Doctors use 3D Printing to Safeguard an Unborn Baby’s Life
3D printing technology is starting to become commonplace for several medical applications, including dental work, hip replacement, prosthetics and custom made surgical guides that reduce procedure time by hours. More recently, a process to convert MRI and echocardiographic data into a 3D model that can be printed and used for surgical pre-planning has started to be used more often, especially for heart surgery. Unfortunately the programs and printers used in many of these applications are still prohibitively expensive and often not covered by patients’ insurance plans. But the technology is there, and doctors and surgeons always want the best tools available to them while working with their patients, so they are starting to find some creative ways of using the technology with the hope that it will become more affordable.
Recently a group of doctors at the University of Michigan were examining the ultrasound data of a 22-year-old mother-to-be. She was 30 weeks into her pregnancy when they noticed a large mass on the face of the fetus. The doctors didn’t know what the abnormality was, and were afraid that the mass would block the airway of the baby when it was born. If that was the case then the doctors would need to quickly intubate (place a plastic tube into the windpipe) the baby at birth to help with breathing. That could risk the life of the baby, so obviously the doctors wanted to get more information so they could be prepared for whatever needed to be done.
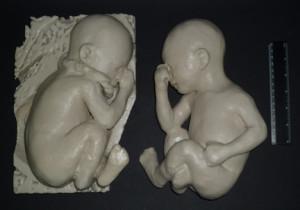
The young mother was given a second ultrasound, however the new imaging still didn’t reveal enough information about the mass because of the the positioning of the fetus. So the doctors tried an MRI, but again they couldn’t get enough data on the mass be sure that the fetus’ airway would be clear after birth. So as a last ditch effort to safeguard the health of the fetus, the doctors turned to 3D printing to help them get a clearer picture of what they were in for. They started by using a specialized MRI process to capture enough data to build a 3D model and then 3D printed it so they could get a clearer look at the placement of the mass on the fetus’ face.
“In this specific instance where airway distress is a major possible issue, I think [3D printing] potentially can help to revolutionize that field. It really provides a new tool so that doctors are much better prepared to deal with airway problems or other congenital anomalies that they need to diagnose critically right when babies are born. I would suggest that there’s no replacement for being able to hold an object in your hand and have this tactile three-dimensional ability to assess something. When you’re actually holding a model of a skull, for example, in your hand, it’s a whole different experience,” explained Dr. Albert Woo, the director of the 3D printing lab at Washington University School of Medicine in St. Louis, who was not involved in this study.
Once the doctors had a 3D printed model of the fetus’ face it became instantly clear that the baby had a cleft lip and palate deformity that wouldn’t cause any airway obstructions. Thankfully, a cleft lip is a relatively harmless birth defect that is generally easy to correct with plastic surgery. The baby was delivered without incident and was able to be discharged without any difficulties.
“The neonate was born with a protuberant cleft lip and palate deformity, without airway obstruction, as predicted by the patient-specific model,” noted the research team in their study abstract. “The delivery was uneventful, and the child was discharged without need for airway intervention. This case demonstrates that 3D modeling may improve prenatal evaluation of complex patient-specific fetal anatomy and facilitate the multidisciplinary approach to perinatal management of complex airway anomalies.”
This was the first time that 3D printing technology was used to diagnose a facial deformity and assess the severity of airway risk with a fetus in utero. The team of doctors submitted their findings to the Oct. 5 online edition of the medical journal Pediatrics where they reported that 3D printing technology took the guesswork out of a high-risk pregnancy. The case report, “Antenatal Three-Dimensional Printing of Aberrant Facial Anatomy,” was written by a team including Kyle K. VanKoevering, MD; Robert J. Morrison, MD; Sanjay P. Prabhu, MBBS; Maria F. Ladino Torres, MD; George B. Mychaliska, MD; Marjorie C. Treadwell, MD; Scott J. Hollister, PhD; and Glenn E. Green, MD.
Discuss this story in the 3D Printed Fetus forum thread on 3DPB.com.
[Source: Medical Xpress]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
3D Printing News Briefs, April 4, 2026: 3D Printed Food, Cocoa Press, & More
We’re starting off with 3D printed food in this weekend’s 3D Printing News Briefs, followed by some business news about Cocoa Press. Then we’ll move onto a metal additive manufacturing...
3D Printing News Briefs, March 26, 2026: AMUK, IP Dispute, Asbestos, & More
We’re kicking off today’s 3D Printing News Briefs with an America Makes Project Call, and then moving on to additive manufacturing in the UK. Then we’ve got some legal news...
3D Printing News Briefs, March 14, 2026: Student Grant, Automation, DfAM, & More
In this weekend’s 3D Printing News Briefs, we’ll start with event sponsor and competition news from Dyndrite, and then move on to a new metal 3D printing system from Eplus3D....
OCL Architectural Lighting Uses 3D Printing for Luminaries
OCL Architectural Lighting is using material extrusion to make luminaries. The luminaries are intended for commercial lighting and are available in the Printz line. The line is “specification-grade lighting,” a...