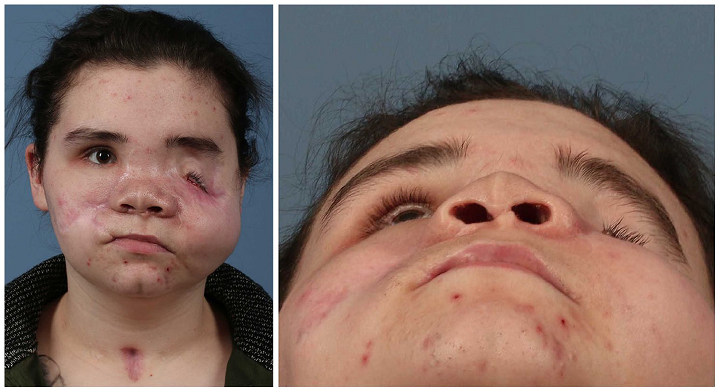
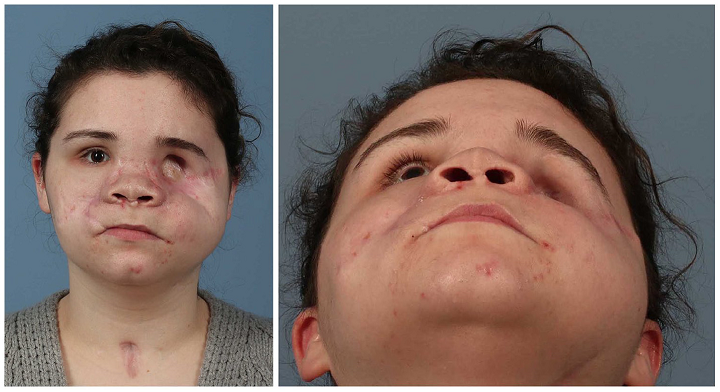
3D Printing and Virtual Surgery Help Repair Damage to Patient’s Face
3D printed surgical guides and virtual surgical planning (VSP) have been used in many types of procedures, such as knee replacement, spinal surgery, and reconstruction of chest walls and faces. But when it comes to reconstructing complex maxillofacial deformities, this kind of computer-aided technology is used far more often for bony reconstruction than for soft tissue. A team of researchers from the University of Michigan published a paper, “Using a 3D Printed “Phantom of the Opera” Soft Tissue Surgical Guide for Complex Facial Reconstruction,” about their work utilizing VSP and 3D printed guides to help a patient suffering complex soft tissue damage from a gunshot wound.
“In ballistic injuries there is often disfiguring damage to the soft tissue, with destruction of anatomic landmarks making satisfactory soft tissue reconstruction a unique challenge,” the abstract states. “By combining tangible surgical models and aesthetic judgment in a team setting, it is possible to optimize the efficiency and accuracy of soft tissue reconstruction in the setting of complex facial deformities.”
Ballistic facial injuries are extremely challenging to reconstruct, as both bony and soft tissue are damaged, and often there are tissue burns and contamination as well. For their study, the researchers presented a case that integrated VSP, 3D printed surgical guides, and anaplastology—a branch of medicine dealing with the prosthetic rehabilitation of an absent, disfigured, or malformed anatomically critical location of the face or body—to provide a 19-year-old female patient with “improved facial symmetry and orbital prosthesis accommodation.”
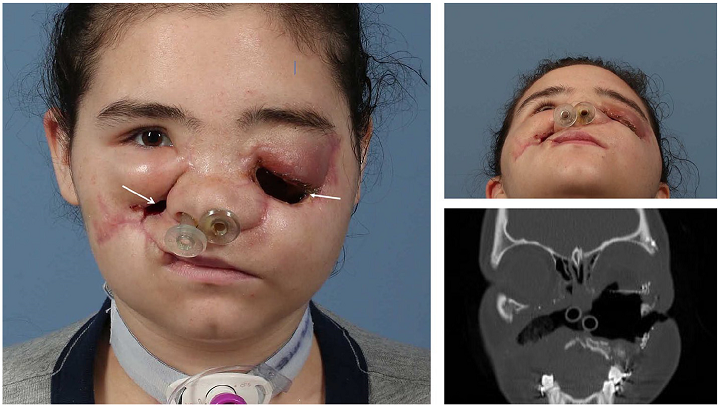
Preoperative photograph of a 19-year-old female with history of facial injury, status post debridement, ORIF of facial fractures, left globe enucleation. Arrows indicate antro-cutaneous fistulas.
Initially, the patient went to another facility, presenting with major facial injuries such as left globe rupture and fractures of the bilateral orbits, zygomas, maxilla, nasal bones, and septum. While there, she received a tracheostomy and “multiple facial washouts,” had her fractures fixed, and her left eye enucleated. Unfortunately, she later developed painful “antro-cutaneous fistulas at the bilateral malar regions” and was transferred to the U Mich facility for further reconstructive surgery.
The team used a “free tissue transfer” to reconstruct all of the patient’s facial wounds, which would close the fistula and help reconstitute her soft tissue. While this helped with her pain, it unfortunately made the left side of her face heavier, which, when paired with gravity, caused major asymmetry. So they moved on from wound control to “restoring her facial contours” and getting her an orbital prosthesis.
They paired VSP mirroring technology with the dimensions of the proposed prosthesis to 3D print custom surgical guides to facilitate “precise debulking and resuspension of the left malar soft tissue and peri-orbita.” The researchers used Materialise Mimics to isolate the relevant bony and soft tissue anatomy, and then imported the image into 3Matic to create a clear model. Qualitative metrics and quantitative measurement were used to find “a sagittal plane of symmetry,” over which the unaffected part of the patient’s face was mirrored onto the left side.
