Russian Research Yields New Insight Into 3D Printed Titanium Implants for Mandibular Reconstruction
Russian researchers are experimenting with titanium implants meant to promote the reconstruction of the jaw after surgery, outlining their study in the recently published ‘Experimental Biointegration of a Titanium Implant in Delayed Mandibular Reconstruction.’
Surgery to remove an oral tumor usually also results in the need for mandibular reconstruction. And while implants are commonly required in reconstruction, the authors point out that not much is known about how bone integrates into a titanium implant, leaving them to examine the process further.
Unfortunately, surgery to remove cancer in the area of the jaw can be disfiguring, as well as making it difficult to chew. In reconstructing the area, surgeons are becoming more used to inserting titanium implants to replace tissue, beneficial due to its structure and biocompatibility.
Many methods revolve around grafting bone for replacing the deficiency in the mandibular area, whether including the use of an implant or not. Risks include resorption, challenges in rehab later, and delayed infection. There is also a common need for ‘secondary revisional procedures,’ which are obviously counterintuitive to the efficiency of what is initially assumed to be a one-time reconstruction.
As 3D printing becomes more accessible, affordable, and acceptable for use in the medical field, better options are becoming available for creating implants that can be customized completely to the patient, including those who are considered complex.
“The efficacy of mandibular reconstruction with direct implant prosthesis is a controversial topic, yet, in cancer patients with aggravating comorbidities, the best solution can be achieved by individually printed prosthetic mandibular implants,” explain the researchers. “The osseointegrative capabilities of modern porous titanium implants is high, and current technological manufacturing progress, including selective laser melting and 3D printing, has increased the interest of surgical teams in implant-based reconstruction.”
Undeniably, many questions remain around the topic of implant adaptation and the success of prostheses with additional implantation. The researchers delved further into the science of osseous integration with titanium implants in animals, post re-section, studying both the implanting and then the required removal of a prothesis meant to be temporary.
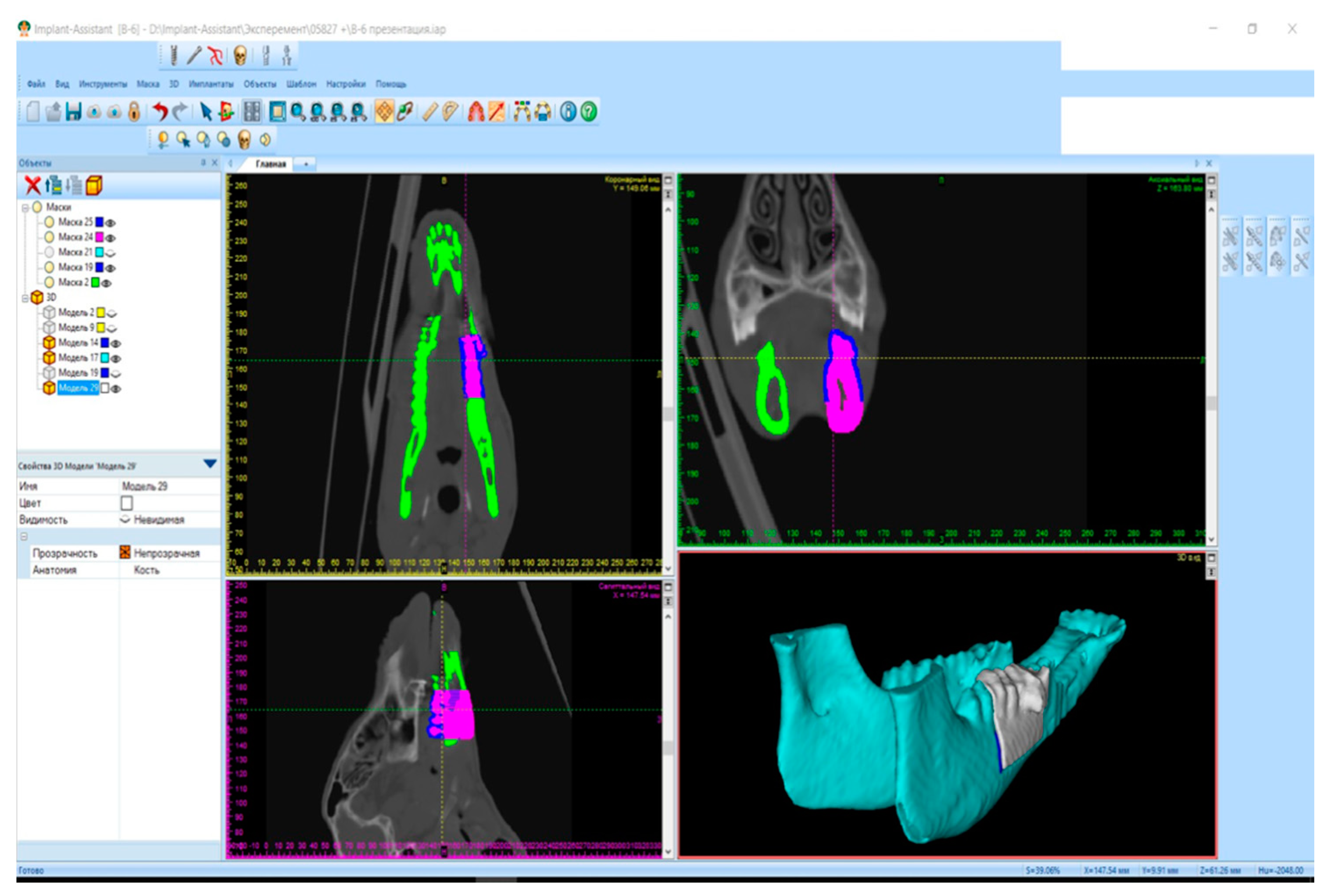
