2014 and November 2018 were enrolled,” the team stated.
“Nine patients (2 males and 7 females) were included in the study with a mean age of 31.4 years (12 to 59 years). Seven patients demonstrated tumors located in C2 and 2 showed involvement of C2 and C3.”
The nine patients initially complained of “aggravating pain,” with two suffering neurological impairment, and average duration since the onset of these symptoms was almost three months. Here’s the tumor breakdown for the patients, established using a CT-guided biopsy:
- 4 giant cell tumors (GCT)
- 2 chordoma
- 1 Ewing sarcoma
- 1 paraganglioma
- 1 aggressive hemangioendothelioma
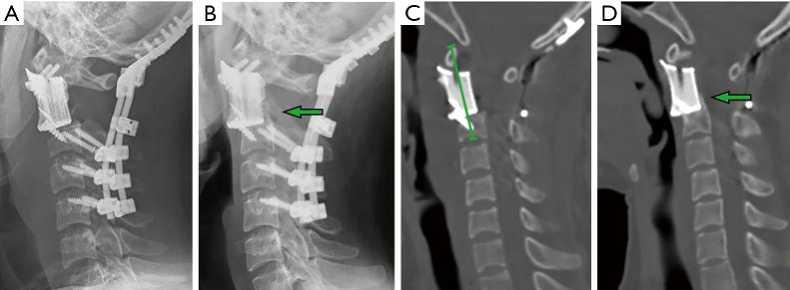
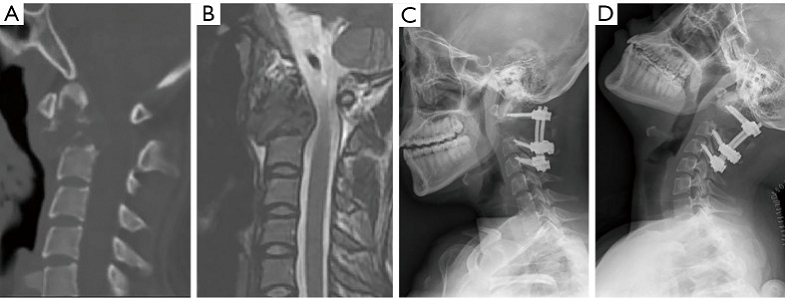
Fig. 1: Imaging studies for patient #3. The achievement of osseointegration was defined when new bone formation was observed around the bone-implant interface on X-ray (B) and CT (D) during the follow-up compared to that of immediately postoperative (A,C). The postoperative segment vertebral height was measured on the midsagittal reconstruction CT from atlas anterior tubercle to the midpoint of the adjacent lower endplate (C).
Making the implants was a 7-day process. First, CT scans were performed on the patients’ spines, and the DICOM data was imported into Materialise Mimics 15.0 software, where a CAD model for the implant was designed. Ti6Al4V powder was used to print the porous metal scaffold implants with Arcam EBM’s electron beam melting technology.
“Based on our previous studies, the parameters set for the trabecular structure and the size of the uniform micro-pores were determined to generate the optimized biomechanical and osteoinductive properties (8,15,16). The upper contact surface morphology of the implant coincided with the inferior articular surfaces of C1, while the lower contact surface morphology coincided with the upper endplate of the caudal vertebra,” they wrote.

Fig. 2: The 3D printed artificial vertebral body with porous scaffold fabricated out of titanium alloy powder.
A two-stage intralesional spondylectomy was performed on each patient, and the 3D printed vertebral body was used to accomplish anterior reconstruction, without the use of a bone graft.
“The average interval between the posterior and anterior procedures was 14.4 days,” the researchers said.
“In the first 4 cases in this series, occipitocervical fixation was performed (Figure 1). Subsequently, with more confidence in the stability of the 3D-printed anterior construct, we were able to preserve the atlanto-occipital joint in the next 5 cases.”
If you’re interested in the rest of the nitty-gritty surgical details, check out the full research paper.
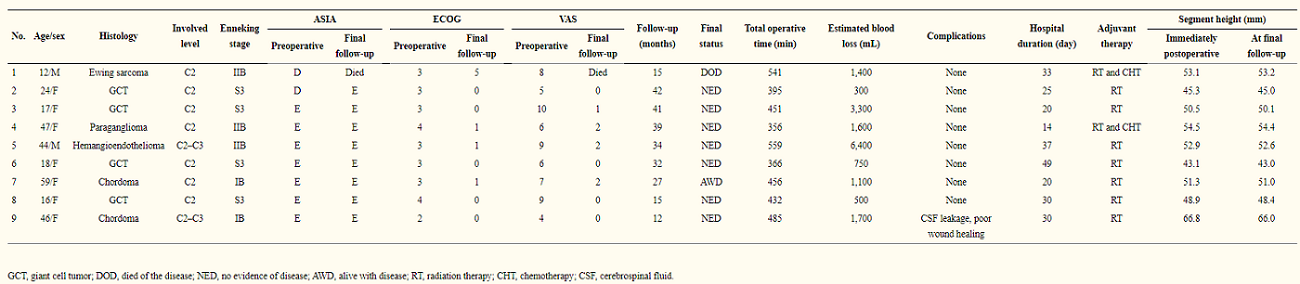
In the table above, you can see the details of the patients, who all had follow-up appointments after the 3D printed vertebral body was implanted. All nine received postoperative radiotherapy, while two also received chemotherapy.
