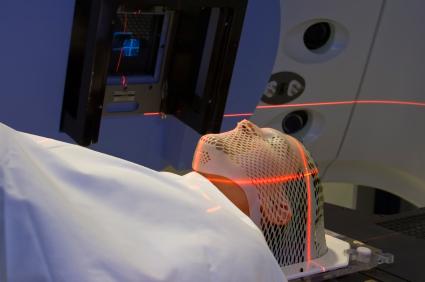
 Cancer patients undergoing brain or head and neck radiotherapy are required to be immobilized, which is certainly not always popular with those undergoing the procedure, who may already be suffering from anxiety. To make things worse, in order to be immobilized completely during the procedure, it is crucial that they are wearing a fitted mold to prevent motion. Having the mold made is a whole process in itself before the procedure can begin.
Cancer patients undergoing brain or head and neck radiotherapy are required to be immobilized, which is certainly not always popular with those undergoing the procedure, who may already be suffering from anxiety. To make things worse, in order to be immobilized completely during the procedure, it is crucial that they are wearing a fitted mold to prevent motion. Having the mold made is a whole process in itself before the procedure can begin.
In a recent study produced by the Journal of Radiotherapy in Practice, over half of the patients describe the process of having a mold made as ‘horrific.’ Many of them also described the process as ‘uncomfortable.’
Topping that off with molded shells that quite often do not fit appropriately, the anxiety levels are heightened for patients — enough so that researchers centered their study around the creation of molded shells through 3D printing that could be created from data conveniently already existing in the form of a CT scan. The process would increase the comfort level for the patient and save a great deal of time in preparing a molding.
Radiotherapy is a type of cancer treatment which uses high-energy rays to zap cancer cells. The procedure has to be precisely aimed directly at specific areas to have effect, and it’s not a procedure anyone wants immediately repeated; therefore, It’s important to have the head shell or molding during radiotherapy because the patient must lie still. The mold or shell holds the head and neck in the correct position, and is fixed to the radiotherapy treatment table.
The shell is made in what is usually a 30-minute process, and there are a number of factors involved in the process which make it even more inconvenient, such as hairstyle, dental issues, facial hair, and more. The current method for using molds during radiotherapy in the UK is in using the Orfit mask, which is made through soft draping, in a process where soft plastic is draped over the head and shoulders of the patient and it is molded to their body. Another method for making 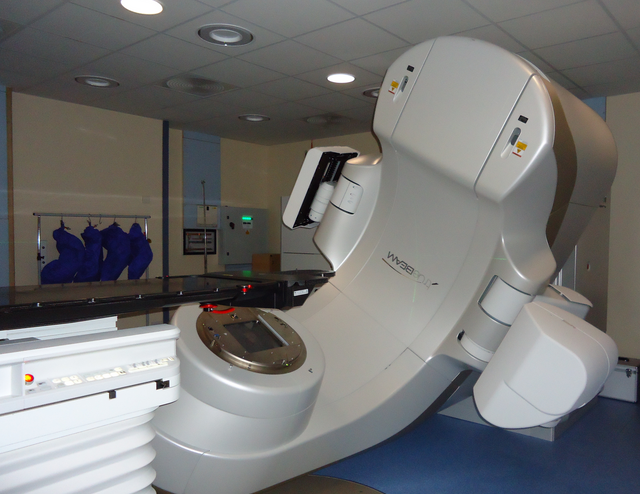 the mask or mold is completed through use of high-temperature thermoplastics which are molded onto a plaster of the patient’s face.
the mask or mold is completed through use of high-temperature thermoplastics which are molded onto a plaster of the patient’s face.
In the study, the multiple researchers confronted the issue of patient discomfort and anxiety over the radiotherapy molds and evaluated whether it would be possible to 3D print them and if the time, expense, and product outcome would make it a feasible idea. Their focus was on 3D printing the front of a test shell, and measuring whether it would interfere with the dose being given to the patient in radiotherapy. The actual material used in 3D printing was of obvious concern as well.
The researchers reconstructed the head and neck of a whole body scan at a slice thickness of 3.75 mm and processed Digital Communications in Medicine (DICOM) data from MRI or CT scans with data relating to items such as masking, segmenting, conversion of the data from black to white, conversion to a hollowed out positive head, creation of a negative shell, and then conversion to an .stl file format for 3D printing. Visijet clear and EOS PA 3200 were the materials used, and researchers point out that any materials used for 3D printing of the shells should be the same or of even better quality to reach the same standard or better.
Using a Z-Corps 650 printer from 3D Systems, researchers 3D printed their shells and set out to measure how they would affect the dosage being sent through the radiotherapy. Their findings were quite positive. Using three different types of materials, they found that the dosimetric properties of the 3D printing were promising in that all materials produced a small decrease in the dose of radiotherapy of up to one percent. All of the materials also produced an increase in skin dose between 54 and 80 percent, which could be minimized in using thinner materials, or creating holes in the masks, as having it increased too much is obviously not a good idea.
While 3D printing of the shells proved to be a bit more expensive than the more conventional methods, the researchers point out that this can be reduced if multiple masks are created in the same build chamber. It’s also possible that multiple hospitals could coordinate to purchase 3D printers together, thus reducing upfront cost.
The bottom line was that the items can be feasibly 3D printed without reducing the dose, saving patients the anxiety of having the molds created through direct contact with their bodies, and affordability should be not be an issue in the near future as prices have been coming down consistently.
Do you think this is something that will be helpful to patients experiencing radiotherapy? Discuss in the 3D Printing & Radiotherapy forum thread on 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
3D Printing News Briefs, March 28, 2026: TCT Asia, Distribution Agreement, FDA Clearance
We’re starting 3D Printing News Briefs this weekend with some news out of TCT Asia, and then moving on to a metal AM distribution agreement between MULTISTATION and WAAM3D. We’ll...
The Magic of AMUG as Reported by a First-Time Attendee
There’s a special kind of magic about AMUG. I’ve heard about it for years, but never experienced it myself until last week. It’s different than what you see at some...
3D Printing News Briefs, March 26, 2026: AMUK, IP Dispute, Asbestos, & More
We’re kicking off today’s 3D Printing News Briefs with an America Makes Project Call, and then moving on to additive manufacturing in the UK. Then we’ve got some legal news...
At TCT Asia 2026, China’s AM Industry Looked Ready for Scale: Part 1
Walk into TCT Asia 2026, and the first impression is density. More than 55,000 square meters across Halls 7.1 and 8.1 at Shanghai’s National Exhibition and Convention Center, over 550...
