“The shape of the resulting left orbital sphere was edited to the specific dimensions of the prototype orbital prosthesis provided by our anaplastologist,” they wrote.
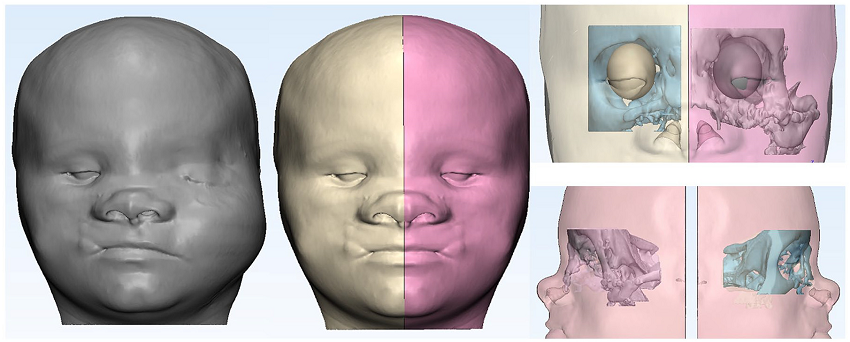
Illustration of mirroring technique to achieve facial symmetry and creation of ideal left orbit utilizing data from the patient’s unaffected side and specifications of the planned orbital prosthesis. (Materialise Mimics Innovation Suite; Belgium).
The patient approved the virtual images for her planned reconstruction, and a custom guide was 3D printed for the “left orbital debulking portion of the surgery,” and another was made for the “left malar recontouring and suspension surgery.” If you’re familiar with “The Phantom of the Opera” musical, this second 3D printed surgical guide resembles the mask that the Phantom himself wears.
“In order to maximize use of the guides intraoperatively, 2 posts were added to the external surface of the orbital guide, and 2 matching slots were created on the internal surface of the malar mask. This allowed for implantation of the guides separately or in conjunction depending on intraoperative need,” the researchers explained. “Square cells were also cut from the malar mask to create a lattice that would allow the surgeons to visualize the patient’s face when the guide was in place.”
The guides were printed out of biocompatible Dental SG resin on a Form 2. I’ll leave out all of the surgical details, but suffice it to say the procedures were all successful, and eight months later, the patient showed major improvements “in the symmetry of her midface and periorbital regions.”
“Although we have only presented 1 patient with limited follow up, this case demonstrates a new application of computer aided technology and adds to the armamentarium of the maxillofacial surgeon,” they wrote.
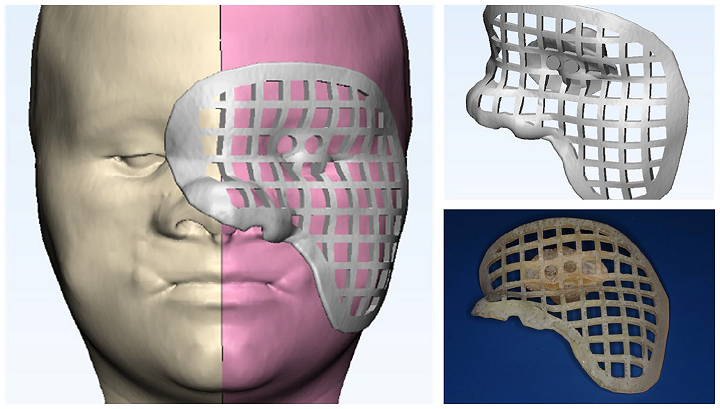
3D printed models of the surgical guides for left orbit and cheek. The guides were modified to be interlocking. The malar mask had a lattice structure that allowed for better visualization of underlying structures.
While things worked out here, there are still challenges in using computer aided technology to reconstruct soft tissue, such as “the natural irregularity” in a human face and the fact that soft tissue is very sensitive to inflammation, as well as dynamic, meaning it can’t be totally immobilized.
“As such, deformational forces and involuntary activation of facial muscles during the course of imaging can distort the measurements and lead to inaccurate calculations,” the researchers explained.
“Surgeons must therefore still use their judgment and account for the long-term effects of scar tissue and gravity when developing the virtual model.”
Additionally, there can be increased costs if the hospital has not already adopted VSP, 3D printing, and CAD/CAM technologies. But overall, I’d call this a success story.
“Although it cannot replace clinical judgment, computer aided technology can produce better, more accurate outcomes and should be considered for soft tissue reconstruction,” the team concluded.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
The Hidden Cost of Lost Engineering Intent
Recent reporting on the UPS MD-11 engine separation on Flight 2976 has understandably focused on the immediate question: what happened? The investigation will determine that, as it should. Serious engineering...
3D Printing News Briefs, May 28, 2026: Continuous Fiber Reinforcement, Bioprinted Trachea, & More
In today’s 3D Printing News Briefs, America Makes announced the winners of its JAQS-SQ Project Call. Axtra3D is partnering with Keystone Industries to expand its dental material ecosystem, while BigRep...
Stratasys Acquires Markforged, Analysis of AM’s Latest Consolidation Move
A very long time ago, in 2023, the additive manufacturing (AM) industry was enraptured over the attempts by a large chunk of its publicly traded original equipment manufacturers (OEMs) to...
Why Additive Manufacturing Has Finally Earned Its Place on the Production Line
For years, the conversation around additive manufacturing followed a predictable script. Engineers would acknowledge its usefulness for prototyping – faster iterations, cheaper design validation, no tooling to worry about –...