“Patient one died of systemic metastases 15 months postoperatively without signs of local recurrence. Patient seven had tumor local recurrence. The others were alive and functional in their daily livings at the last follow-up without evidence of disease. At their final follow-ups, the neurological status of all alive patients was ASIA E, and the average VAS score was 0.9. Three patients had ECOG 1, while 5 patients had ECOG 0 for their general well-being and activities of daily life,” they stated.
Through radiograph and CT examinations, the researchers observed new bone formation around the bone to implant contact surfaces, “which provided the evidence of osseointegration,” and they found that all of the 3D printed vertebral bodies were stable, without any signs of ” implant displacement or subsidence.” Additionally, none of the screws had come loose, and there was no rod breakage in the posterior instrumentation systems.
The researchers found several advantages to using 3D printing for this reconstruction rather than traditional methods of manufacturing, such as the implant offering “reliable primary immediate postoperative stability.” A patient-specific implant provides a better match to bony surfaces and a larger contact area, and because screw tracks are actually integrated directly into the artificial vertebra, “self-stabilization” occurs.
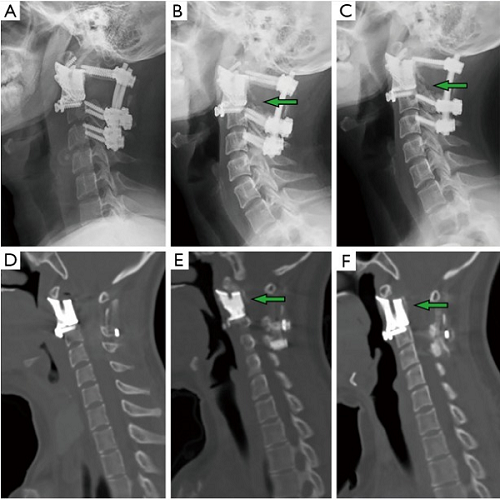
Fig. 4: Imaging studies for patient #6 showing fusion process. Compared to the immediate postoperative X-ray (A) and CT (D), regenerated osseous tissue can be seen to have gradually grown along the implant 12 months (B,E) and 24 months (C,F) post-op (arrow).
“Secondly, the anatomical design of the contact surface of the curved porous endplate and its biocompatibility provided reliable mid-long-term stability. The porous bone-contacting surface of the 3D-printed vertebral body is conducive to bone in-growth into the trabecular pores to achieve firm osseointegration, which was supported by evidence from previous basic research and in vivo studies (15,16,24),” they explained.
Additionally, post-op radiotherapy may not affect the 3D printed vertebral body as much, so long as osseointegration on two ends occur, “because solid combination was accomplished.” Conversely, this treatment can lead to instrumentation failure with conventionally manufactured implants.
“In our study, the progress of osseointegration is evident on follow-up with imaging studies. On lateral radiography, regenerated osseous tissue was seen adhering to the 3D-printed vertebral body (Figures 1B,4B,C1B,4B,C).),” the researchers noted. “Sagittal CT revealed new bone tissue crawling and growing around the ends of the 3D-printed vertebral body from the upper and lower vertebra (Figures 1D,4E,F1D,4E,F).). All patients were capable of resuming normal activity without mechanical pain associated with spinal instability at 12-month follow-up.”
Finally, a 3D printed vertebral body could mean there’s less of a need for transoral (direct access through the mouth) or transmandibular surgical approaches. For example, as noted above, this research team used the posterior-anterior approach to perform C2 spondylectomy, which made it easier and safer to isolate the vertebral arteries.
“Our study suggests that 3D-printed implant may be a good option in upper cervical reconstruction, the tailored shape matching with the contact surfaces and the porous structure conductive to osseointegration provide both short- and long-term stability to the implant,” the researchers concluded. “However, a higher level of evidence is still needed.”
Discuss this and other 3D printing topics at 3DPrintBoard.com or share your thoughts below.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Creality Marks 12 Years with KliTek and AI-Powered Ecosystem Expansion
For 12 years, Creality has advanced accessible 3D printing technologies, enabling global users to turn ideas into tangible creations. What began as a desktop 3D printer manufacturer has evolved into...
Asia AM Watch: Creality Launches $177M Hong Kong IPO as HKEX Trading Debut Nears
Creality has formally launched its Hong Kong initial public offering (IPO), marking one of the biggest public market moves by a 3D printing company in 2026 and offering a new...
How AtomForm’s 12-Nozzle System Cuts Multi-Color FDM Transition Waste by Up to 90%
Pull up the print stats on multi-color FDM jobs. The number that stings isn’t time; it’s material efficiency. On six-color models, single-nozzle systems consume significant filament during transition flushing, expelling...
3D Printed Weapons Keep Showing Up in Crime
In the past few weeks, activity around 3D printed weapons in the U.S. has increased across several fronts. States including California, Colorado, New York, and Washington are moving forward with...