3D Printed Bioplotting May Offer Comfort to Diabetes Patients
 Type 1 diabetes is a malady usually diagnosed in children and young adults, once known as juvenile diabetes. Only five percent of diabetes sufferers have this form of the disease; in Type 1 diabetes, the body fails to produce insulin, a hormone the body uses to convert sugar, starches, and other food into energy.
Type 1 diabetes is a malady usually diagnosed in children and young adults, once known as juvenile diabetes. Only five percent of diabetes sufferers have this form of the disease; in Type 1 diabetes, the body fails to produce insulin, a hormone the body uses to convert sugar, starches, and other food into energy.
With a combination of insulin therapy and various other treatments, even the youngest children can learn to manage their condition and live long, relatively healthy lives.
One of the ways patients can compensate for their lack of insulin is via an as-yet experimental procedure. Called pancreatic islet transplantation, it’s a process in which clusters of cells are transplanted from the pancreas of a healthy donor.
There is a major side effect of this treatment. It requires that a patient undergo ongoing doses of immunosuppressant drugs to prevent the patient’s body attacking the foreign, transplanted cells.
Now a new approach offers relief from that issue by using a 3D printed scaffold as a delivery technique to manage the condition.
In Type 1 diabetes, a patient’s system can display low levels of glucose in the blood. The condition is known as hypoglycemia, and its effects are both unpleasant and potentially lethal.
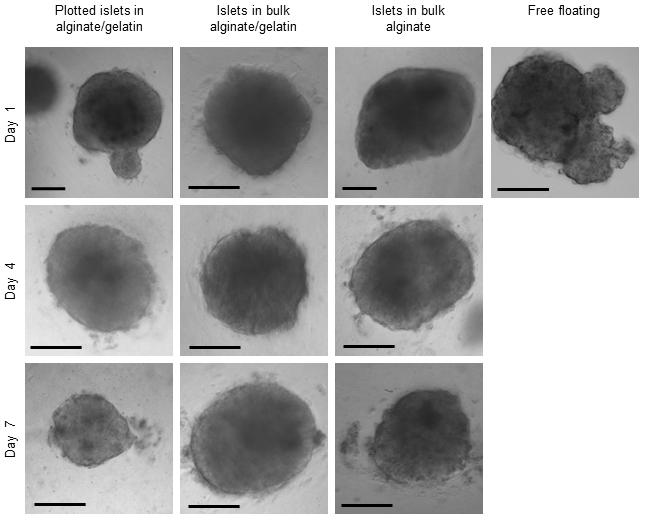
Now researchers at the University of Twente in the Netherlands have built scaffolds they say will improve the success rate of pancreatic islet transplantation by embedding the islets within a mixture of alginate and gelatin.
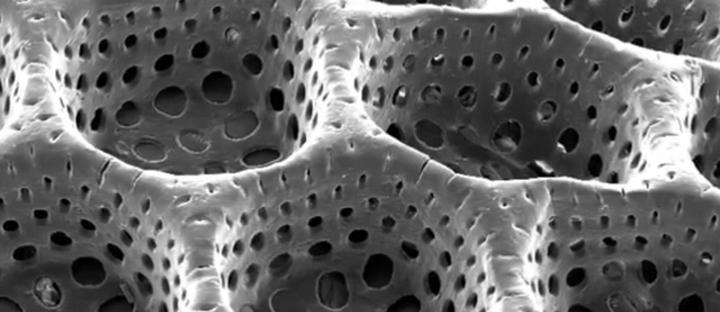
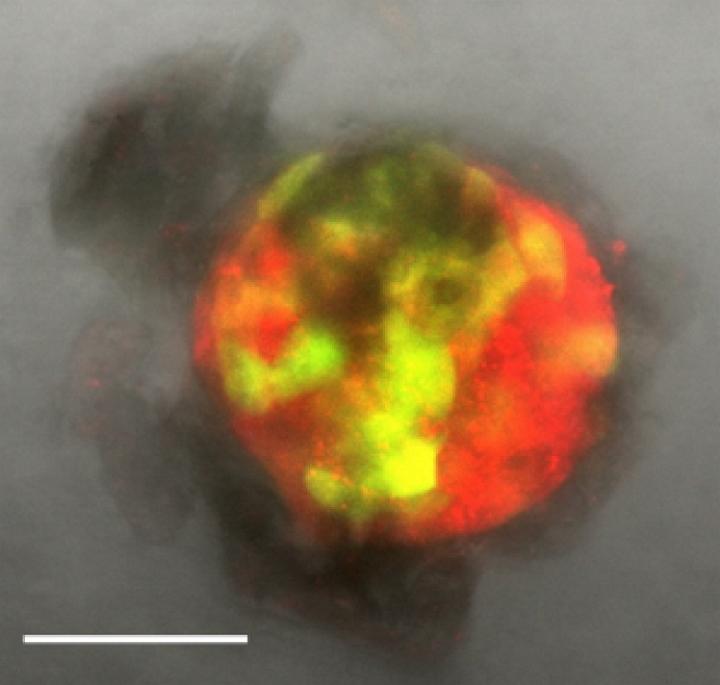 They call the process bioplotting, and it results in a porous, 3D printed structure which allows for an optimum exchange of glucose and insulin.
They call the process bioplotting, and it results in a porous, 3D printed structure which allows for an optimum exchange of glucose and insulin.
In fact, lab results have shown these 3D printed islets and scaffolds are every bit as capable of performing the role as the islet cells they replace and that they provide the necessary protection against the immune system response of the body.
Dr. Aart van Apeldoorn, a co-author of the research, says this “immunoprotective scaffold” may be developed by using a non-degradable hydrogel. The hydrogel includes a proper mesh size which can block antibodies and immune system-specific cells while the mesh remains large enough to allow for insulin diffusion.
“If we are to improve the success of this treatment for Type 1 diabetes, we need to create an implant in which islets are embedded, or encapsulated, from a material that allows for very efficient oxygen and nutrient supply, and quick exchange of glucose and insulin, while keeping the host cells out,” says van Apeldoorn.
According to van Apeldoorn, these “macroporous scaffolds” ensured that the islet cells held within them wouldn’t migrate uncontrollably throughout the rest of the body once transplanted into the donor site.
Results of the research were published in the journal Biofabrication.
What do you think of this biofabricated treatment, which may one day help Type 1 diabetics avoid ongoing immunosuppresant treatments? Let us know in the 3D Printed Bioplotting forum thread on 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
You May Also Like
RAPID 2025: Stratasys & trinckle Announce Strategic Software Partnership
News continues to flood in from last week’s RAPID+TCT 2025, including a new partnership between AM market leader Stratasys and Berlin-based software company trinckle. By automating important steps in fixture...
RAPID TCT 2025: Spring in the Paris of the Midwest
I’m going to go out on a limb here and say that whomever coined the phrase Detroit: Paris of the Midwest, had not spent a lot of time in Paris...
3D Printing Financials: 3D Systems Looks to Bounce Back in 2025
After a challenging year for the industry, 3D Systems (NYSE: DDD) ended 2024 with results pointing to a reset, laying the groundwork for future profitability. The company didn’t post strong...
Printing Money Episode 27: Q4 2024 Public 3D Printing Earnings Review with Troy Jensen, Cantor Fitzgerald
Q2 2025 has already begun, but public markets reporting has only just finished with Q4 2024. To tie a bow on Q4 2024, we are thankful to have Troy Jensen...