Titanium bionic implants, tetragonally shaped, were fabricated to mimic human bone. A Russian-made selective laser melting (SLM) printer was used with Titanium VT1-00 powder. For the experimental model, four adult ewes (from 1.5 to 2 years old) received implants in a fully approved research capacity.
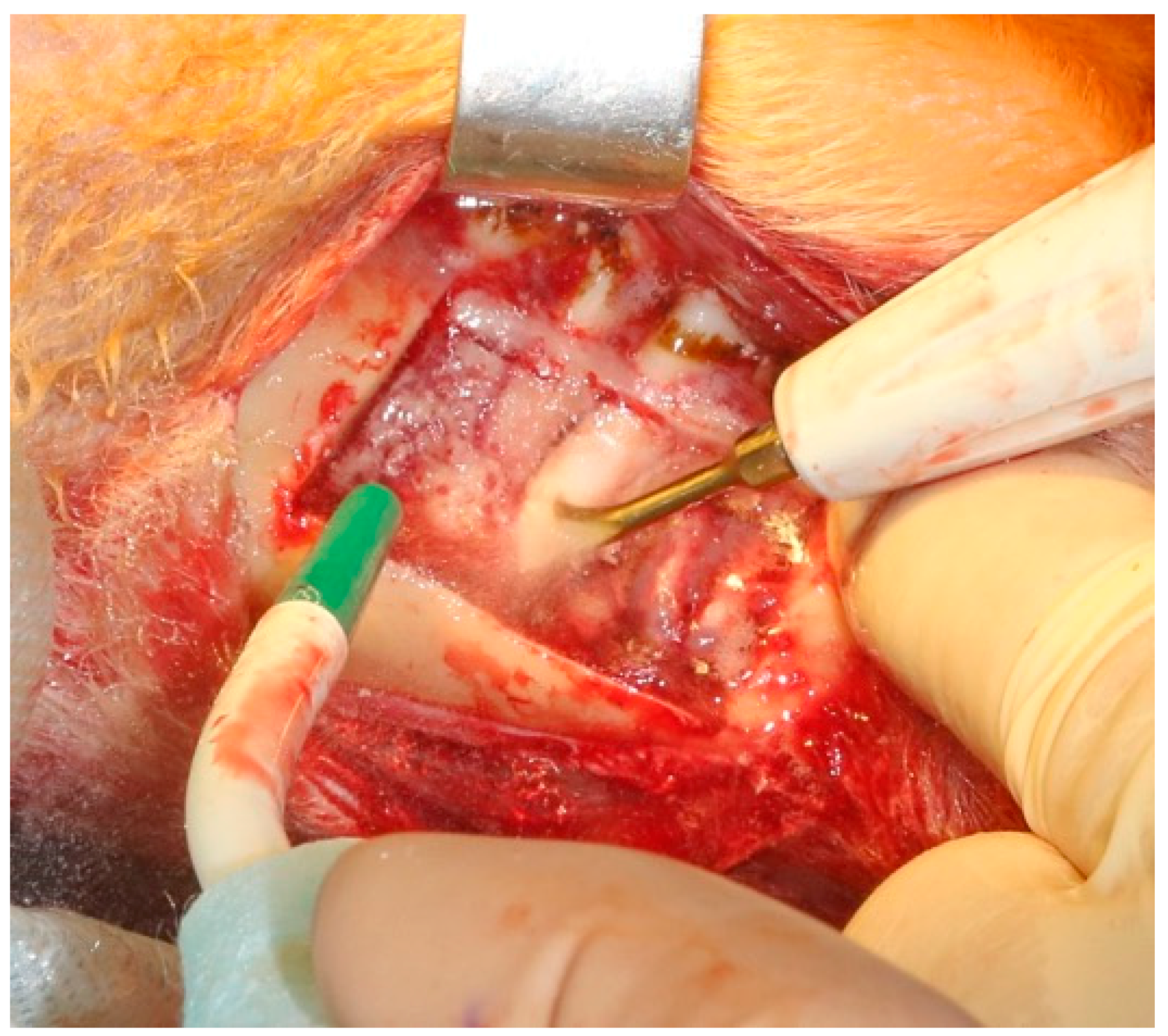
“The experiment protocol included the primary resection of the external cortical layer of the mandible at an extent of 3 cm, with consequent implantation of a sterilized plastic implant created via 3D printing,” stated the authors.
“A plastic implant was positioned into the mandibular defect and secured with standard orthopedic screws. Layered wound closure was performed with absorbable sutures. The skin was closed with non-absorbable material. This completed the first surgical stage of the experiment. As a result, all subjects received 3D modeled plastic implant for mandibular reconstruction.”
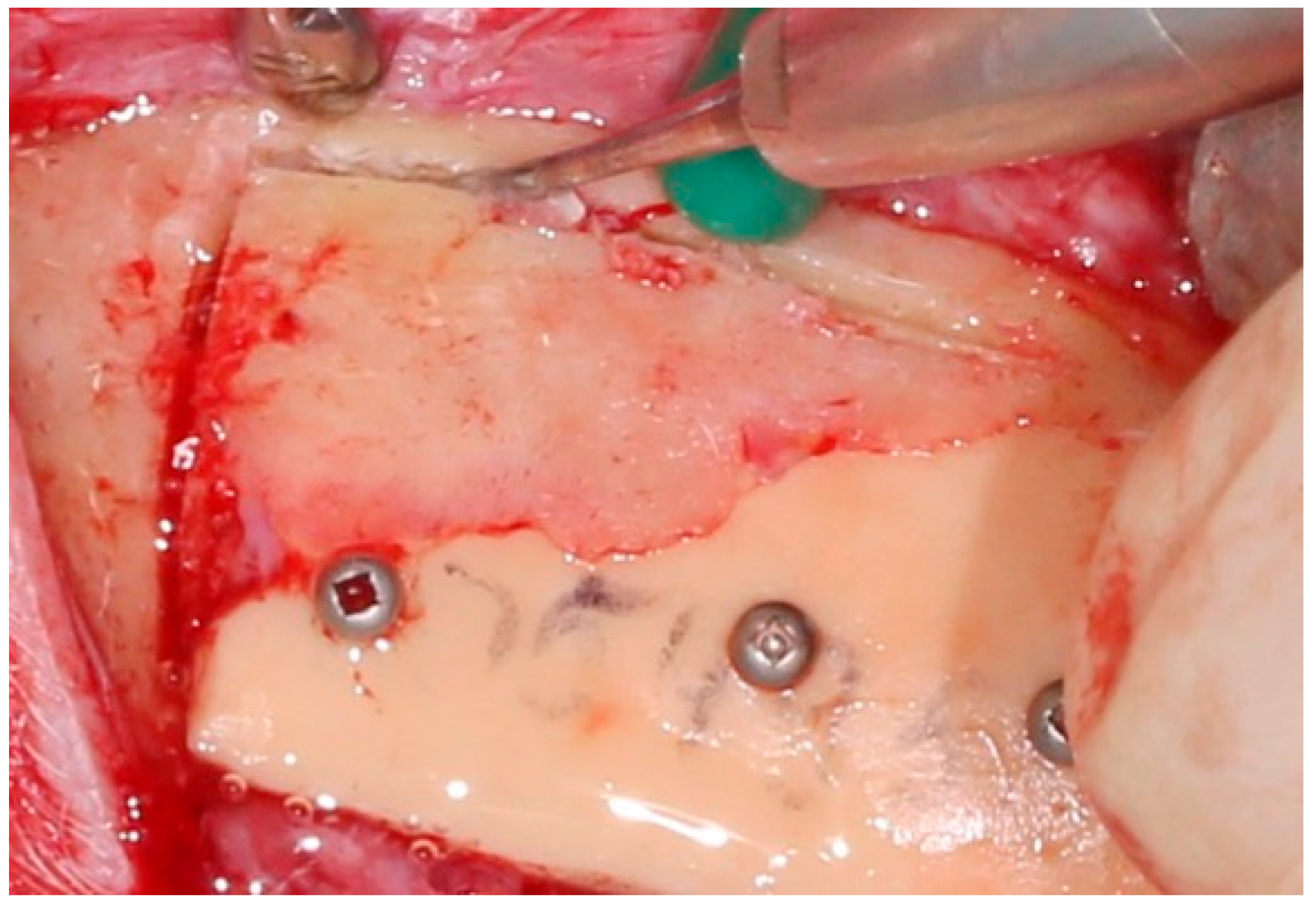
Each subject then also underwent secondary surgical intervention but at different times—specifically, one, three, six, and twelve months later, after which they received a patient-specific titanium implant.
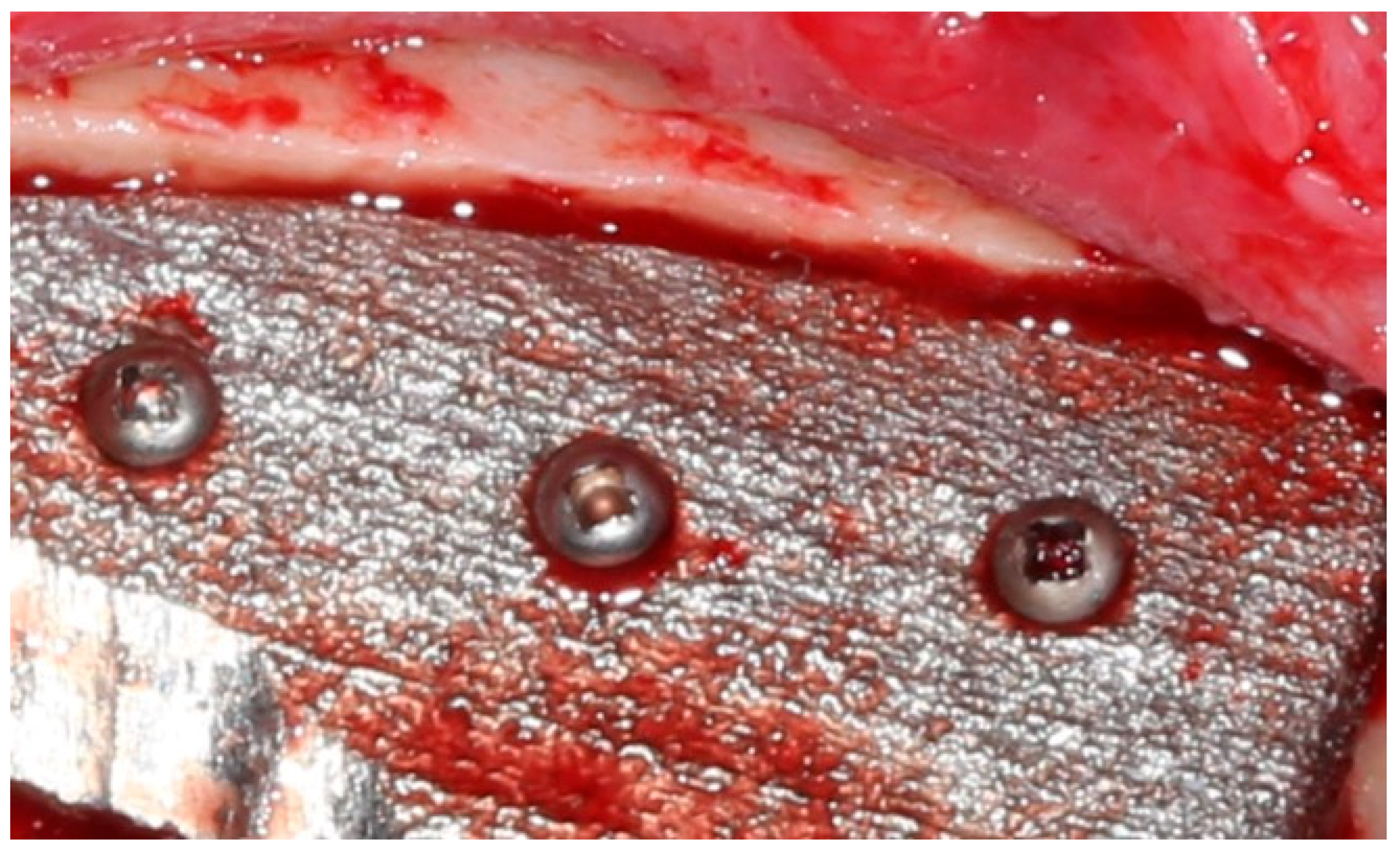
