 Bioprinting has proven to be useful for bone regeneration, as researchers learn to create more stable structures that mimic human tissue. In ‘Three-Dimensional Printed Polylactic Acid Scaffolds Promote Bonelike Matrix Deposition in Vitro,’ authors Rayan Fairag, Derek H. Rosenzweig, Jose L. Ramirez-Garcialuna, Michael H. Weber, and Lisbet Haglund explore the uses of desktop bioprinting with PLA.
Bioprinting has proven to be useful for bone regeneration, as researchers learn to create more stable structures that mimic human tissue. In ‘Three-Dimensional Printed Polylactic Acid Scaffolds Promote Bonelike Matrix Deposition in Vitro,’ authors Rayan Fairag, Derek H. Rosenzweig, Jose L. Ramirez-Garcialuna, Michael H. Weber, and Lisbet Haglund explore the uses of desktop bioprinting with PLA.
Even in conventional medicine today, surgeons find difficulty in repairing bones that have undergone trauma, whether due to an accident, tumor, or other serious issue. Grafting can still be challenging to complete, and then problematic later in terms of pain, infection, and the need for multiple procedures. Materials such as calcium phosphate bone cement (a synthetic graft) have become more popular for repairing bone defects, but there are also limitations due to lack of mechanical strength. While poly-cements have been used also, they can cause stress around the ‘target area,’ and lead to secondary fracture, which defeats the purpose of healing altogether.
Here, the researchers have investigated the use of tissue engineering for bone repair in growing cells, scaffolds, and using numerous bioactive factors. 3D printing has been successful in fabricating scaffolds using different polymers like PLA.
“The ideal material for scaffold development should fulfill specific criteria,” state the researchers. “The material must be biocompatible and must be capable of being generated with an interconnected network to mimic the natural tissue architecture.”
Cell sustainability is the greatest challenge, along with creating stable structures. The researchers sought to create scaffolds that would allow for complete cell sustainability, along with the best environment for encouraging tissue to form. They must also allow for the following:
- Fabrication in different, complex shapes
- Resistance to inflammation and toxicity
- Strong mechanical properties
- Appropriate porosity
- Affordability
In previous studies, the researchers were aware that PLA 3D printed from the desktop was suitable for both chondrocyte and nucleus pulposus tissue engineering applications. Here, they tested PLA scaffolds with pore sizes of 500, 750, and 1000 μm, fabricating accurate structures with good porosity; in fact, all scaffolds reflected pores in line with the initial designs, leaving the authors to conclude that this ‘suggested accuracy’ with desktop 3D printer—in this case, the Flashforge Creator Pro.
Pore size results were as follows:
- Small pore scaffolds – 585.61 μm ± 26.40
- Medium pore scaffolds – 769.94 μm ± 12.98
- Large pore scaffolds – 1028.85 μm ± 57.54, p < 0.0001
“The scaffold fabrication and replication process manifests high accuracy and precision as evidenced by μCT analysis, which proves the value of low-cost printing in tissue engineering applications,” stated the researchers.
The authors reported the following for mechanical properties:
“Significant differences in stiffness were observed between the three sizes (p < 0.05, p < 0.0001) in which Young’s modulus for the small pore size was 206.7 MPa ± 0.17 SD, medium size scaffold was 137.5 MPa ± 6.98 SD, and 116.4 MPa ± 5.97 SD for the large size PLA scaffold.”
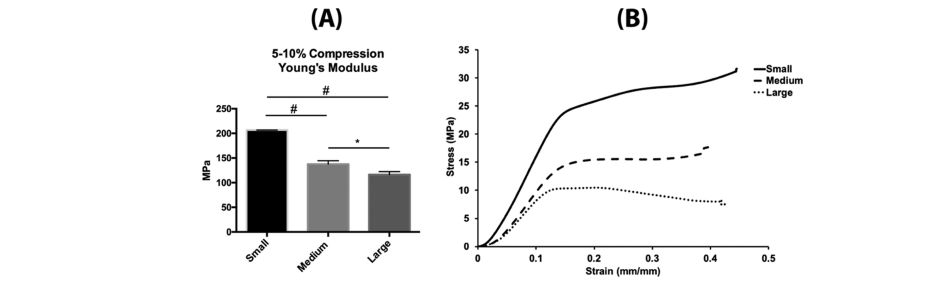
Mechanical properties of 3D-printed scaffolds. (A) Young’s modulus representing 5−10% compressive stress/strain curves of printed PLA scaffolds. For each set, (n = 3), error bars represent ±SD and (* = P value < 0.05), (# = P value < 0.0001). (B) Stress/strain curves of 500, 750, and 1000 μm showing the amount of deformation, elastic (proportionality) limit, and plastic region. For each set, (n = 3).
“The failure point of each scaffold was determined from the stress/strain curves in which the small-size failure point was around 21.63 MPa, around 11.86 MPa for the medium size, and around 8.53 MPa for the large-pore scaffold. Our results demonstrated an overall higher compressive modulus with smaller pores because of the addition of bulk material (smallest pore size has the highest amount of material and is the stiffest).”
The use of PLA was successful, indicating both accuracy and reproducibility, and the scaffolds presented properties like native bone. The authors stated that the data reflected structures stable enough for an environment recruiting host stem cells and repairing bone.
