“Patient understanding of their diagnosis and treatment regimen is integral to individual compliance and satisfaction with their physician,” the researchers state. “Visual aids can be an important clinical tool for educating patients as they tend to understand and retain information more effectively with visual reinforcement. However, classical graphical aids, such as photographs or illustrations, often require patients to view a three-dimensional morphology in a two-dimensional representation. Patient comprehension can be especially difficult with regards to internal anatomic relationships such as the nasal sinus passages, as these are not commonly visualized systems. Poor comprehension can hinder the informed consent process and may result in the patient electing not to move forward with a beneficial and necessary procedure.”
According to the paper, which you can access here, ENT surgical cancellation rates are over 16%, but the researchers believe that 3D printed models may be a valuable tool for improving patient compliance and outcomes. To test this theory, they conducted a study involving 100 candidates for nasal or sinus surgeries. 50 of the patients were shown standard two-dimensional charts and diagrams while their doctors explained their conditions, and 50 were shown a 3D printed model generated from patient CT scans.
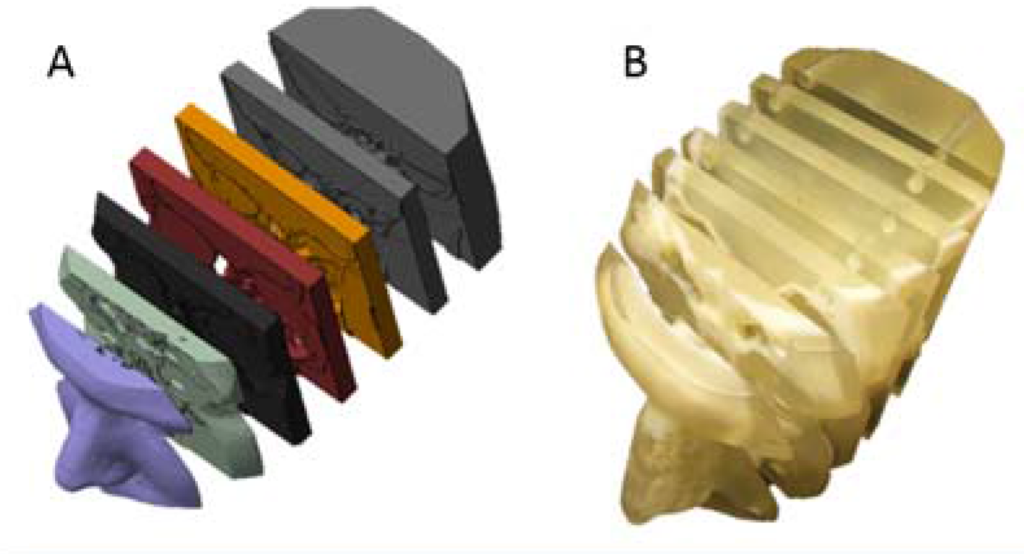
“The turbinates and nasal septum, soft nasal tissues, were accessible and easily manipulated by the ENTs to demonstrate physical manifestations of the patient’s disease state, altered air flow pathways, and proposed surgical treatments to the patients,” the researchers explain. “In this fashion, a single model was adaptable to describe the disease states of all individuals, preventing the need to create expensive, patient-specific repicas on a case-by-case basis.”
After their consultations with their ENT physicians, each patient was given a survey asking them to rate the physician’s explanation of the treatment plan, their own understanding of their anatomy and disease, and how much the educational tools – either the diagrams or the 3D printed model – helped in their understanding. They were also asked if the consultation eased their anxiety and if they planned to go through with the proposed treatment plan.
The results suggest that the researchers’ theory is correct. The average score for each survey question was higher for the group that received 3D printed models than it was for the group that did not. The scores were significantly higher in the 3D printed model group in regards to how they rated the quality of the physician’s explanation and their own understanding of their anatomy, disease, and the proposed surgical procedure.
“The largest increase in score was seen in patient understanding of the surgical treatment, which is the most critical information to ensure the patient is making an informed decision,” the researchers state.
“Overall, the survey results demonstrate the positive educational benefits of the 3D model as a clinical teaching tool for ENTs,” the researchers conclude. “…Future studies with larger cohorts in each group could help in distinguishing which increases are significant, and could also test each patient to objectively measure the understanding of their anatomy.”
The paper’s authors include Ian M. Sander, Taimi T. Liepert, Evan L. Doney, W. Matthew Leevy and Douglas R. Liepert. Discuss in the ENT forum at 3DPB.com.