3D Printed Paracetamol Tablets Have Big Implications for Personalized Medicine
Drugs affect everyone differently. That’s why it’s so hard to find the right medication and right dosage to treat people with depression, for example, or why certain people don’t seem to get much relief from painkillers. That’s why the prospect of 3D printed medication is so exciting. Companies like FabRx are working to create medicines with personalized doses through 3D printing. Not only does 3D printing allow for different medications to be combined in one dose, but, as a new study shows, dosages can also be customized to suit people with different metabolic rates. The study, entitled “Extrusion 3D Printing of Paracetamol Tablets from a Single Formulation with Tunable Release Profiles Through Control of Tablet Geometry,” was written by a group of researchers from the University of Nottingham and GlaxoSmithKline.
“Personalised medicine is defined as a customization of health care to individual patients through linking diagnostics and treatments with genetic testing and emerging technologies such as proteomics and metabolomics analysis,” the researchers state. “The main advantages of this approach are to increase the effectiveness of the prescribed treatment regimen and to minimise their adverse effects such as those linked to overdosing of drugs with a narrow therapeutic index such as digoxin and anti-clotting agents.”
Paracetamol, or acetaminophen, is one of the most commonly used over-the-counter painkillers, so the researchers selected it as the subject for their proof of concept study. Work has been done before using FDM 3D printing to formulate paracetamol tablets, they note, but the high extrusion temperature limits the potential active ingredients to only heat-stable ones. Other methods like SLA and ink-jet printing use excipients that are not generally recognized as safe, however, so FDM was chosen for the study.
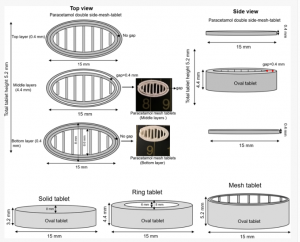 A regenHU 3D bioprinter was used to print paracetamol into three different tablet geometries – solid, ring and mesh. The outer dimensions of the tablets were kept in the same oval shape, but the inner geometries were varied, as were the number of layers. The weights of the tablets were also kept consistent by varying their heights. The tablet surface area influenced the speed of the drug release – for example, with the mesh tablets, 70% of the drug was released within the first 15 minutes, while 25% was released from the ring tablets and 12% from the solid tablets in the same period of time.
A regenHU 3D bioprinter was used to print paracetamol into three different tablet geometries – solid, ring and mesh. The outer dimensions of the tablets were kept in the same oval shape, but the inner geometries were varied, as were the number of layers. The weights of the tablets were also kept consistent by varying their heights. The tablet surface area influenced the speed of the drug release – for example, with the mesh tablets, 70% of the drug was released within the first 15 minutes, while 25% was released from the ring tablets and 12% from the solid tablets in the same period of time.
Notably, each of the tablets contained the same dosage of paracetamol, but the different release rates meant that they would affect people in different ways. These release rates could, therefore, be tailored to specific patients’ metabolisms for the most effective treatment.
“The demonstrated ability to use a single unmodified formulation to achieve defined release profiles presents opportunities to optimise or personalise medicines during formulation development and in clinical use,” the researchers explain. “For example, relatively straightforward personalization of medicines would be possible for individuals with different metabolism rates due to their genetic makeup for certain drugs and hence could address issues where people who metabolise drugs slowly may accumulate a toxic level of a drug in the body or in others who process a drug quickly and never have high enough drug concentrations to be effective.”
Any drug is dangerous when taken in too-high doses, but some people tend to go overboard with painkillers such as paracetamol, because, as the researchers point out, they metabolize the drugs too quickly for them to be effective and thus think that more is better. More is toxic, in fact, but programming drugs so that their release rates are tailored to each individual’s metabolism means that the same dosage can be taken by different people and still have the proper effect on each one.
If this study could be applied to painkillers only, it would still be big news, but its potential goes beyond just paracetamol. Adverse effects could be minimized from drugs such as anticoagulants and antidepressants, even as they are tailored to be more effective to each individual patient. The prospect of personalized medicine through 3D printing has a lot of promise; one day we may look back on our current “one dosage fits all” standard as primitive medicine.
Authors of the paper include Shaban A. Khaled, Morgan R. Alexander, Derek J. Irvine, Ricky D. Wildman, Martin J. Wallace, Sonja Sharpe, Jae Yoo and Clive J. Roberts.
Discuss this and other 3D printing topics at 3DPrintBoard.com or share your thoughts below.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
DMG Mori Joins $10M Defense 3D Printing Program
To look at the Biden administration and the Trump administration that succeeded it and find areas of policy overlap is obviously a bit of a challenge. But such areas certainly...
Where the Money Is Going: The New Infrastructure Landscape
This is Part 1 of a two-part PRO series examining where infrastructure investment is flowing and how those trends are reshaping manufacturing, energy, logistics, and additive manufacturing. Part 2, by...
First Containerized System from AML3D Now Operational at US Navy AM CoE
Shipbuilding giant Austal USA recently announced the launch of the Digital SEA (Secure Exchange for Additive) platform, which should play a major role in expanding accessibility to the sorts of...
INDOPACOM Advanced Manufacturing Team Saves Thousands Per Week at Joint Exercise in the Philippines
In the summer of 2025, the US Indo-Pacific Command (INDOPACOM) opened a new advanced manufacturing facility at Schofield Barracks, the Hawaiian home of the US Army’s 25th Infantry Division. INDOPACOM...
















