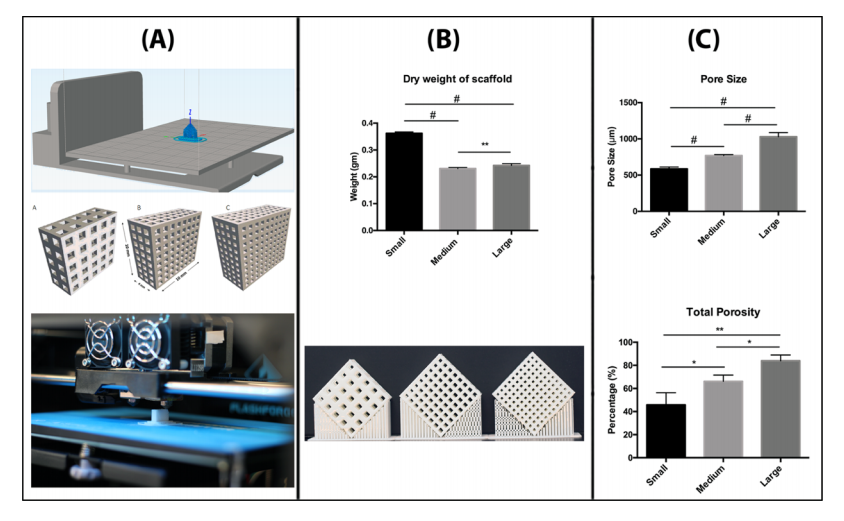
Morphological characterization of 3D printed scaffolds. (A) Representative images of the 3D models with dimensions and printing process. (B) Quantification of scaffold weight, (n = 6), error bars represent ±SD (** = P value < 0.005), (# = P value < 0.0001), with a representative image of printed scaffolds (Canon EOS 350d Camera). (C) Pore size was calculated by scanning electron microscopy, and porosity was determined by μ-CT. For each set, (n = 3), error bars represent ±SD and (* = P value < 0.05), (** = P value < 0.005), (# = P value < 0.0001).
“In vivo studies will be necessary to determine potential adverse effects, bone repair, and scaffold resorption rates,” stated the researchers. “It comes without surprise that 3D printing has been strongly adopted by orthopedic surgery clinical practice, medical education, patient education, and orthopedic-related basic science.
“Whereas 3D printing has been used for some time to generate patient models of defects for presurgical planning, there is a growing shift in using this technology in actual bone or tissue repair. One major focus in orthopedic and reconstructive surgery is to use 3D printed constructs for filling bone defects, substituting current standard therapies as an innovative approach for bone repair. Several studies have shown applicability and clinical relevance of using different types of 3D-printed polymers as a graft substitute.”
From 3D printing in hospitals to bioprinting in outer space and bringing forth materials which may eventually yield fabricated human organs, researchers are driven to create what used to be considered impossible, with a wide range of innovations already in use around the world. Find out more about desktop bioprinting here. What do you think of this news? Let us know your thoughts! Join the discussion of this and other 3D printing topics at 3DPrintBoard.com.
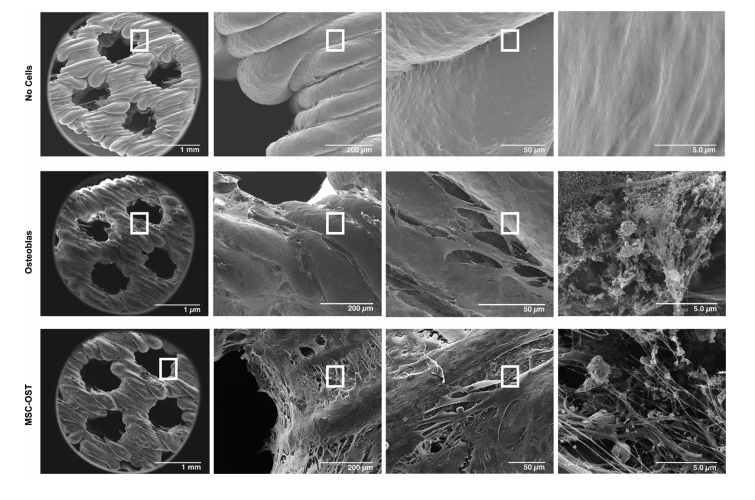
SEM of acellular and cell-seeded scaffolds. Representative SEM images of acellular, osteoblasts, MSC−OST seeded scaffolds at 80×,450×,1500×, and 22 000× magnifications and scale bars represent 1 mm, 200, 50, and 5 μm with the rectangular marker indicating the region of the scan (n = 3).
Subscribe to Our Email Newsletter
Stay up-to-date on all the latest news from the 3D printing industry and receive information and offers from third party vendors.
You May Also Like
Why Corrosive Resistant Materials Are Important to the Success of 3D Printing Across Industries
The adoption of additive manufacturing (AM) is accelerating across many major industries. As this technological shift unfolds, the importance of corrosion resistance has emerged as a challenge for 3D printing...
America Makes Announces IMPACT 2.0: $6.6M in New 3D Printing Funding
America Makes, the Manufacturing Innovation Institute (MII) based in Youngstown, Ohio, has announced IMPACT (Improvement in Manufacturing Productivity via Additive Capabilities and Techno-Economic Analysis) 2.0, a project call which will...
3D Printing Webinar and Event Roundup: April 14, 2024
We’re starting off the week’s 3D printing webinars and events at ASTM AMCOE’s 11th Snapshot Workshop and MACH Exhibition. Stratasys continues its advanced training courses, SME is holding a virtual...
AMUK Welcomes Airframe Designs as British 3D Printing Industry Grows
While the UK is not the hub for 3D printer and materials manufacturers as other nations, the country continues to excel at the research, development, and application of additive manufacturing...































