A trio of researchers from Bucharest, Romania completed a multi-centre cohort study, entitled “3D patient specific implants for cranioplasty,” about 50 patients from 10 hospitals with a variety of cranial defects.
A cranioplasty is performed to repair these defects after congenital anomalies, growing skull fractures, surgical decompression, trauma, or tumor surgery, which can result in aesthetic, functional, and psychological implications. We’ve seen 3D printing used in this type of procedure before.
The abstract states, “In all patients the neurosurgeon repaired the cranial defect using 3D printed and CNC milling and drilling grafts or Patient Specific Implants, from two world known manufacturers, custom made in accordance with the data obtained from the patient’s 3D CT reconstruction.”
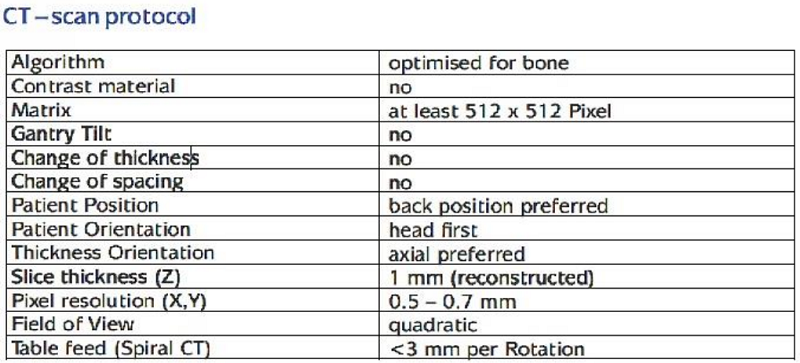
Of the 50 patients between 5-68 years old, 16 were female and 34 were male, while 22 were from urban areas and 28 from rural. 31 patients presented with trauma, while 16 were decompression and three had a tumor. The neurosurgeons used a scanning protocol, coupled with data from patients’ 3D CT reconstruction, to determine whether 3D printing or CAD-CAM manufacturing should be used to fabricate the patient-specific implants.
The procedure was the same for nearly all the cases – DICOM data files were collected, archived into a ZIP file, and sent in an encrypted message through a secure platform to keep the information confidential. Once the files are extracted, they’re verified to make sure the scan protocol was followed, and to see if they can be transformed to STL files in order to clearly see the bone defect and compare it “with standard anatomic models, with contra-lateral side of the same patient” in order to develop a 3D dynamic model of the cranium with the defects included.
“The 3D model (pdf file with 3D media option activated) is sent and presented by manufacturer directly to the surgeon with several comments regarding: surrounding soft tissue, sizes, distances, thickness and a lot of other parameters, including material together with an approval letter that has to be stamped and signed by the surgeon,” the researchers explained. “The surgeon will reply (in written) to the manufacturer with its comments regarding all of the above and in some steps will conclude if he agrees or not, on the proposed 3D model. If the response is affirmative and all legal and financial issues are agreed upon by all parts, the manufacturer will start to produce the implant, respecting all safety and regulations of EU, regarding Patient Specific Implants. That will be delivered in the country of the surgeon, directly to its hospital OR during a period of 5-15 days. In some emergency cases, the implant can be delivered within 48 hours, with a set of legal documents and a passport for the implant; the passport contains all of the important info that patient has to have, after surgery. If the Implant came unsterile and very well packaged, it will be sterilized to 134 °, 1-2 cicles 20 minutes, 24-48 hours prior the day of surgery.”
Surgeons used factors like anatomical area, risk of infection, and position and size of the defect to determine which material to use – 45 implants were made with PEEK, while four were created out of a titanium alloy and one was made from the ceramic glass material Bioverit. These same factors were taken into consideration when determining the best type of fixation system, such as bio-resorbable craniofix implants that use a special tool for anchoring and fixation, titanium holed plates, non-locking or locking screws, or non-resorbable sutures.
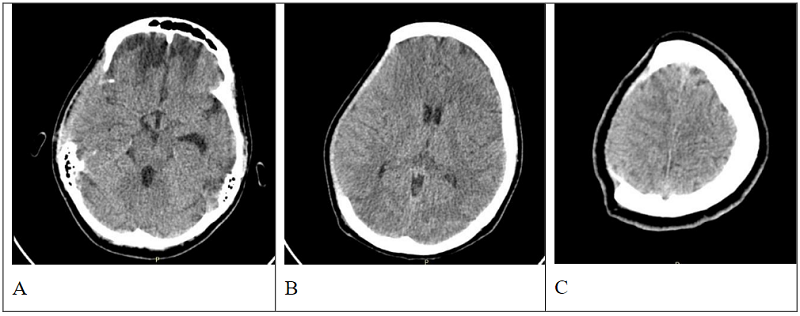
The presented case was for a 23-year-old female whose cranial trauma was caused by a car accident. Upon arrival, she had a Glasgow (coma state) score of 3 and intracranial pressure with a peak of 80 mmHg – the standard value is 20 mmHg. The surgeon observed a cerebral edema post-trauma malign, and chose to fix it using a cranial resection with dural plasty. Three days later, the surgeon performed “a large craniectomy FTPO (fontal-temporal-parietal-occipital) and dural plasty with temporal muscle and periosteum.” The cranioplasty was performed 44 days later.
