Cincinnati Hospital Uses 3D Printed Template to Remove Large Birth Mark on Two-Year-Old’s Face
3D printing, with the seemingly infinite innovations it offers to us from around the world, is a technology that is proving beneficial to businesses, individuals, and professionals in many sectors and for many valuable reasons. This new technology, centered around bringing digital design and concept into physical form, just generates enthusiasm, most often due to the excitement and energy resulting in the ultimate rewards—and this is certainly the case when it comes to using 3D printing in the medical field to help children.
Researchers and doctors today, in many facilities, are beginning to grasp onto 3D printing to make serious strides not only for the world, but also for specific young patients who require customized applications for healing and for surgeries.
For Dr. Thomas Sitzman at Cincinnati Children’s Hospital-Medical Center, a challenge lay ahead with the case of young Lily Hall of Whitesburg, KY. The child, only two years old, was born with a condition called linear nevus sebaceous syndrome. Lily would have to be treated and operated on for the condition as it causes not only great issue to the skin due to the large raised birthmarks, but also affects the nervous system and the eyes. The condition causes the patient irritation and pain, and the birthmarks have the potential to turn into malignant lesions.
“For us, it was never really an option NOT to do anything,” said Brandi Hall, Lily’s mother. “My husband and I knew we were going to get it removed as soon as we possibly could.”
In Lily’s case, Dr. Sitzman was using a very specialized treatment. Basically, for Lily, skin is a valuable commodity and before they could repair her skin and proceed with numerous surgeries, they needed to ‘grow’ some more skin. Sitzman achieves this through using tissue expanders which work over time, before procedures are performed.
“Tissue expanders are like water balloons,” said Dr. Sitzman, a plastic surgeon in the Pigmented Lesion Clinic at Cincinnati Children’s. “The deflated expanders are placed under the skin near the birthmark. Lily’s parents slowly fill the expanders at home over a period of three months. As the expanders inflate, they stretch the normal skin nearby. We then use that normal skin to remove the birthmark.”
 Extra care is obviously required for such a delicate surgery in such a young patient. In taking on complex treatment for this complex case, Dr. Sitzman turned to new technology as well as outside help, reaching out for the innovation and versatility offered via 3D printing, as well as enlisting the expertise of Matt Batie in the clinical engineering department at Cincinnati Children’s. Together, they were able to collaborate on a way to use 3D printing to create 3D models which would help with the surgical process, and pave the way for guidance in future procedures.
Extra care is obviously required for such a delicate surgery in such a young patient. In taking on complex treatment for this complex case, Dr. Sitzman turned to new technology as well as outside help, reaching out for the innovation and versatility offered via 3D printing, as well as enlisting the expertise of Matt Batie in the clinical engineering department at Cincinnati Children’s. Together, they were able to collaborate on a way to use 3D printing to create 3D models which would help with the surgical process, and pave the way for guidance in future procedures.
Batie’s 3D model enabled Sitzman to envision and prepare for Lily’s surgeries.
“After we scan the patient I digitally add the expanders to the model and prepare the file to print,” said Batie. “Then in a matter of hours we have a life size replica of the patient.”
Using all the tools of a special effects artist, Batie makes the 3D model using the dimensions of the patient’s head. He then used a silicone rubber that looks a bit like peanut butter, to make the 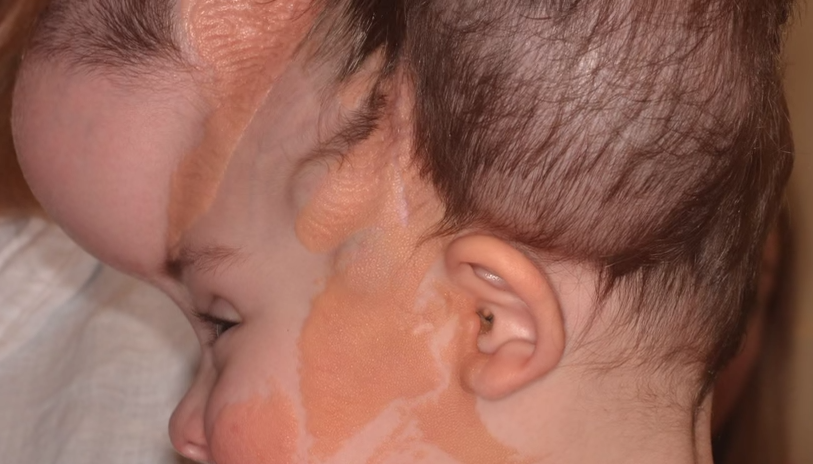 artificial skin, which covers the model in multiple layers.
artificial skin, which covers the model in multiple layers.
Dr. Sitzman was then able to use the model as a template for drawing areas where the incisions would go as well as the areas to where the skin would be moved. In essence, the 3D model becomes a complete map for Lily’s procedure. The 3D model fit to Lily’s head and scalp perfectly once she was anesthetized and on the operating table, and surgery went off without a hitch.
“Her surgery took four hours and went exactly as planned,” Dr. Sitzman said. “As soon as she was asleep, we put the new template and model on her scalp and it fit perfectly, so we were able to do the surgery exactly as we planned and rehearsed.”
With this process in place, Dr. Sitzman indeed will be able to use this type of 3D model as a tool in the future for other patients and their consequent surgeries.
“You only get one shot with how you are going to do this surgery. Being able to model each individual patient’s surgery in advance is a tremendous step forward in how we care for patients,” said Dr. Sitzman.
As is the case in many aspects of using 3D printing applications to make new breakthroughs, there isn’t any roadmap. Doctors may have little to no foundation to work from, and this is where they have to use their training in research and science, as well as applying creativity, resourcefulness, and strategy. In the medical field, this often means calling in others with expertise—especially when lives are at stake.
Using 3D printed models both ahead of and during surgery, doctors can practice and pinpoint exactly what’s needed, and where—as well as being able to explain to parents ahead of time, in 3D, exactly what they will be doing.
The bottom line is that the use of 3D models in diagnosing and pre-surgical planning is an enormously helpful tool to the surgeon, who passes on the benefits to patients with shorter operating times and better outcomes.
Have you heard of pediatric surgeons in your area using 3D printing for breakthrough procedures? Do you know an individual who could benefit from this type of technology and procedure? Tell us your thoughts in the 3D printed Template forum thread over at 3DPB.com.
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
Post-Printing at RAPID 2026: PostProcess Technologies & Mass Finishing
The whole 3D printing workflow was on display in Boston at RAPID+TCT last week, from design software and 3D printing hardware all the way to post-processing and finishing solutions. For...
RAPID Roundup 2026: New Machines and Market Moves
RAPID + TCT 2026 wrapped up yesterday, but the show floor proved there’s a lot happening across the additive manufacturing (AM) space, especially when it comes to new hardware and...
trinckle’s Tool Design Software Lands in Stratasys GrabCAD Print
I’m a fan of trinckle, the German startup that offers super easy-to-use tools for creating customized jigs, fixtures, and other 3D printed products. With trinckle, it’s not just designers who...
Farsoon’s Fine Laser Spot 3D Printing Gives China a Thermal Management Edge
Metal additive manufacturing (AM) systems generally utilize lasers with spot sizes that fall into a range of 80 micrometers (μm) to 100μm, although dynamic beam shaping may soon lead to...













