The researchers reported that it was ‘clearly established’ that the insertion of the implant led to tissue growth over the device, but with no inflammation detected.
“In all cases, the direct contact of osseous tissue with the titanium implant was established, which confirms the biointegration of the metal implant into the mandibular tissue. There were also areas of reorganization of osseous and soft tissue on the surface between the implant and bone with evidence of fibrous and bone integration into the implant.
“The authors conclude that the data obtained demonstrates that a porous titanium implant used in secondary surgical reconstruction provides significant osseous biointegration. This shows that it is possible and often advisable to postpone the implantation of a permanent implant in order to achieve better therapeutic results and account for possible complications after tumor resection.”
3D printing has played a role in numerous research projects focused on mandibular reconstruction as scientists fabricate innovative scaffolds, innovative methods for grafting, and 3D print other types of implants too.
What do you think of this news? Let us know your thoughts; join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
[Source / Images: ‘Experimental Biointegration of a Titanium Implant in Delayed Mandibular Reconstruction’]Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
Print Services
Upload your 3D Models and get them printed quickly and efficiently.
You May Also Like
AMPulse Asia: Creality IPO Headlines APAC 3D Printing Market Roundup
Asia’s additive manufacturing sector spent the back half of May moving capital and capacity, not just demos. Chinese desktop and consumer printer makers pushed onto public markets, metal powder producers...
Blue Origin’s New Glenn Explosion Comes During Major Manufacturing Push
Blue Origin‘s orbital New Glenn rocket exploded during a hot-fire test at Launch Complex 36 in Cape Canaveral on May 29, setting back the company’s launch ambitions at a time...
Aibuild Says New FETS Simulation Tool Is 10,000x Faster for AM
Aibuild has launched FETS for Additive Manufacturing, a Finite Element Thermomechanical Simulation tool that lets you simulate stress, distortion, thermal effects, and thermomechanical effects. The solution has been optimized for...
AI CAD Tools for 3D Printing: An Overview
There is a bevy of AI-to-CAD tools coming out. Some are finding users; some are raising millions in funding. Many new ones are coming out all the time, so we...