The manufacturer received and analyzed the patient’s CT DICOM files, and created a 3D model that the surgeon then had to approve.
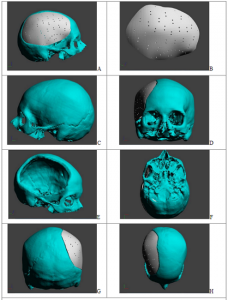
FIGURE 4. Presentation of 3D model proposed by manufacturer using Adobe Acrobat 3D pdf file where model can be visualized in motion. (A) right view with implant; (B) proposed model of implant; (C) left view; (D) frontal view with implant into defect; (E) right view without implant; (F) below view; (G) rear view with implant; (H) above view with implant in place.
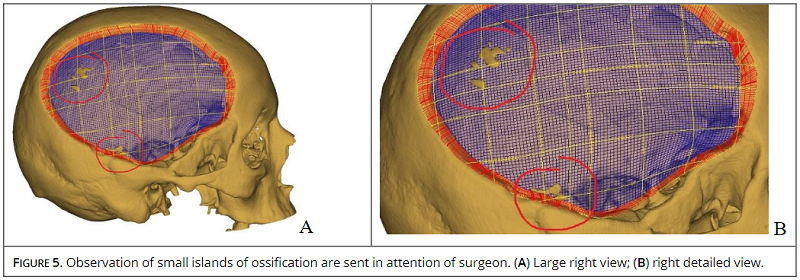
“There are cases when CT DICOM files are rejected, because they are not done as required by the protocol and they are not accurate enough and cannot be used for 3D model and also for implant construction,” the researchers explained.
“A team of specialists in cranial reconstruction communicate to the surgeon (in writing): any possible complications, details regarding sizes of implants, remaining bone, distances and surrounding soft tissues, options for manufacturing materials, fixation systems (Titanium Alloy, Peek, Bioverit–ceramic glass) (9,10) to help him take the most efficient decision.”
The surgeon asked for the implant to be fabricated from PEEK-Optima, in case any intra-op adjustments were needed, and also requested 1 cm suture holes.
In this particular case, the patient-specific implant was not 3D printed; rather, CAD-CAM manufacturing was used.
“Regarding the general study: There were a total of 50 patients treated with Patient Specific Implant that proved significant aesthetic, functional and psychological improvements after the cranioplasty surgery,” the researchers explained. “Minor complications occurred in several cases, that were related to cranioplasty fixation systems and scalp complications (related to initial trauma), and two cases of wound infection (one related to the type of suture used and the otherwound contamination without suture defect). There were no fatalities and no long-term complications.”
The team concluded that a custom 3D printed patient-specific implant can result in better aesthetics and “good functional outcomes,” making this cranial reconstruction option “a safe and viable solution.”
“Nevertheless, the financial aspect of using such an implant is the main factor that negatively influences the addressability of such a technique to the general public,” the researchers wrote. “At this time Patient Specific Implants in Romania are paid by patients and are expensive, but very reliable and effective at the same time.”
Discuss this story and other 3D printing topics at 3DPrintBoard.com or share your thoughts in the Facebook comments below.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Ceramitec 2026 3D Printing Wrap Up
I was surprised by just how many 3D printing companies and 3D printing projects there were at Ceramitec this year. I came away from the show convinced that the ceramics...
RusselSmith Brings Additive to Ghana’s Maritime Sector
Nigerian firm RusselSmith is in talks with Ghana’s Maritime Authority (GMA) to bring 3D printing to Ghana’s maritime sector. The Commonwealth Enterprise and Investment Council (CWEIC) helped make the discussion...
The Blueprint for Industrial Serial Production
Lithoz is kicking off the 2026 trade fair season with a powerful showcase of real-world applications of ceramic AM serial production capabilities alongside new material upgrades. The company is stepping...
Fraunhofer ILT Tests 3D Printed Titanium Reactors to Generate Hydrogen Onboard Heavy Vehicles
The Aachen-based Fraunhofer Institute for Laser Technology (Fraunhofer ILT) is to research titanium aluminide hydrogen reactors and heat exchangers. The hope is that lightweight, better-performing 3D printed components will make...