3D printed medical models in 3D Systems’ Healthcare Technology Center lobby [Photo: Sarah Goehrke for 3DPrint.com]
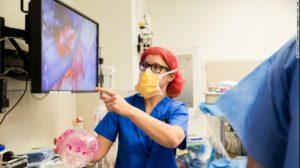
A case that has held the interest of many over recent months, CNN has been reporting with unprecedented OR access on the case of twins Jadon and Anias McDonald, twin boys born conjoined at the brain. In the Children’s Hospital of Montefiore (CHAM) operating room alongside the surgical team and CNN team were two additional observers, present from 3D Systems and there to see 3D printed models put to use directly alongside the patients.

Dr. James Goodrich holds the 3D printed model of Jadon and Anias McDonald’s conjoined skulls [Photo: CNN]
Before getting into the details of the surgery and presenting the full case study, Weimer led those of us gathered on a complete tour of the Healthcare Technology Center so we were first able to build up a basis of understanding of the technologies used in this and many other medical cases.
“It is the nature of our business to see abnormal content,” Weimer told us.
We followed another case study as we met biomedical engineers around the office, looking at the case of a cranial deformity that required that surgeons cut off and reshape the top of a child’s skull. Using CT- and MRI-based data in DICOM format, the engineers take a series of 2D data and bring it into the third dimension. Presently using off-the-shelf software for the data, the engineers use the generated 3D data for content preparation, ready to interact with surgeons for clinical input via screen sharing technology to discern exactly what will be useful on a per-case basis. For the case of the cranial deformity, there was an interactive session with the surgeon to compare with a typical skull shape, using a manual process based on predetermined surgical techniques; there is no way to protocolize this process due to the specificity demanded for each individual patient. The team has become savvier in their approach, as the longer they work directly with clinical teams the more they know the right questions to ask. As we continued around the office, which is ringed with those focusing on digital workflow, with customer service and HR in the middle of the circular setup, we could see that most of the workforce at the facility is concentrated on content creation; we were also halfway around the ring of the office before anyone even brought up 3D printing. Each patient model and guide is completely custom-designed, and the team uses Geomagic Freeform software, benefiting from the haptic feedback possible in the system to feel and touch the model, ensuring smooth edges and proper positioning. In briefly testing this out hands-on, I immediately used the haptic pen to accidentally decimate about half of a patient’s skull; fortunately, the undo command works quite well in these systems, and those using them day-to-day have much better control over the delicate settings. (Due to patient confidentiality concerns, note that there are no photos available of this part of the tour.)
Following a close look at the computer worksystems of the office, Weimer led our small tour into the facility’s labs. We started in the Simulation Lab, where the 3DS team had set up simulators including the GI Mentor Express (ready to go for a charming colonoscopy procedure), ANGIO Mentor setup for cardiac procedure, U/S Mentor for ultrasound and echocardiogram, and LAP Mentor for surgery. 3DS has been active in this area since the 2014 acquisition of Simbionix; additionally, the center itself has grown following its 2014 acquisition, as it began operations as Medical Modeling Inc. Given the opportunity to interact with these virtual surgical planning systems, including a training game using haptic feedback to work on tool dexterity within the system, I learned that I will not soon be changing careers to focus on laparoscopic surgery.
 We moved next to the various 3D printing labs, where we saw:
We moved next to the various 3D printing labs, where we saw:
- Multijet Printing Lab
- Using flexible materials useful for soft tissues, the ProJet 5500X can blend two materials, creating for example a cardiac model of a soft material valve with a hard material calcific deposit
- These models can be useful in explaining to patients and families in total detail what is happening
- Colorjet Printing Lab
- Older technology in this lab features gypsum materials that offer benefits in speed and full-color printing, additionally housing original Z Corp machines
- A full-color model of a three-year-old’s heart with an anomalous branch was illustrative of a useful patient education model
- Stereolithography Lab
- The model of sled hockey champion Mark Weimer’s spine was made here, using photoreactive dye capabilities
- This lab produces biocompatible and sterilizable materials that are useful in creating OR-ready cutting guides
- SLS Lab
- This large lab currently houses one machine, using nylon to create such products as scoliosis braces and single-use disposable tweezer sets, using powder-based laser sintering technology benefiting from thermoplastic flexibility rather than thermoset rigidity
- Using material recycling equipment, this machine can use a 60/40 blend of recycled/virgin powders; one recycling station is capable of feeding two machines
- Direct Metal Printing Lab
- Here, technicians create titanium implants, tools, and devices using hot isostatic pressing and heat treating, as materials must meet ASTM standards
- The first FDA-cleared 3D printed titanium medical implant came out of this lab
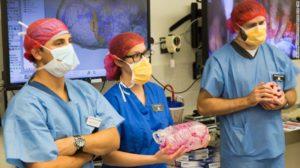
Finally, we sat down to hear directly about the McDonald conjoined twins’ case, having all gained an understanding of the technological capabilities at hand that made this work possible. Models created from the boys’ medical records included a vertical model created in full-color gypsum showing in a true-to-life look at their conjoined heads, as well as in-depth anatomical models. Used in the operating room were a model showing both skulls and, with a photoreactive dye, their highlighted veins that showed where critical bloodflow existed, as well as a cutting guide that showed surgeons where planned cuts were to be made, including those that would lead to ensuring each boy, once separated, had enough cranial material and skin to close his own newly complete and separate skull.
Weimer showed photos straight from the operating room, detailing the feelings of alternating tension and elation as the 27-hour final procedure was carried out. The boys, born in September 2015, were 13 months old as of their final October separation surgery, following four procedures over seven months. The birth rate for craniopagus twins, joined at the head, is approximately one in 2.5 million live births.
“This intricate procedure was greatly enhanced by cutting edge 3D technology that enabled the surgeons to see inside the boys’ brains… This is Montefiore at its best: sophisticated science, medicine and patient care are at the heart and soul of what we do,” said Steven M. Safyer M.D., President and CEO, Montefiore.
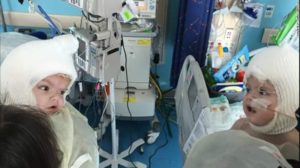
The surgery, as we know, was ultimately successful — and so we have also recently heard that, finally, both boys are now home with their parents, Nicole and Christian, and big brother Aza. Below are several photos from CNN showing the boys’ 3D printed medical models:
- The boys, separated, see each other for the first time from their hospital beds
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Asia AM Watch: China’s 5 Million-Printer Export Year Signals Desktop AM at Scale
For years, a lot of the discussion around China and additive manufacturing has focused on industrial competition. Can Chinese companies move into higher-end markets? Can they challenge Western machine makers...
Creality Launches Filament Maker M1 & Shredder R1, Letting Makers Reuse Waste, Cut Costs, and Create Their Own Filament
From Printing Objects to Shaping Materials Desktop 3D printing has made on-demand creation more accessible than ever. Yet one critical part of the process remains fixed: the material itself. Most...
Bambu Lab 3D Prints Miniature Playground City for Kids in China
Bambu Lab has partnered with meland to open what they describe as China’s first 3D printing creativity center for children. The new space, officially named “meland x Bambu Lab,” launched...
Bambu Lab Says 2025 Was a Breakout Year: 10 Million Monthly Users and Real Business Growth
Chinese 3D printer maker Bambu Lab reported strong results for 2025, showing that the company’s push into community and small-business 3D printing is working. The numbers suggest consumer 3D printing...