3D Printed Bolus Protects Cancer Patients During Radiation Therapy, May Cut Treatment Costs Substantially
 Electron Beam Therapy (EBT) is a type of radiotherapy that uses electrons to treat the tumor site. Because of the finite range of electron beams the dose falls off rapidly leaving deeper tissue unaffected by the treatment. Superficial tumors such as those present in skin cancer are a primary location of treatment for EBT. In addition, EBT is sometimes used in conjunction with radiation directly after a mastectomy or lumpectomy.
Electron Beam Therapy (EBT) is a type of radiotherapy that uses electrons to treat the tumor site. Because of the finite range of electron beams the dose falls off rapidly leaving deeper tissue unaffected by the treatment. Superficial tumors such as those present in skin cancer are a primary location of treatment for EBT. In addition, EBT is sometimes used in conjunction with radiation directly after a mastectomy or lumpectomy.
The scope of each treatment is determined by modifying the amount of energy used. One means of modifying the amount of energy is through the application of a bolus to the site to be treated. A bolus is a mass that has been shaped for application to a particular area where its thickness is differentiated in order to modify the energy that is allowed to pass through it.
Researchers at Dalhousie University and the Nova Scotia Cancer Center in Halifax recently released a paper in the Journal of Applied Clinical Medical Physics in which they discussed the use of 3D printing as a mechanism for creating boluses for electron radiation therapy. An exacting method for the creation of each bolus is required as dosage patterns must be tailored to each patient’s surface structure and cancer presence.
To create a bolus the research team developed an in-house algorithm taking into account dose distribution in terms of coverage, conformity, and homogeneity within the targeted area. The results of the calculation indicate the exact form needed to administer the appropriate dosage. The team had previously studied other methods for bolus design creation, such as fabrication with a milling machine from an electron pencil beam design. Those creations presented problems because of the margin of error inherent in the processes used for their creation, and because of irregularities in individual patient’s surfaces. Therefore, unnecessarily high doses could be delivered to critical structures and tissues immediately underlying the targeted area.
The design of each bolus is calculated on a 2.5mm grid using Eclipse software. The software models deeper and shows surfaces according to the coordinates that are input. In addition, as each person’s tissue is different and unique, accommodations must be made for potential tissue heterogeneity. The model is tested and refined as many times as necessary to account for all of the patient variables. While this method is generally useful when the geometries are simple it is more difficult to create an accurate form in the presence of more aberrant features.
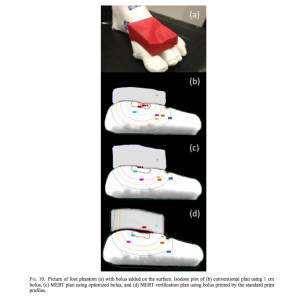 The researchers hypothesized that the complex geometry created by these variables made 3D printing and ideal fabrication method for boluses. For this proof-of-concept investigation careful calculations performed on model body surfaces (phantoms) were converted into stereolithography files to be printed in solid polylactic acid on a Makerbot Replicator 2. The researchers used Makerware, also produced by MakerBot, to define printing quality and create their print profile. The boluses were printed with 100% infill in order to make it completely solid, rather than filled with a low-density honeycomb pattern.
The researchers hypothesized that the complex geometry created by these variables made 3D printing and ideal fabrication method for boluses. For this proof-of-concept investigation careful calculations performed on model body surfaces (phantoms) were converted into stereolithography files to be printed in solid polylactic acid on a Makerbot Replicator 2. The researchers used Makerware, also produced by MakerBot, to define printing quality and create their print profile. The boluses were printed with 100% infill in order to make it completely solid, rather than filled with a low-density honeycomb pattern.
After the bolus is reprinted and applied to the fans and services, a CT scan of the combination was taken to verify fitting and to calibrate final dose distribution. It is during this process that the fit accuracy of the 3-D printed bolus could be closely studied. It was determined that given the data collected there is no expectation that the bolus created by the 3-D printer would lead to any clinically significant errors in dose distribution. In fact, the team discovered that the 3D printed bolus reduced the quantity of electrons previously impacting surrounding tissue areas.
The importance of such a reduction in electron “spillage” becomes particularly apparent when the researchers applied the bolus to a phantom head. It is clear to see, from the image provided, that the radiation therapy is to be applied near the area of the eyes, making containment vital to preventing damage to the sensitive tissues. And indeed the researchers found a decrease in the presence of electron dosage in the eye of approximately 20%.
 The data gathered from this study allowed the researchers to develop an algorithm that will optimize bolus design and produce data for fabrication of a 3D printer. This will improve the accuracy of the dose distribution, leading to decreases in damage to healthy tissues surrounding the treatment area. In addition, as the cost of 3D printing continues to decline, this method will allow for lower-cost, high accuracy, perfectly individualized bolus creation on demand. This process offers the advantage that the patient does not need to be present during fabrication.
The data gathered from this study allowed the researchers to develop an algorithm that will optimize bolus design and produce data for fabrication of a 3D printer. This will improve the accuracy of the dose distribution, leading to decreases in damage to healthy tissues surrounding the treatment area. In addition, as the cost of 3D printing continues to decline, this method will allow for lower-cost, high accuracy, perfectly individualized bolus creation on demand. This process offers the advantage that the patient does not need to be present during fabrication.
3D printers may become standard equipment in hospital cancer centers in the near future, further reducing medical costs and simplifying logistics. The benefits to the field of medicine from 3D printing have been demonstrated again and again. They lie not only in the technical capabilities of the machinery but also in its ability to lessen discomfort and stress for all involved. These “soft” advantages may, in the end, demonstrate the humanizing benefits of advanced technology. Let’s hear your thoughts on this innovative new use of 3D printing within the cancer treatment forum thread on 3DPB.com.
[Source: Jacmp.org]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
AM Drilldown: the Beginning of 3D Printing’s Next Phase in the Energy Sector
For much of the last decade, many have pushed an unjustifiably optimistic view of global energy consumption, along the lines of, fossil fuels are “on their way out.” Sadly, this...
Mikhail Gladkikh on Digital Inventory: “Think of It as Netflix for Manufacturing”
As manufacturers continue looking for ways to reduce supply chain risk, additive manufacturing (AM) is increasingly being discussed as more than just a production tool. Across aerospace, energy, defense, and...
ROBOZE Buys Dimanex Assets to Build “Physical AI” Platform
Dutch firm Dimanex got its start as an MRO platform for the railways. The company had a contract with the Dutch Army in 2018, and later that year signed one...
3D Printing Financials: Xometry Surges After Record Quarter and Siemens Deal
Shares of Xometry (Nasdaq: XMTR) surged on Thursday, May 7, after the company reported record first-quarter 2026 results and announced a major partnership with Siemens. The stock climbed as much...















































